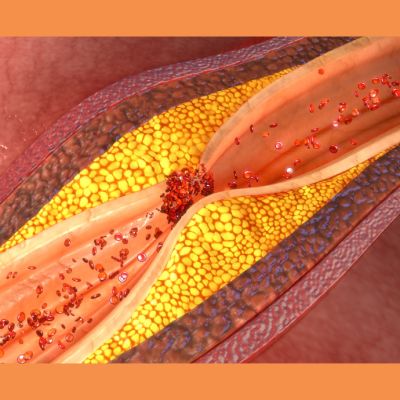
The absence of AAC is a predictor of no disease, just as the presence suggests obstructive CAD and all-cause mortality. In an analysis of noncontrast abdominal scans of 367 patients, AAC's ability to predict obstructive coronary disease had a sensitivity of 96 percent and a specificity of 31 percent, with positive and negative predictive values of 58 percent and 89 percent, respectively.
AAC scores proved to be significantly higher in patients with obstructive CAD, while at the other end of the AAC range, only seven of the 62 patients with an AAC score of zero showed obstructive CAD on the angiography. Specifically, increasing AAC was associated with increased mortality during univariate analysis, while multivariate analysis showed AAC adding incremental prognostic information over clinical variables, coronary anatomy and left ventricular function.
Scientists warned that their findings must be confirmed in larger group, including lower-risk patients, before AAC can be adopted as a method of risk stratification. However, they encourage recording the CT coronary calcium score if the scan had already been administered, as