Hospitalisation rates for aortic dissection (AD) have remained stable, although survival rates have improved particularly in patients undergoing surgical repair, according to a new study reported in the November 2014 issue of Circulation: Cardiovascular Quality and Outcomes.
Researchers examined US inpatient Medicare data from 2000 to 2011 to determine trends in hospitalisation, mortality and interventions for patients with AD. Mortality rates were ascertained through corresponding vital status files. In all, 32,057 initial hospitalisations for AD were identified by the researchers from the University of Texas Southwestern Medical Center (Dallas, TX, USA), Yale-New Haven Hospital (YNHH; New Haven, CT, USA), and other institutions.
During the study period, the overall hospitalisation rate for AD remained stable at 10 per 100,000 person-years. Rates were also stable for all age, race and sex subgroups, and remained highest for older, male and black adults, the research team noted.
AD occurs when a tear in the inner wall of the aorta causes blood to flow between the layers of the wall of the aorta, forcing them apart. In most cases, AD is associated with severe characteristic chest or abdominal pain, often with other symptoms that result from decreased blood supply to other organs. If the blood-filled channel ruptures through the outside aortic wall, aortic dissection is often fatal.
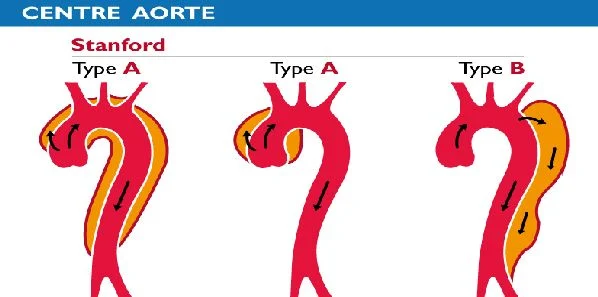
The Stanford classification divides AD into two groups. Type A involves the ascending aorta and/or aortic arch, and possibly the descending aorta. In Type B, the descending aorta or the arch (distal to the left subclavian artery) is dissected, without involvement of the ascending aorta.
The retrospective study revealed the following results:
“The reason for the improvement in mortality in operative patients might have been subtle improvements on various fronts, such as neuroprotection, improved intraoperative and postoperative pharmacological therapy, operative algorithm and standardised cannulation techniques, and development of care teams,” explained senior author Harlan Krumholz, MD, of YNNH, and colleagues. “Additionally, part of the improvement in mortality seen with Type B dissection could be possible because of the increasing use of the endovascular approach in the treatment of surgically high-risk patients.”
The study was supported by the National Heart, Lung, and Blood Institute (NHLBI).
Source: HospiMedica.com
Image Credit: Google Images
Researchers examined US inpatient Medicare data from 2000 to 2011 to determine trends in hospitalisation, mortality and interventions for patients with AD. Mortality rates were ascertained through corresponding vital status files. In all, 32,057 initial hospitalisations for AD were identified by the researchers from the University of Texas Southwestern Medical Center (Dallas, TX, USA), Yale-New Haven Hospital (YNHH; New Haven, CT, USA), and other institutions.
During the study period, the overall hospitalisation rate for AD remained stable at 10 per 100,000 person-years. Rates were also stable for all age, race and sex subgroups, and remained highest for older, male and black adults, the research team noted.
AD occurs when a tear in the inner wall of the aorta causes blood to flow between the layers of the wall of the aorta, forcing them apart. In most cases, AD is associated with severe characteristic chest or abdominal pain, often with other symptoms that result from decreased blood supply to other organs. If the blood-filled channel ruptures through the outside aortic wall, aortic dissection is often fatal.
The Stanford classification divides AD into two groups. Type A involves the ascending aorta and/or aortic arch, and possibly the descending aorta. In Type B, the descending aorta or the arch (distal to the left subclavian artery) is dissected, without involvement of the ascending aorta.
The retrospective study revealed the following results:
- For 30-day and one-year mortality associated with AD, the observed rate decreased from 31.8 percent to 25.4 percent and from 42.6 percent to 37.4 percent, respectively.
- For patients undergoing surgical repair for Type A dissections, the observed 30-day mortality decreased from 30.7 percent to 21.4 percent, and the observed one-year mortality decreased from 39.9 percent to 31.6 percent.
- For surgical repair of Type B dissections, the 30-day mortality decreased from 24.9 percent to 21 percent, and the one-year rate decreased from 36.4 percent to 32.5 percent.
“The reason for the improvement in mortality in operative patients might have been subtle improvements on various fronts, such as neuroprotection, improved intraoperative and postoperative pharmacological therapy, operative algorithm and standardised cannulation techniques, and development of care teams,” explained senior author Harlan Krumholz, MD, of YNNH, and colleagues. “Additionally, part of the improvement in mortality seen with Type B dissection could be possible because of the increasing use of the endovascular approach in the treatment of surgically high-risk patients.”
The study was supported by the National Heart, Lung, and Blood Institute (NHLBI).
Source: HospiMedica.com
Image Credit: Google Images
Latest Articles
Aorta, Endovascular, neuroprotection, aortic dissection, chest pain
Hospitalisation rates for aortic dissection (AD) have remained stable, although survival rates have improved particularly in patients undergoing surgical r...