HealthManagement, Volume 12 - Issue 2-3, 2012
Public health authorities face massive strain on their financial capacity and resources due to the explosion in the development of new medical technology, and the aging population. New reforms in legal initiatives prompted a radical change of the market structures which are being replicated in today’s health systems. The EU, for example, intends and has planned for some time, to reform previously monopolistic, traditional ways, because public services of general interest are more and more evolving into competitive structures. The establishment of health services as competitive structures will inevitably lead to a process of natural selection and only economically successful participants will survive to lead the healthcare market.
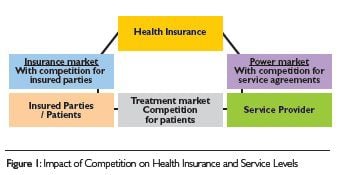
Competition in the healthcare market will impact both the health insurance and service levels (Figure 1). Consequently, there is a continuous need to increase effectiveness and efficiency, and thus to improve processes, in the healthcare sector generally and in the organisation of hospitals and medical practices in particular. The concept of competition in healthcare refers to both performance and cost competition, with a given emphasis on improved quality. “It is not the major players that will push the smaller ones out of the market, but the fast will push out the slow” (W. von Eiff, Medical Data Institute, Münster). Thus, the successful management of hospital departments and medical practices requires suitable structures and optimisation processes in the fields of medical quality, service quality and efficiency.
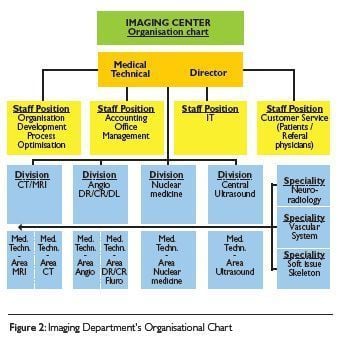
Organisational Structures in Brüderkrankenhaus Trier
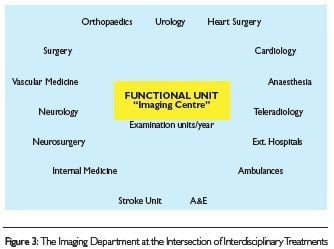
The Department for Radiology, Ultrasound and Nuclear Medicine in the Brüderkrankenhaus Trier has 69 employees, allocated as shown in Table 1.
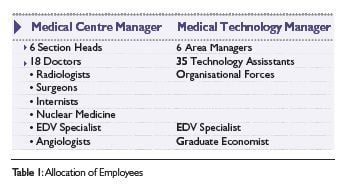
Medical imaging greatly influences the optimisation of the entire treatment pathway for patients in the hospital, as it plays a central part within the hospital, providing services to a large number of internal hospital departments as well as referring third parties (e.g. local practices). The imaging diagnostics and interventional treatment divisions are therefore particularly meaningful as service providers to all clinical departments of the hospital (Figure 3).
How Processes Impact Payment
It is essential that the organisation of the treatment process be viewed holistically, as a complete and entire process in order to execute a well-managed payment system. Along with the provision of individual services, interdisciplinary counselling must be provided prior to the diagnostic and treatment of disease patterns (e.g. vascular diseases), in particular in the context of medically and economically efficient diagnostic and treatment paths. Avoiding a CT examination through set treatment paths or interdisciplinary team meetings creates value both for the patient, potentially leading to less or no radiation exposure, and for the overall value creation chain of the hospital. In a system of diagnosis-based fixed reimbursement, the unperformed exam will be compensated in any case, while still respecting patient safety and a high medical quality.
How We Do It
Our department’s revenue streams include:
• outpatient services;
• Private patients;
• Internal activity allocation;
• External referrers; and
• Additional revenue from new offerings (Cardio-CT; screening, leasing of equipment and personnel from other health providers, increasing the number of private patients, etc.)
Increasing your service offering also generates new revenue when carried out in an efficient way. For us, our efficiency increased with the establishment of two ambulatory care centres. These systems allow for better utilisation, additional margins and the integration of ambulatory and stationary spheres, representing extension of the value chain. Cost savings are derived from the ratio of total costs to total revenues and internal transfer pricing. The positive difference between revenues and costs allows an increase in budget in the areas of personnel, equipment and investment.
Organisation of Our Budget
An interdisciplinary framework is not just useful for high quality medical treatment and process optimisation. In terms of budgetary planning, we carry out annual budget meetings that involve the administration personnel as well as the central management team, who create the frame for an overall targeted planning for the economic management of the medical imaging department (MID). This is subdivided into service area planning, cost planning and revenue planning. The parameters we use to measure the success of this plan include the service volume, which is rated by service points, and the cost of personnel and materials. Overall cost-effectiveness is the result of the relationship between revenues and costs.
Operational sector budgets set the targets for the upcoming year and are generally based on the data of the preceding year. The size of the service volume is determined to a high degree by the internal service allocation of the referring parties, who are responsible for the effectiveness of the service request but also for the involved prices. The MID's management is responsible for the productivity and the cost-effectiveness of the service provision (Figure 4).
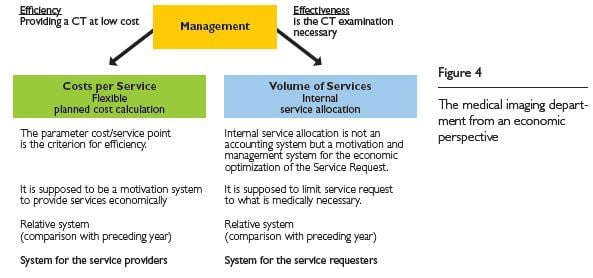
In this way, any deviations that arise between planning and execution becomes apparent and can be addressed by management. In the hospital, parameters offering service and cost information are particularly important in preparing the annual budget meetings between a department and the hospital management. Well-prepared target-oriented meetings, with a proper analysis of the service development and costs, can be crucial for the department’s future development.
In a monthly reporting of internal controlling, carried out in close coordination with the department of business administration, the data is provided to the responsible managers of the relevant cost centres in the MID. Budgets consist of both a value based cost component (input) and volume based services (output).
Cost adjustments in personnel and material costs are made using a flexible planned cost calculation that takes any resulting potential higher or lower revenue into account. For example, productivity increases in the form of more services at lower costs are rewarded by a bonus for the medical imaging department’s employees. In case of a productivity increase, this will be negotiated as planned/target parameter for the next year, so that the efficiency criterion is continually driven upwards (Figure 5).
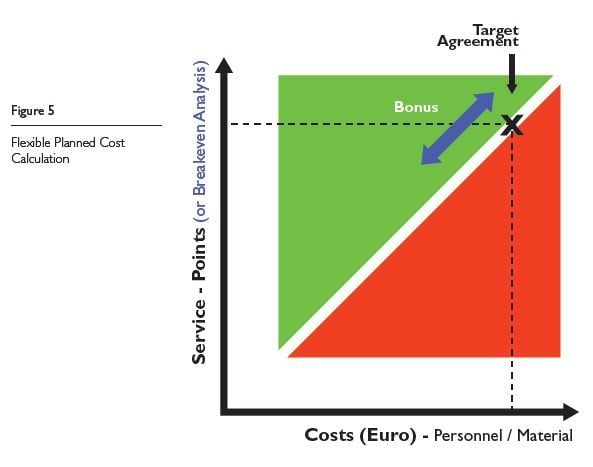
When Does Fee-for-Service Work?
By setting up a budgetary management system that operates under the umbrella of optimised efficiency, a hospital or medical practice is better equipped to survive and will add some protection in the face of challenging or changing financial conditions. In a hospital, efficiency, which in this case refers to the relationship between revenue and costs, refers to the sum of individual services (e.g. out-patient services, emergencies), but beyond this also to the realisation of treatment complexes – diagnosis related groups (DRG). Approximately 70 – 80 percent of the revenue of hospitals consists of diagnosis-based fixed compensation. The DRG system is a service-based compensation scheme that follows the motto “fee for service”. A comparison of the annual volume of personnel and material costs with the sum of the corresponding DRG portions can be used as a criterion of efficiency. This applies especially to the personnel costs, which represent the largest cost pool.
Benchmarking Costs and Services
In order to evaluate the results of productivity external hospitals are used as comparators (external benchmarking). This way, costs for personnel and material may be compared e.g. with the cost data of the DRG calculation, and analysed (Figure 6).
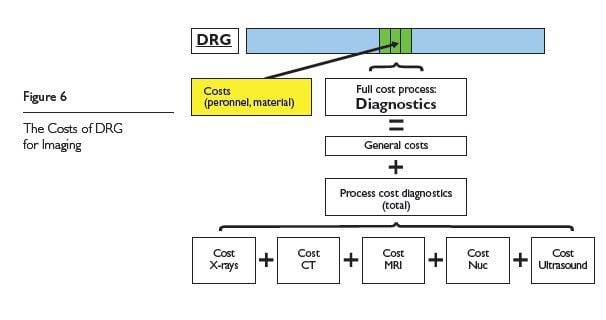
Revenue, the process sequence and the type and number of the procedures used must be compared and reviewed for optimisation needs. The same applies to service data, the comparison of which allows for the deriving of effectiveness assessments. How the examination mix in a complex diagnosis-based, fixed compensation case (e.g. B70B, stroke) looks in retrospective comparison with other hospitals is shown in Table 2.
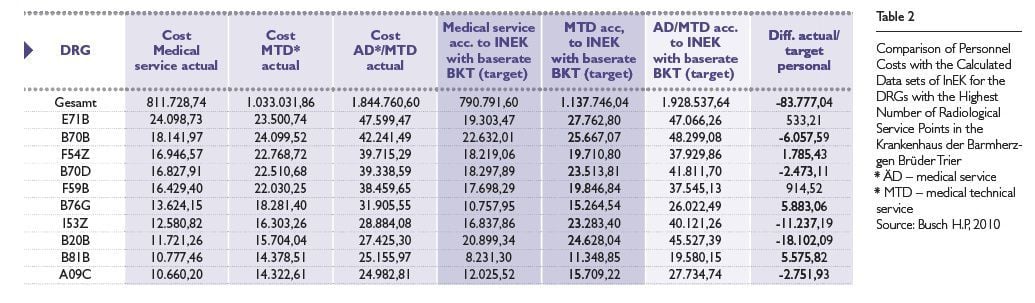
Benchmarking against the procedures used on average in the German Institute for the Compensation System in Hospitals (InEK) calculation shows the possible optimisation need of the clinical treatment path.
Further, utilisation management within the scope of external benchmarking against 500 hospitals in Europe (Philips Utilization Services) enables the assessment of the quality of the process workflow based on the criteria of patient flow management, examination flow management, schedule logistics management, optimisation of the procedures.
Process Optimisation
The optimisation of the organisational structure has a direct impact on the value chain of medical imaging departments. In the DRG context, the entire treatment path in the hospital is compensated, so that a continuous optimisation of processes in the areas of medical quality, service quality and efficiency is necessary to secure revenue. (See Zapp, W./Dorenkamp, A. (2002), page 65). On these three pillars, the centre must be managed according to the rules of a business enterprise.
Diagnosis based fixed compensation (the price is a “Date”) requires an optimisation in the areas of effectiveness (i.e, looking at whether the indication and/or the MR examination was necessary) and efficiency (i.e, analysing the way in which the examination was conducted). In this context, productivity (costs per examination) must be used as criterion of success. Further, it is necessary to use resources where they are needed the most according to the rationality principle.
The difference between the revenue determined by the DRG compensation and the costs can be enlarged by the increase of productivity and the avoidance of unnecessarry examination numbers. New equipment (e.g. 3-Tesla MRT, flat plate detectors) afford the possibility to increase patient throughput.
The economic success of the MID requires continuous efforts in order to be able to succeed in the areas of medical quality, service quality and efficiency.
References:
For references please send a request to






