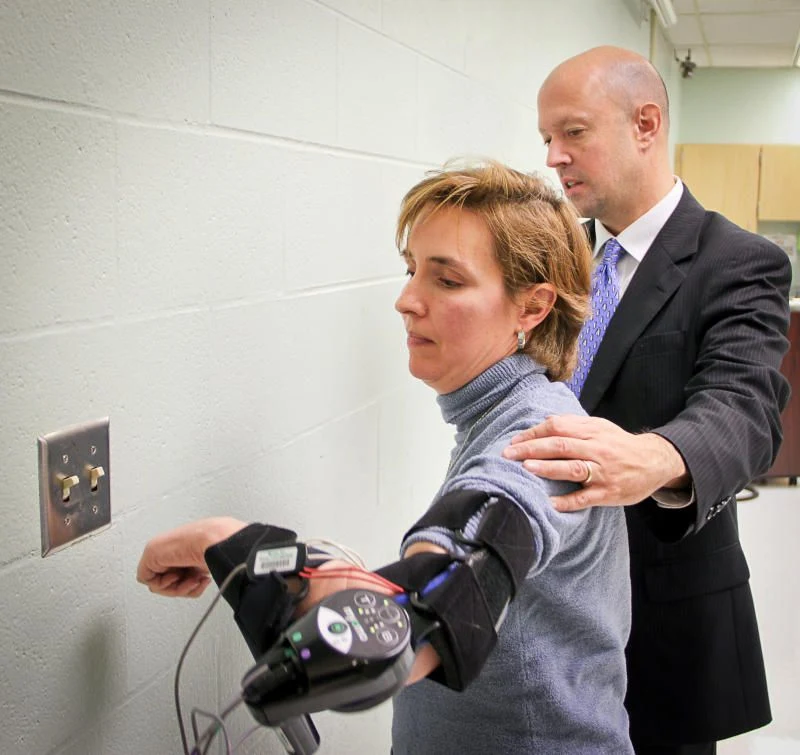
Patient in rehab with device. (Credit: Image courtesy of Ohio State University Wexner Medical Center)
Stroke survivors left weakened or partially paralyzed may be able to regain more arm and hand movement than their doctors realize, say experts at The Ohio State University Wexner Medical Center who have just published two new studies evaluating stroke outcomes.
One study analyzed the correlation between long-term arm impairment after stroke and the size of brain lesions caused by patients’ strokes – a visual measure often used by doctors to determine rehabilitation therapy type and duration. The other study compared the efficacy of a portable robotics-assisted therapy program with a traditional program to improve arm function in patients who had experienced a stroke as long as six years ago.
“These studies were looking at two entirely different aspects of a stroke, yet they both suggest that stroke patients can indeed regain function years and years after the initial event,” said Stephen Page, PhD, OTR/L, author of both studies and associate professor of Health and Rehabilitation Sciences in Ohio State’s College of Medicine. “Unfortunately, we know that this is not a message that many patients and especially their clinicians may be getting, so the patients may not be reaching their true potential for recovery.”
Size doesn’t matter
Clinicians frequently tell patients that the bigger the size of the area of their brains affected by their strokes, the worse that their outcomes will be. However, in a lead article in the Archives of Physical Medicine and Rehabilitation, Page’s research team found that there was no relationship between the size of stroke lesions and recovery of arm function in 139 stroke survivors. On average, study participants had experienced a stroke five years earlier.
“Historically, lesion size been thought to influence recovery, but we didn’t find that to be the case when looking at regaining arm and hand movement,” said Page, who also runs Ohio State’s B.R.A.I.N Lab, a research group dedicated to developing approaches to restore function after disabling injuries and diseases. “This has important implications because we know clinicians look closely at lesion volume and may make decisions about the type and duration of therapy, and that some may communicate likelihood for recovery to patients based on this size. Many people think the window for therapy is roughly six months, but we think it’s much longer.”
Page agrees that the first six months after a stroke may represent important healing time for the brain, but that “retraining” it with occupational therapy can potentially be helpful at any time after the stroke. He says that his findings support other theories that the health of remaining brain tissue influences recovery much more than lesion size.
Although there are many studies that have identified a relationship between stroke lesion size and overall neurological function, Page’s study is the first to specifically look at lesion size and upper extremity outcomes.
Robotic arm as good as traditional therapy
In the second study, Page’s team demonstrated that stroke survivors using a portable robotic-assisted arm to perform repetitive task training showed as much motor recovery as patients who performed similar tasks in a therapist-guided outpatient setting.
“Our results are exciting not just because we showed robotics-assisted therapy can offer equal benefit. We showed that both groups got better, even among patients who had suffered strokes as long as eight years ago,” noted Page.
For the study, which was published in the June 2013 issue of Clinical Rehabilitation, patients performed repetitive exercises that focused on everyday tasks while supervised by a therapist in an outpatient setting. Half of the group was randomly assigned to use the robotic arm, a portable device that is worn over the arm like a brace. When a person tries to move a weakened arm, the device senses the electrical impulses and helps the person carry out the movement. A second group performed the same tasks without the device for the same amount of time and in the same environment. The group training with the robotic arm performed tasks as well as their counterparts.
“Therapy can be tiring, expensive, and resource-intensive. This study is important because it shows us that in patients with moderate arm impairment, similar benefits can be derived from using a robotic device to aid with arm therapy as with manually based rehabilitative approaches,” said Page. “Study participants who trained with the robotic arm also reported feeling stronger and more positive about the rehabilitation process.”
Most of the estimated 80 million stroke survivors worldwide will continue to have upper body weakness for months after a stroke, preventing them from accomplishing everyday tasks like lifting a laundry basket or drinking from a cup. Page says that more research in stroke outcomes and rehabilitation is needed, and that he hopes families and healthcare practitioners dealing with stroke will keep the door to recovery open wider and longer.
“Loss of upper extremity movement remains one of the most common and devastating stroke-induced impairments. And the fact is that more stroke survivors are expected yet studies and pathways to optimize rehabilitative therapy for these millions are not always emphasized. In particular, we know active rehabilitation programs help people regain function, but we still don’t know who will benefit the most from these types of therapy,” said Page. “Both of these studies give us insights about patients who will respond best – and most importantly, that we have to give these patients every chance possible to get better, because they can keep getting better.”
Click here to see video of a stroke survivor using the bionic arm.
Source: The Ohio State University Wexner Medical Center
Stroke survivors left weakened or partially paralyzed may be able to regain more arm and hand movement than their doctors realize, say experts at The Ohio State University Wexner Medical Center who have just published two new studies evaluating stroke outcomes.
One study analyzed the correlation between long-term arm impairment after stroke and the size of brain lesions caused by patients’ strokes – a visual measure often used by doctors to determine rehabilitation therapy type and duration. The other study compared the efficacy of a portable robotics-assisted therapy program with a traditional program to improve arm function in patients who had experienced a stroke as long as six years ago.
“These studies were looking at two entirely different aspects of a stroke, yet they both suggest that stroke patients can indeed regain function years and years after the initial event,” said Stephen Page, PhD, OTR/L, author of both studies and associate professor of Health and Rehabilitation Sciences in Ohio State’s College of Medicine. “Unfortunately, we know that this is not a message that many patients and especially their clinicians may be getting, so the patients may not be reaching their true potential for recovery.”
Size doesn’t matter
Clinicians frequently tell patients that the bigger the size of the area of their brains affected by their strokes, the worse that their outcomes will be. However, in a lead article in the Archives of Physical Medicine and Rehabilitation, Page’s research team found that there was no relationship between the size of stroke lesions and recovery of arm function in 139 stroke survivors. On average, study participants had experienced a stroke five years earlier.
“Historically, lesion size been thought to influence recovery, but we didn’t find that to be the case when looking at regaining arm and hand movement,” said Page, who also runs Ohio State’s B.R.A.I.N Lab, a research group dedicated to developing approaches to restore function after disabling injuries and diseases. “This has important implications because we know clinicians look closely at lesion volume and may make decisions about the type and duration of therapy, and that some may communicate likelihood for recovery to patients based on this size. Many people think the window for therapy is roughly six months, but we think it’s much longer.”
Page agrees that the first six months after a stroke may represent important healing time for the brain, but that “retraining” it with occupational therapy can potentially be helpful at any time after the stroke. He says that his findings support other theories that the health of remaining brain tissue influences recovery much more than lesion size.
Although there are many studies that have identified a relationship between stroke lesion size and overall neurological function, Page’s study is the first to specifically look at lesion size and upper extremity outcomes.
Robotic arm as good as traditional therapy
In the second study, Page’s team demonstrated that stroke survivors using a portable robotic-assisted arm to perform repetitive task training showed as much motor recovery as patients who performed similar tasks in a therapist-guided outpatient setting.
“Our results are exciting not just because we showed robotics-assisted therapy can offer equal benefit. We showed that both groups got better, even among patients who had suffered strokes as long as eight years ago,” noted Page.
For the study, which was published in the June 2013 issue of Clinical Rehabilitation, patients performed repetitive exercises that focused on everyday tasks while supervised by a therapist in an outpatient setting. Half of the group was randomly assigned to use the robotic arm, a portable device that is worn over the arm like a brace. When a person tries to move a weakened arm, the device senses the electrical impulses and helps the person carry out the movement. A second group performed the same tasks without the device for the same amount of time and in the same environment. The group training with the robotic arm performed tasks as well as their counterparts.
“Therapy can be tiring, expensive, and resource-intensive. This study is important because it shows us that in patients with moderate arm impairment, similar benefits can be derived from using a robotic device to aid with arm therapy as with manually based rehabilitative approaches,” said Page. “Study participants who trained with the robotic arm also reported feeling stronger and more positive about the rehabilitation process.”
Most of the estimated 80 million stroke survivors worldwide will continue to have upper body weakness for months after a stroke, preventing them from accomplishing everyday tasks like lifting a laundry basket or drinking from a cup. Page says that more research in stroke outcomes and rehabilitation is needed, and that he hopes families and healthcare practitioners dealing with stroke will keep the door to recovery open wider and longer.
“Loss of upper extremity movement remains one of the most common and devastating stroke-induced impairments. And the fact is that more stroke survivors are expected yet studies and pathways to optimize rehabilitative therapy for these millions are not always emphasized. In particular, we know active rehabilitation programs help people regain function, but we still don’t know who will benefit the most from these types of therapy,” said Page. “Both of these studies give us insights about patients who will respond best – and most importantly, that we have to give these patients every chance possible to get better, because they can keep getting better.”
Click here to see video of a stroke survivor using the bionic arm.
Source: The Ohio State University Wexner Medical Center
Latest Articles
Stroke
Patient in rehab with device. (Credit: Image courtesy of Ohio State University Wexner Medical Center) Stroke survivors left weakened or partially paralyze...