New guidelines published in the British Journal of Anaesthesia describe a comprehensive strategy to optimise oxygenation, airway management, and tracheal intubation in critically ill patients, in all hospital locations. These guidelines were formulated by a panel of experts assembled by the Difficult Airway Society (DAS) of the UK, together with Intensive Care Society, Faculty of Intensive Care Medicine, and Royal College of Anaesthetists.
The guidelines recognise that closer attention to human factors, rather than simply introduction of new devices or improved technical proficiency, is required to improve outcomes of airway management in critically ill patients.
"In the critically ill, patient factors may preclude standard airway assessment. Urgency and reduced physiological reserve contribute dramatically to increased risks of profound peri-intubation hypoxaemia, hypotension, arrhythmia, cardiac arrest, and death. Delays during tracheal intubation and multiple attempts at laryngoscopy are associated with increased complications, again including cardiac arrest and death," according to the panel.
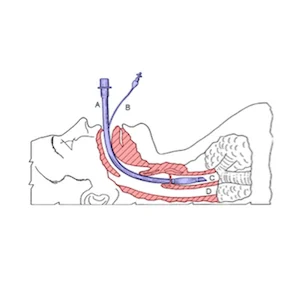
To address these challenges, the guidelines emphasise the role of the airway team, a shared mental model, planning, and communication throughout airway management. The primacy of oxygenation including pre- and peroxygenation is highlighted. A modified rapid sequence approach is recommended.
To avoid delays and task fixation, the guidelines recommend assembly of a team with a team leader who remains "hands free" to maintain situation awareness. The guidelines also recommend early use of a videolaryngoscope, with a screen visible to all, and second generation supraglottic airways for airway rescue.
In addition, the new guidelines recommend the "Vortex approach", attempting insertion of a supraglottic airway device interspersed with attempted facemask ventilation. Recommendations for emergency front of neck airway (FONA) are for a scalpel–bougie–tube technique while acknowledging the value of other techniques performed by trained experts. As most critical care airway catastrophes occur after intubation, from dislodged or blocked tubes, essential methods to avoid these complications are also emphasised.
In an accompanying editorial, Takashi Asai, MD, PhD, Department of Anaesthesiology, Dokkyo Medical University Saitama Medical Centre, Koshigaya, Japan, emphasises the need for more effective strategies for airway management in critically ill patients.
"Airway management is required not only in patients undergoing anaesthesia in operating rooms, but also in critically ill patients outside operating rooms (such as intensive care units, on the ward, or in emergency departments). Nevertheless, it seems that less effort has been taken to minimise problems associated with airway management in critically ill patients, in particular for patients on the ward," Dr. Asai writes.
The new guidelines published by DAS, Dr. Asai says, clearly highlight current problems and provide comprehensive strategies to minimise these problems. "It is our task to introduce appropriate strategies for airway management, establish training systems, and carry out necessary studies to minimise risk in airway management of critically ill patients," he adds.
Source: British Journal of Anaesthesia
Image Credit: Wikimeda Commons
References:
Higgs A et al. on behalf of Difficult Airway Society, Intensive Care Society, Faculty of Intensive Care Medicine, Royal College of Anaesthetists (2018) Guidelines for the management of tracheal intubation in critically ill adults. Br J Anesth. 120(2):323-352, doi: 10.1016/j.bja.2017.10.021
Asai T (2018) Airway management inside and outside operating rooms -- circumstances are quite different. Br J Anesth. 120(2):207-209, doi: 10.1016/j.bja.2017.10.014
Asai T (2018) Airway management inside and outside operating rooms -- circumstances are quite different. Br J Anesth. 120(2):207-209, doi: 10.1016/j.bja.2017.10.014
Latest Articles
Critical Care, oxygenation, airway management , Tracheal intubation
New guidelines published in the British Journal of Anaesthesia describe a comprehensive strategy to optimise oxygenation, airway management, and tracheal intubation in critically ill patients, in all hospital locations. These guidelines were formulated by