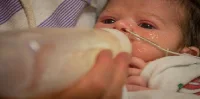
Although enteral nutrition (EN) or the feeding of patients through a tube is a common practice in an intensive care unit, the problem of underfeeding remains. A usual practice is to have a certain amount of feeding per hour but this is often interrupted by procedures, tests, or emergencies.
A better way to reduce underfeeding in ICU patients is to have a volume-based system that sets a nutrition volume per day, according to findings of a quality improvement audit which appears in Nutrition in Clinical Practice. The journal is published by the American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.).
The audit included a review of ICU patients under mechanical ventilation in a hospital in St. Louis, Missouri. It found that the patients' EN volume intake was at 37 percent, well below the normal standard of 80 percent. The study patients were then placed on a volume-based system called the FEED ME (Feed Early Enteral Diet adequately for Maximum Effect) protocol. Results from both patient pools were analysed.
The EN volume and calories delivered through FEED ME were much higher than the prior practice, according to the reviewers, as were grams of protein and increase in body weight for patients. Moreover, only a slight increase in diarrhoea was observed.
The audit results show that a volume-based approach to EN could improve nutrition and healthcare outcomes for ICU patients. However, the investigators would like to see further audits conducted to ensure compliance, effectiveness and safety of the volume-based system. Additional studies could also be useful in finding ways to improve the protocol as needed, the researchers said.
Nutrition Support Protocols
The audit results support the views expressed in an article published in the August issue of Critical Care Nurse (CCN). "Interruptions in Enteral Nutrition Delivery in Critically Ill Patients and Recommendations for Clinical Practice" offers specific strategies to combat the problem of underfeeding and decrease the time patients spend without nutrition.
"Malnutrition is common in critically ill patients, and the use of a nutrition support protocol can help improve patients' outcomes," writes Melissa L. Stewart, RN, DNP, MSN, CCNS, CCRN, a staff nurse in the medical ICU at the University of Kentucky Chandler Medical Center in Lexington.
The article supports the development and use of nutrition support protocols to offer guidance to bedside nurses when addressing issues related to enteral feedings, including initiation of feedings and feeding intolerance, as well as advancement and discontinuation of enteral nutrition.
Protocols can help increase the amount of nutrients provided to critically ill patients and decrease the amount of time necessary to reach target nutrition goals, according to the CCN article.
Other evidence-based strategies for treating or preventing malnutrition include: head of bed positioning, postpyloric feeding access, use of prokinetic medications, and use of a higher threshold when monitoring gastric residual volumes.
Source: ScienceDaily.com
Image Credit: Wikipedia
A better way to reduce underfeeding in ICU patients is to have a volume-based system that sets a nutrition volume per day, according to findings of a quality improvement audit which appears in Nutrition in Clinical Practice. The journal is published by the American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.).
The audit included a review of ICU patients under mechanical ventilation in a hospital in St. Louis, Missouri. It found that the patients' EN volume intake was at 37 percent, well below the normal standard of 80 percent. The study patients were then placed on a volume-based system called the FEED ME (Feed Early Enteral Diet adequately for Maximum Effect) protocol. Results from both patient pools were analysed.
The EN volume and calories delivered through FEED ME were much higher than the prior practice, according to the reviewers, as were grams of protein and increase in body weight for patients. Moreover, only a slight increase in diarrhoea was observed.
The audit results show that a volume-based approach to EN could improve nutrition and healthcare outcomes for ICU patients. However, the investigators would like to see further audits conducted to ensure compliance, effectiveness and safety of the volume-based system. Additional studies could also be useful in finding ways to improve the protocol as needed, the researchers said.
Nutrition Support Protocols
The audit results support the views expressed in an article published in the August issue of Critical Care Nurse (CCN). "Interruptions in Enteral Nutrition Delivery in Critically Ill Patients and Recommendations for Clinical Practice" offers specific strategies to combat the problem of underfeeding and decrease the time patients spend without nutrition.
"Malnutrition is common in critically ill patients, and the use of a nutrition support protocol can help improve patients' outcomes," writes Melissa L. Stewart, RN, DNP, MSN, CCNS, CCRN, a staff nurse in the medical ICU at the University of Kentucky Chandler Medical Center in Lexington.
The article supports the development and use of nutrition support protocols to offer guidance to bedside nurses when addressing issues related to enteral feedings, including initiation of feedings and feeding intolerance, as well as advancement and discontinuation of enteral nutrition.
Protocols can help increase the amount of nutrients provided to critically ill patients and decrease the amount of time necessary to reach target nutrition goals, according to the CCN article.
Other evidence-based strategies for treating or preventing malnutrition include: head of bed positioning, postpyloric feeding access, use of prokinetic medications, and use of a higher threshold when monitoring gastric residual volumes.
Source: ScienceDaily.com
Image Credit: Wikipedia
Latest Articles
malnutrition, enteral nutrition, underfeeding
Although enteral nutrition (EN) or the feeding of patients through a tube is a common practice in an intensive care unit, the problem of underfeeding remai...