ICU Management & Practice, Volume 18 - Issue 1, 2018
Regarding the growing number of patients with long-term mechanical assist devices, intensivists need to understand the physiology of the devices, their functioning, potential complications and their management.
Long-term mechanical circulatory support (MCS) is being used increasingly for patients at risk of dying from heart failure and cardiogenic shock (Ponikowski et al. 2016; Gustafsson and Rogers 2017). As a result, intensivists who do not have training in managing advanced heart failure patients are increasingly likely to encounter patients requiring MCS at various points in the trajectory of their disease, especially during subsequent admissions for complications (Pratt et al. 2014; DeVore et al. 2014). A basic understanding of ventricular assist device (VAD) physiology is essential for the safe and effective care of these patients. This review highlights the physiology of patients with MCS and management of common complications relevant to the critical care physicians.
Indications of long-term MCS
MCS systems can be used to unload the failing ventricle and maintain sufficient end-organ perfusion. While heart transplantation (HT) is a highly effective therapy for advanced refractory heart failure (HF), it is limited to <10% of candidates, due to a severe shortage of donor organs and a variety of contraindications (Ponikowski et al. 2016; Aissaoui et al. 2018). This paucity of effective therapy promoted the development of VAD, which may be used as a) a bridge to HT or b) a long-term alternative to HT, also known as destination therapy.
Depending on which ventricle is assisted, three categories of long-term MCS are available: left VAD, biventricular assist device, and total artificial heart (TAH) (Ponikowski et al. 2016; Mehra et al. 2017).
Improvements in technology, especially the advent of smaller, durable continuous flow pumps, have led to the use of LVADs in a much broader population of patients in the last 10 years (Gustafsson and Rogers 2017). It is estimated that 2000 pumps are implanted annually in Europe. Compared with LVADs, TAH is implanted in a much smaller subset of patients (Cook et al. 2015; Torregrossa et al. 2014). Data from the most recent analysis from the LVAD registry show a one-year survival rate of 80% (Gustafsson and Rogers 2017). Concerning TAH patients, the most recent multicentre studies reported a one-year survival rate between 56% to 76% (Cook et al. 2015; Torregrossa et al. 2014).
Device physiology: what should intensivists know?
Management of these patients requires an understanding of the principles, indications and limitations of this unique technology.
LVAD
LVAD are intracorporeal rotary pumps that unload the LV continuously. A percutaneous driveline connects the pump to an external controller and a power source (Gustafsson and Rogers 2017). The three currently approved LVADs are the HeartWare HVAD (HeartWare International, Inc. Framingham, MA), the HeartMate II (Thoratec Corporation, Pleasanton, CA) and the newest HeartMate 3™ (Thoratec Corporation, Pleasanton, CA) (Mehra et al. 2017) (Figure 1). Pump parameters are key and include the following (Figure 1) (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014; Estep et al. 2015).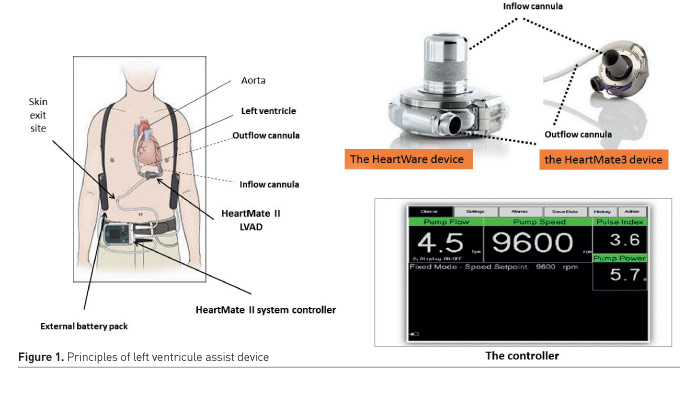
Pump speed (revolutions per minute, RPM) is the only variable programmed by the operator. For each patient, it is adjusted after implantation by the heart failure physician [between 8000 and 10000 rpm for HeartMate II, 2400-3200 rpm for HeartWare and 4000-6000 rpm for HeartMate 3].
Pump flow is the blood flow displayed on the LVAD monitor and calculated based on measured pump power and set pump speed. The device flow is directly proportional to the pump speed and inversely related to the LV intracavitary pressure, i.e. the difference of pressure in the inflow and outflow cannulas (Figure 2). Any change in pump function or in patient condition may lead to significant changes in pump flow.
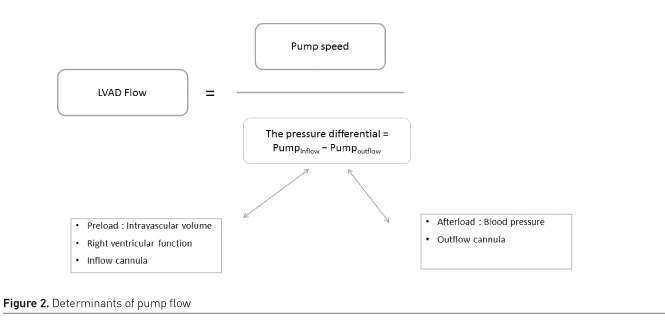
The Pulsatility index corresponds to the magnitude of flow pulse through the pump. It fluctuates with changes in volume status and with heart contractility (Heartmate II and 3).
Total artificial heart
For patients with severe biventricular failure and/or valvular mechanical prosthesis, a TAH may be an option (Cook et al. 2015; Torregrossa et al. 2014). TAHs replace all functions of the native heart. The most used TAH is the CardioWest TAH consisting of two polyurethane ventricles (Figure 3). The newest CARMAT TAH, an implantable electro-hydraulically actuated pulsatile biventricular pump will probably replace the CardioWest TAH in the future (Latrémouille et al. 2018). The CardioWest device is typically set to partially fill and runs at a fixed percentage of systole and a fixed beat rate of 120 to130 bpm with a stroke volume of 50–60 mL (Cook et al. 2015; Torregrossa et al. 2014). The clinician can modify several parameters to optimise cardiac output: beat rate, drive pressure, percentage of time in systole, and vacuum pressure. Depending on exercise or volume status, the cardiac output may automatically increase in response to an increase in venous return and preload such as in a normal heart.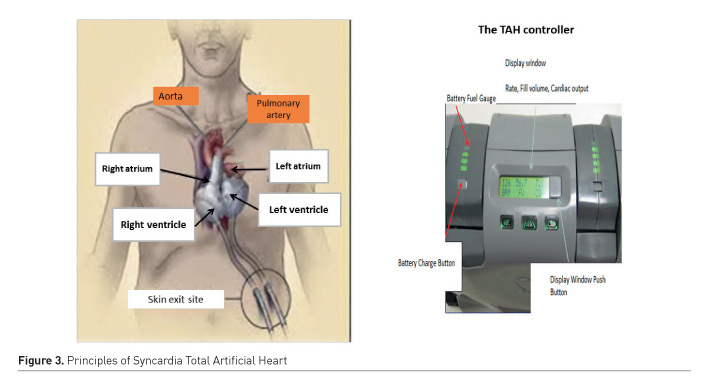
Which medication and specific care are required in VAD patients?
Anticoagulation and antiplatelet therapy. Anticoagulation protocols vary by institution, device, and individual patient. Patients are typically receiving therapy with aspirin (81–325 mg) and warfarin (goal INR 2.0–3.0) (Gustafsson and Rogers 2017; Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014; Cook et al. 2015; Torregrossa et al. 2014; Mehra et al. 2017). Management of MCS patients requires assessment of the risks of thrombosis and haemorrhage (Suarez et al. 2011).
Medications of advanced HF. Despite the lack of evidence and in order to favour weaning, the guidelines used for patients under MCS are those used for heart failure patients (Gustaffson and Rogers 2017). Specifically, and according to the most recent International Society of Heart and Lung Transplant (ISHLT) guidelines, mean blood pressure (BP) should be lower or equal to 80 mm Hg with a typical goal range between 70 and 80 mmHg to prevent stroke and LVAD dysfunction due to increased afterload (Estep et al. 2017).
Driveline. The most important factor in preventing the morbidity of infections is anchoring the device to help stabilise the driveline, thus minimising trauma and tension at the exit site (Gustafsson and Rogers 2017; Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014). The patient follows a sterile dressing care regimen in accordance with protocol and has to monitor the driveline exit site for redness, drainage, tenderness and open areas at the site.
Why do patients with LVAD come into the ICU?
The most frequent complications occurring in MCS patients are bleeding, driveline infections, thrombosis, device malfunction, right ventricular (RV) failure and arrhythmias (Gustafsson and Rogers 2017; Cleveland et al. 2011; Feldman et al. 2013). Patients with MCS can also be admitted to the ICU for non-specific aetiologies (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014).
The implanting hospital and VAD coordinator should be contacted for each MCS patient requiring admission into the ICU (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014; Mehra et al. 2017). Some patients may be managed by non-LVAD specialists after advice and agreement of the implanting team whereas all TAH should be transferred to the implanting hospital.
Frequent complications in MCS patients
Bleeding is the most frequent adverse event in MCS due to combination anticoagulation and acquired von Willebrand disease due to the sheer stresses in the pump (Suarez et al. 2011). Bleeding events (after one month from VAD implantation) are epistaxis, gastrointestinal bleeding, intracranial haemorrhage and mediastinal and thoracic bleeding.
Infection is the second most common cause of death after cardiac failure in MCS patients (Estep et al. 2015; Feldman et al. 2013). The driveline exit sites need special attention. An infection can develop and ascend up to the device. LVAD-specific infections are located on the driveline or pump pocket (Kusne et al. 2017). They need aggressive treatment by including blood culture: blood cultures, antibiotics, surgical debridement, and even HT (Kusne et al. 2017).
Major thrombotic events in LVAD patients include pump thrombosis and arterial thromboembolism.
One of the common causes of a low cardiac output state is device thrombosis, which occurs in approximately 8% (per year) of implanted, continuous-flow LVAD (Aissaoui et al. 2012). Signs of pump thrombosis include haemolysis, thromboembolism events, heart failure, and, ultimately, cardiogenic shock with elevated power uptake and high calculated flows (reading on the LVAD controller). Such patients will need increased anticoagulant medications, thrombolytic therapy, a device exchange or urgent HT (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014; Feldman et al. 2013; Aissaoui et al. 2012). Device thrombosis can develop even when patients are fully anticoagulated and taking antiplatelet therapy, because the LVAD causes a chronic hypercoagulable state (Aissaoui et al. 2012).
The major complications of TAH implantation include strokes, infection, bleeding, thrombosis, renal failure and chronic anaemia (Cook et al. 2015; Feldman et al. 2013).
Cardiac arrest. Consequences of cardiac arrest on pump function highly depend on cardiac rest function. While some patients will collapse immediately, others may even be able to exercise. The impact of ventricular arrhythmia is also variable, sometimes creating some kind of Fontan circulation, with a sufficient output flow. In general, LVAD patients in cardiac arrest who are collapsing should be managed according to the Advanced Cardiac Life Support (ACLS) recommendations, with some precautions (Hazinski et al. 2015; Nolan et al 2015).
The major risk factor to chest compressions during cardiopulmonary resuscitation is dislodgement of the device or its outflow cannula, located directly beneath the sternum (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014). A potential alternative to chest compression is abdominal compression 1 to 2 inches left of midline, as previously described although still not currently recommended (Pratt et al. 2014; Sen et al. 2016).
Patients with device stoppage can present in severe cardiogenic shock or full arrest and should be managed appropriately while searching for the cause of malfunction. In these cases, the VAD coordinator should be contacted immediately and all of the VAD equipment should be assessed to verify that critical connections are intact. The driveline and power supply should be checked and reconnected if disconnected (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014). Alarms should be assessed. If there is a VAD hum, it should be assessed with auscultation. Doppler ultrasonography should be used to evaluate the patient’s BP and echocardiography to assess some haemodynamic parameters and look for VAD complications.
Once restarted, a major concern is thromboembolism from the device. Device exchange can be performed emergently if necessary and feasible.
Electrical activity without cardiac contractility should prompt a search for underlying causes, such as tension pneumothorax and electrolyte derangements.
Noncardiac surgery. Noncardiac surgery presents an increased risk of morbidity due to bleeding (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014). However, it can be performed if a VAD coordinator or nurse familiar with the management of the device accompanies patients in the operating room to manage the console, monitor LVAD flow and address any alarms. If emergency surgery at a centre without VAD support is necessary, care providers should call the manufacturer or nearest hospital with a VAD programme to obtain advice and recommendations on management of the device. Intra-abdominal procedures must proceed with extreme caution to avoid encountering the subcutaneously tunnelled driveline. Ultrasound can be used to mark the driveline’s location. No protocols exist for managing anticoagulation in the perioperative period, and a variety of approaches have been used.
Suction events. A suction event occurs when there is reduced filling of the pump (reduced preload), which increases negative pressure within the LV. During this event, part of the LV wall is sucked over and covers the pump’s inlet cannula, generating an alarm and a decrease of speed to release the suction. Suction events are caused by low volume, RV failure or tamponade. Suction events can lead to low LVAD flows and can trigger ventricular arrhythmias. The management includes decreasing the RPM rate and administering fluid.
Specific monitoring
Blood pressure. Contrary to TAH patients, it can be difficult to record BP using traditional measurements in LVAD patients with a reduced pulse pressure (Estep et al. 2015). A Doppler ultrasound probe that detects flow at any point during the cardiac cycle and measures an opening pressure may be useful. In cases of shock, an arterial catheter should be inserted for continuous mean arterial pressure (MAP) monitoring and is best placed via ultrasonographic guidance (continuous flow makes blind placement difficult) (Pratt et al. 2014; Sen et al. 2016; DeVore et al. 2014; Estep et al. 2015).
Echocardiography. Echocardiography is fundamental in the management of LVAD patients but should be interpreted with knowledge of the patient’s clinical status (Stainback et al. 2015).
It is useful to assess haemodynamic parameters:
- LV size and function
- Position of the ventricular septum (flat and neutral)
- Competency of the aortic valve (it should be competent and open intermittently, every second or third beat)
- RV size and function
- Inferior vena cava and collapsibility
- Signs of pericardial effusion or tamponade
- Inflow cannula (if visualised) aligned with the mitral valve; and
- Outflow cannula (if visualised).
Bedside echocardiography can also detect and/or diagnose LVAD complications. It is useful in TAH patients.
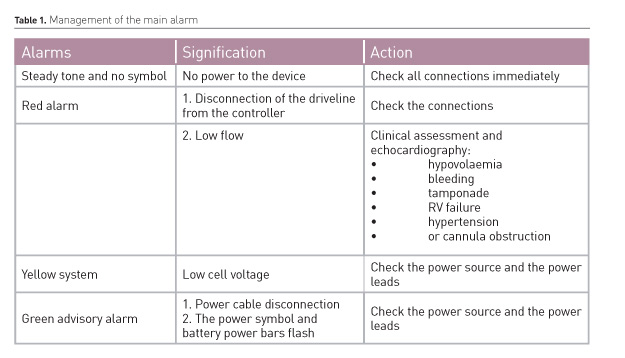
Advisory alarms. Table 1 reports the main alarms to look out for and to manage.
If there is a steady tone and no symbol, there is no power to the device. All connections should be checked immediately (the system driver connections to the device and the system driver and power connections to the power source), because patients may be at risk of cardiopulmonary arrest.
The red hazard alarm can indicate disconnection of driveline from the controller, low flow or incorrect operation, and so the connections need to be checked. It may also suggest hypovolaemia, bleeding, tamponade, RV failure, hypertension, or cannula obstruction. In these cases, both the patient and the device should be assessed emergently.
The yellow system driver signals low cell voltage. When this occurs, the cell battery should be replaced and a system controller self-test performed. The green advisory alarm signals a power cable disconnection; the power symbol and battery power bars flash. Cable connections to the power source should be checked and power leads should be assessed for damage and replaced if necessary.
Conflict of interest
Nadia Aissaoui declares receipt of Medtronic grant for congress participation. All other authors declare that they have no conflict of interest.Abbreviations
HF heart failure
HT heart transplanatation
LVAD left ventricular assist device
MCS mechanical circulatory support
TAH total artificial heart
VAD ventricular assist device
References:
Aissaoui N, et al. (2018) Management of end-stage heart failure patients with or without ventricular assist device: an observational comparison of clinical and economic outcomes. Eur J Cardiothorac Surg, 53(1): 170-7.
Cleveland JC Jr et al. (2011) Survival after biventricular assist device implantation: an analysis of the Interagency Registry for Mechanically Assisted Circulatory Support database. J Heart Lung Transplant, 30(8): 862-9.
Cook JA et al. (2015) The total artificial heart. J Thorac Dis, 27(12): 2172–80.
DeVore AD et al. (2014) Medical management of patients with continuous flow left ventricular assist devices. Curr Treat Options Cardiovasc Med, 16(2): 283.
Estep JD et al. (2015) Continuous flow left ventricular assist devices: shared care goals of monitoring and treating patients. Methodist Debakey Cardiovasc J, 11(1): 33-44.
Feldman D et al. (2013) The 2013 International Society for Heart and Lung Transplantation Guidelines for mechanical circulatory support: executive summary. J Heart Lung Transplant, 32(2): 157- 87.
Gustafsson F and Rogers JG (2017) Left ventricular assist device therapy in advanced heart failure: patient selection and outcomes. Eur J Heart Fail, 19(5): 595-602.
Hazinski MF et al. (2015) Part 1: Executive Summary: 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation 132(16 Suppl 1): S2–39.
Kusne S et al. (2017) An ISHLT consensus document for prevention and management strategies for mechanical circulatory support infection. J Heart Lung Transplant, 36: 1137-1153.
Latrémouille C et al. (2018) A bioprosthetic total artificial heart for end-stage heart failure: Results from a pilot study. J Heart Lung Transplant, 37(1): 33-7.
Mehra MR et al. (2017) A fully magnetically levitated circulatory pump for advanced heart failure. N Engl J Med, 376(5): 440-450.
Nolan JP et al. (2015) European Resuscitation Council and European Society of Intensive Care Medicine 2015 guidelines for post-resuscitation care. Intensive Care Med, 41(12): 2039–56.
Ponikowski P et al. (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J, 37(27): 2129-200.
Pratt AK et al. (2014) Left ventricular assist device management in the ICU. Crit Care Med, 42 (1): 158–68.
Sen A et al. (2016) Mechanical circulatory assist devices: a primer for critical care and emergency physicians. Crit Care, 20(1): 153.
Stainback RF et al. (2015) Echocardiography in the Management of Patients with Left Ventricular Assist Devices: Recommendations from the American Society of Echocardiography. J Am Soc Echocardiogr, 28: 853-909.
Suarez J et al. (2011) Mechanisms of bleeding and approach to patients with axial-flow left ventricular assist devices. Circ Heart Fail, 4:779–784.
Torregrossa G et al. (2014) Results with SynCardia total artificial heart beyond 1 year. ASAIO J, 60(6): 626-34.














