Atrial fibrillation (AF) is the most common heartbeat irregularity and associated with development of stroke, myocardial infarction and heart failure. Vice versa, the structural and neurohormonal changes in heart failure (HF), when the contractility of the heart muscle is reduced, make the development and progression of AF much more likely. HF itself increases the risk of AF 4.5- to 5.9-fold.
Regardless which comes first, the combination of HF and AF is associated with a worse prognosis, repeated and prolonged hospital stays as well as higher hospital costs.
In an analysis of 10,701 hospitalized patients diagnosed with HF, patients who developed new-onset AF had longer in-hospital stays, higher morbidity, and a trend towards increased mortality.
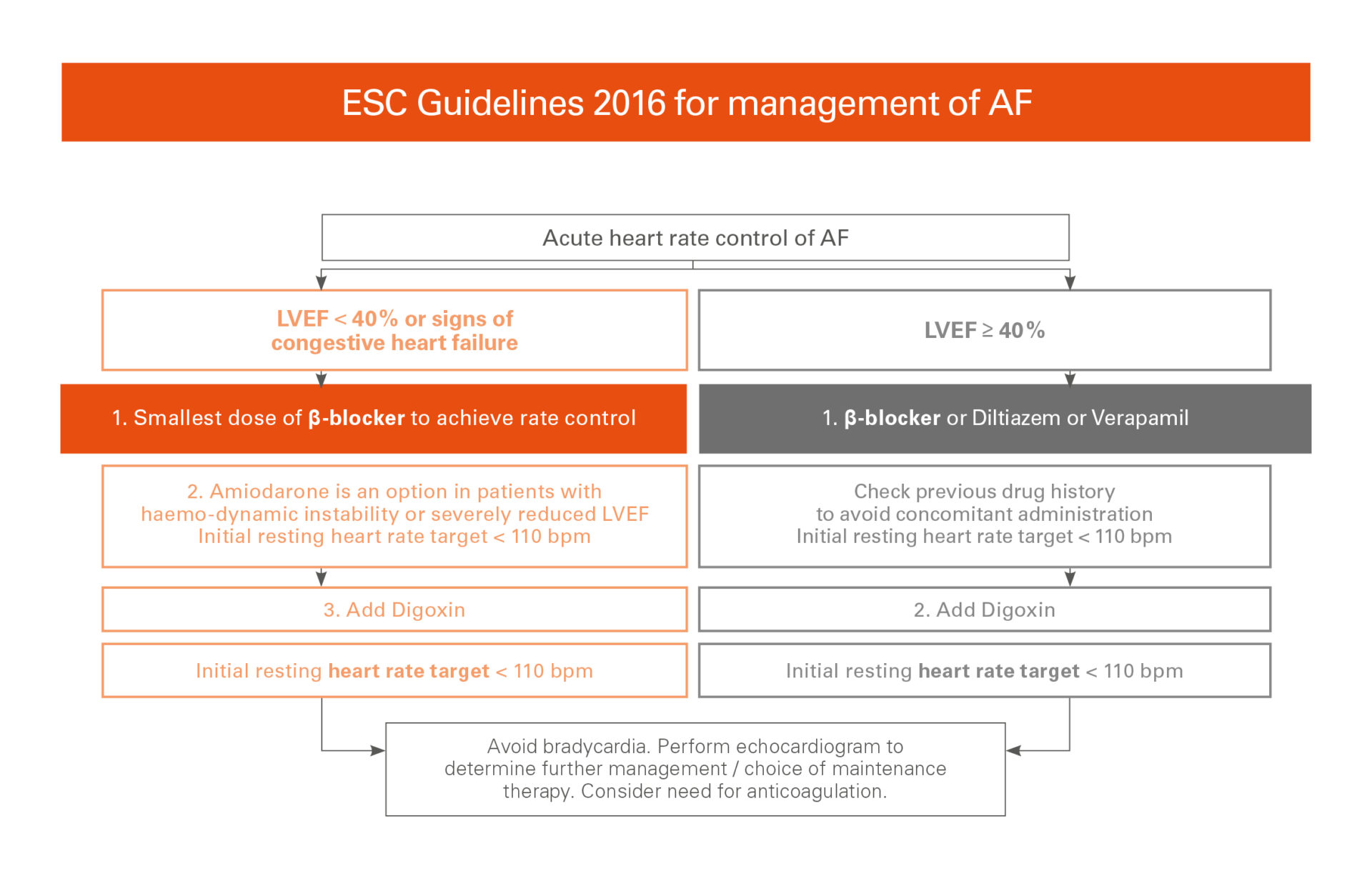
In acute management of AF with concurrent HF, it is important to quickly manage heart rate control as a first approach. The primary goal is to reduce the heart rate below 110 beats per minute to facilitate ventricular filling and improve cardiac work (CO). The current guidelines strongly recommend beta-blockers in clinically stable patients with heart failure and reduced ejection fraction – HFrEF (class I, level of evidence A) for controlling the heart rate.
In a subgroup analysis of AF-CHF-trial, beta blockers were shown to decrease all-cause mortality by 28% in patients with HFrEF and AF. The effect was more pronounced in individuals with higher AF burden. In addition, a better NYHA stage was achieved in many patients.
In the future, ultra-rapid acting intravenous beta-blockers could close the therapeutic gap for precise and individual control of heart rate, when reduction of heart contractility is undesirable in heart failure patients. AMOMED is supporting research projects in critical care setting to develop better therapeutic options for new onset of atrial fibrillation, especially in patients with heart failure.