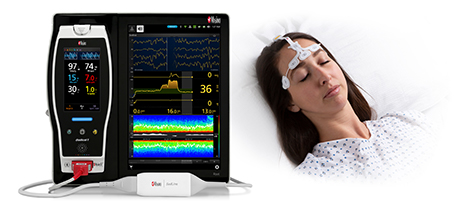
Masimo SedLine® Brain Function Monitoring with PSi Processed EEG Helped Identify the Oversedations
Masimo today announced that in a new study published in Anesthesia Research and Practice, researchers used Masimo SedLine® Brain Function Monitoring to investigate the depth of anesthesia of patients receiving propofol for outpatient colonoscopy, concluding that, "Although providers planned for moderate to deep sedation, processed EEG [electroencephalography] showed patients were under general anesthesia, often with burst suppression. Anesthesiologists and endoscopists may utilize processed EEG to recognize their institutional practice patterns of procedural sedation with propofol and improve upon it."1
Masimo SedLine® Brain Function Monitoring |
Noting that depth of sedation is "rarely quantified," but that "the spectrum of sedation actually attained in gastrointestinal endoscopy procedures may extend to levels deeper than planned for, thereby exposing patients to…cardiorespiratory risks," Dr. Jamie Bloom and colleagues at Thomas Jefferson University Hospital in Philadelphia sought to understand how frequently patients whose procedures called for moderate to deep sedation using propofol actually experience unintended general anesthesia and burst suppression. To quantify this, they monitored 119 adult patients undergoing outpatient colonoscopies using Masimo SedLine brain function monitoring, including its processed EEG index, the Patient State Index (PSi). PSi provides values that range from 0 to 100, with higher values indicating lesser degrees of sedation (with values from 50 to 25 indicative of general anesthesia, and below 25 for burst suppression). For the study, PSi values correlating to general anesthesia and burst suppression were confirmed by examination of the raw EEG by a neurointensivist and a neurophysiologist.
The researchers found that 118 of the 119 (99.1%) patients attained PSi values of <50, consistent with general anesthesia, and that these patients spent a significantly greater percentage of the procedure with PSi values <50 (53.1% of the time) vs. >50 (42% of the time) (p = 0.001). Of the 118 patients, 33 (27.7%) attained PSi values of <25, consistent with burst suppression. In addition, the researchers found the mean total dose of propofol was significantly correlated with PSi during periods of PSi values <25 (R = 0.406, p = 0.021).
Based on the study results, the researchers concluded, "The depth of sedation achieved with anesthesia administered propofol for colonoscopy spans a continuum. Although providers planned for moderate to deep sedation, processed EEG in this study revealed a substantially greater depth consistent with general anesthesia and even burst suppression."
They continued, "Feedback from devices such as employed in this study to guide the depth of sedation may be considered to not only raise awareness of the physiologic implications of deeper levels of sedation but also to optimize institutional sedation practice. Further research is required to establish the impact on patient outcomes of anesthetic practices resulting in intraprocedural burst suppression."
Patients receiving anesthesia during surgery can be over- or undersedated, both of which carry risks. When under-anesthetized, patients may have awareness during the procedure, which can be traumatic; when they are over-anesthetized, they may have alternating periods of no brain activity as measured by EEG, which is referred to as burst suppression.2 Burst suppression has been correlated with increased risk of postoperative delirium,3 which in turn has been shown to increase hospital length of stay and readmission rates, thus increasing costs.4 Burst suppression has also been associated with postoperative trauma, dementia, decreased quality of life, additional healthcare costs, and even death.3 In addition to burst suppression, overly deep sedation may result in loss of spontaneous ventilation and impaired cardiovascular function.1 Oversedation has also been associated with longer time on mechanical ventilation, longer time in the ICU, greater need for radiological evaluation of mental status, and a higher probability of developing brain dysfunction.2
The role of anesthesiologists in keeping patients appropriately sedated, and not over- or under-sedated, is critically important. Masimo SedLine has been shown to help anesthesiologists understand the patient’s sedation state using not only PSi values, but also through interpretation of the raw EEG and the Density Spectral Array that SedLine provides.4-6 In the current study, researchers showed that even in outpatient procedures, like colonoscopy, there is still a risk of patients being over-anesthetized, leading to burst suppression, which was identified using the PSi available as part of Masimo SedLine brain function monitoring.1