A new military trauma care protocol for managing haemorrhage and resuscitation may assist in saving both combat and civilian patients, according to a new study published in the AANA Journal.
David Gaskin, CRNA, MHS, and co-authors write that although “haemorrhage is a less common cause of death than a central nervous system injury, it is the most common cause of preventable death in both civilian and military casualties.” Gaskin and his team examined two unique cases involving military casualties.
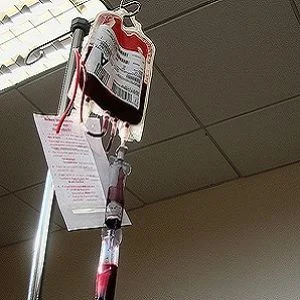
In the military, while providing care in a forward combat zone, the transfusion of packed red blood cells (PRBC) and fresh frozen plasma (FFP) is performed in a 1:1 ratio. While some civilian facilities follow this example, the approach is not universally accepted. Due to difficulties related to packaging and thawing of the plasma in combat zones, delays can happen in being able to quickly administer a sufficient quantity of blood to trauma patients. The severe loss of blood and the inability to replenish it in a timely manner can create new problems for patients that may be life threatening.
In a far forward military environment, the situation is even more dire. Thawing the thinly packaged FFP, which is stored at -20C, can cause ruptures in the plastic, creating delays in thawing other blood component units in the warmer. “Approximately 25 percent will experience a break in the bag as thawing occurs, rendering them unavailable for use,” according to the study.
See Also: Golden Hour Policy Improves Combat Survival
A second issue in a military environment is the challenge of effectively communicating with live donors on site, which also can cause delays in obtaining fresh blood supplies.
Following the surgery performed in one of the cases, protocols were identified and implemented to keep four FFP units thawed and ready for immediate use at all times. Other procedural changes that came from this case study included identifying and prescreening additional donors, and implementing a phone roster and base-wide overhead system to aid in rapid notification of these critical human resources.
The results “suggest that efforts to incorporate this resuscitation strategy into civilian practice may improve outcomes, and warrant continued study,” assert the authors.
Since World War I, most of the anaesthesia providers deployed in Forward Operating Bases in combat areas have been CRNAs. In these challenging settings, the authors note, CRNAs are responsible for the entire anaesthetic process, critically analysing information and rapidly developing a plan of care, often with little or no medical history of the patient, and safely delivering lifesaving anaesthetic care to wounded soldiers and civilians. CRNAs do this with limited resources in the most austere environments.
Source: American Association of Nurse Anesthetists
Image credit: Flickr.com
David Gaskin, CRNA, MHS, and co-authors write that although “haemorrhage is a less common cause of death than a central nervous system injury, it is the most common cause of preventable death in both civilian and military casualties.” Gaskin and his team examined two unique cases involving military casualties.
In the military, while providing care in a forward combat zone, the transfusion of packed red blood cells (PRBC) and fresh frozen plasma (FFP) is performed in a 1:1 ratio. While some civilian facilities follow this example, the approach is not universally accepted. Due to difficulties related to packaging and thawing of the plasma in combat zones, delays can happen in being able to quickly administer a sufficient quantity of blood to trauma patients. The severe loss of blood and the inability to replenish it in a timely manner can create new problems for patients that may be life threatening.
In a far forward military environment, the situation is even more dire. Thawing the thinly packaged FFP, which is stored at -20C, can cause ruptures in the plastic, creating delays in thawing other blood component units in the warmer. “Approximately 25 percent will experience a break in the bag as thawing occurs, rendering them unavailable for use,” according to the study.
See Also: Golden Hour Policy Improves Combat Survival
A second issue in a military environment is the challenge of effectively communicating with live donors on site, which also can cause delays in obtaining fresh blood supplies.
Following the surgery performed in one of the cases, protocols were identified and implemented to keep four FFP units thawed and ready for immediate use at all times. Other procedural changes that came from this case study included identifying and prescreening additional donors, and implementing a phone roster and base-wide overhead system to aid in rapid notification of these critical human resources.
The results “suggest that efforts to incorporate this resuscitation strategy into civilian practice may improve outcomes, and warrant continued study,” assert the authors.
Since World War I, most of the anaesthesia providers deployed in Forward Operating Bases in combat areas have been CRNAs. In these challenging settings, the authors note, CRNAs are responsible for the entire anaesthetic process, critically analysing information and rapidly developing a plan of care, often with little or no medical history of the patient, and safely delivering lifesaving anaesthetic care to wounded soldiers and civilians. CRNAs do this with limited resources in the most austere environments.
Source: American Association of Nurse Anesthetists
Image credit: Flickr.com
References:
Gaskin D et al. (2015) Far Forward Anesthesia and Massive Blood Transfusion: Two Cases Revealing the Challenge of Damage Control Resuscitation in an Austere Environment. AANA Journal, October 2015;
83(5):337-343.
Latest Articles
healthmanagement, trauma, haemorrhage, military medicine, resuscitation, blood transfusion
A new military trauma care protocol for managing haemorrhage and resuscitation may assist in saving both combat and civilian patients, according to a new study published in the AANA Journal.