ICU Management & Practice, ICU Volume 8 - Issue 3 - Autumn 2008
Author
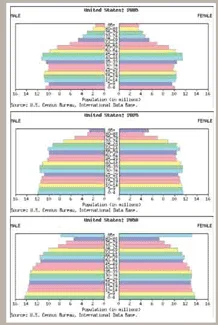
The Baby Boom has become the Elder Explosion. According to U.S. Census figures, the population age 85 and over will grow fivefold by the year 2030 (Figure 1). By 2050, up to 50% of U.S. income tax dollars could go to pay for Medicare.
This is the first in a series of articles in ICU Management concerning the impact of the aging population on our hospitals. These changes are beginning to be felt in our operating rooms and intensive care units and these areas will be examined in our first installment. In 2005, over 13.2 million persons aged 65 and older were discharged from short stay hospitals. This is a rate of 3,596 for every 10,000 persons aged 65+, which is over three times the comparable rate for persons of all ages (Department of Health and Human Services 2007). The rates of ICU admission and utilisation in those ≥85 years old were 58.2 admissions/1,000 residents and 195.8 days/1,000 residents compared with 3.8 admissions/1,000 residents and 11.5 days/1,000 residents in those 18 to 44 years old (Seferian and Afessa 2006). Surgery in the elderly is also on the rise. One out of five of those over age 60 will undergo surgery and anesthesia as compared with only one in ten of those aged 45 to 60 years by 2030. One out of five open-heart surgeries are performed on those over age 70.
Reducing Surgical Risk in Our ICUs
There have been several strategies to reduce perioperative cardiac risk. Pharmacologically, the perioperative use of statins has been supported in recent literature. Studies suggest that statins are protective, but only one article can be used to base clinical recommendations (Williams et al. 2008). Also, there seems to be a rebound effect with statins and, therefore, they should not be discontinued postoperatively. It is unclear whether this effect is independent of lipid status of the patient.Beta blockade has also been popularised and is now driven by the Centers for Medicare and Medicaid Services in the Surgical Care Improvement Project. The therapeutic goal is to control the patient’s preoperative heart rate at or below 60. However, many patients do not or cannot reach this goal for various reasons. These include nature of the surgery as emergent and symptomatic bradycardia. One recent meta-analysis calls this practice into question (Biccard et al. 2008). The authors “…cannot confirm that heart rate control with beta-adrenergic blockade is cardioprotective.”
A recent paper from the anaesthesia literature questions both practices, of perioperative beta blockade and statin use (Daumerie and Fleisher 2008). The authors suggest that “based upon the available evidence and guidelines, patients currently taking [beta-]blockers should continue these agents. Patients undergoing vascular surgery who are at high cardiac risk should also take [beta-]blockers. The question remains regarding the best protocol to initiate perioperative [beta-]blockade. Statins should be continued in patients already taking these agents prior to surgery. The optimal duration and time of initiation of statin therapy remains unclear.”
So what else is at our disposal to reduce perioperative risk in our ICU? Preoperative cardiac and pulmonary evaluations are routinely performed. Clearly, preoperative optimisation of respiratory function is important in decreasing adverse pulmonary events. This optimisation includes cessation of smoking. Preoperative cardiac evaluation can improve outcomes but generally focuses on only the cardiac issues. This is perhaps why systems developed to follow American College of Cardiology and American Heart Association guidelines perform well, perhaps even more efficaciously, in the hands of non-cardiologists (Cinello et al. 2007; Almanaseer et al. 2005).
Recent literature points to a new way to clear elderly patents preoperatively that may follow from the cardiac clearance literature mentioned above. A preoperative comprehensive geriatric assessment (CGA) takes into account the above measures as well as those which, to date, have been relatively ignored. This type of assessment is not limited to a history, physical, and tests. A comprehensive variety of items are examined including functional ability, mental health, social support, and environment. Special issues addressed in the history include sleep, alcoholism, abuse, pain, continence, nutrition, mobility, gait, balance, driving, and sexuality. The physical portion adds functional and cognitive evaluations. These may include functional independence measures (FIM), activities of daily living (ADLs), and instrumental ADLs, Mini Mental Status Exam, or Mini-Cog. Other areas evaluated include caregivers, social support, home safety, values, goals of treatment, and advance directives.
The literature in support of CGA includes use in thoracic surgery (Fukuse et al. 2005). In thoracic surgery patients, dependence for the performance of ADLs and impaired cognitive conditions are important predictors of postoperative complications, especially when the operation time is long. CGA was deemed necessary in addition to the conventional cardiopulmonary assessment in elderly patients. This also applies to cancer patients (Repetto et al. 2002). Factors outside the usual cardiac and pulmonary clearance, such as cognitive and functional performance, have been shown in many studies to influence outcomes. A 2007 study from the United Kingdom showed improved outcomes using CGA in the preoperative setting (Harari et al. 2007). “A proactive evidence-based CGA service for at-risk older elective surgical patients was developed. Pre/post comparison in elective orthopaedic patients showed improved (within methodologi cal limitations) postoperative outcomes indicative of better clinical effectiveness and efficiency...”
The American Geriatrics Society has issued a position statement concerning interdisciplinary care of the elderly (Mion et al. 2006). It states:
(1) Interdisciplinary care meets the complex needs of older adults with complex comorbidities.
(2) Interdisciplinary care improves healthcare processes and outcomes for geriatric syndromes.
(3) Interdisciplinary care benefits the healthcare system and the caregivers.
(4) Interdisciplinary training and education effectively prepares healthcare providers to care for older adult.
Conclusion
As the above literature and data reflect, there should be a new way to treat the elderly in our SICU. This new paradigm could include a preoperative comprehensive geriatric assessment in addition to cardiopulmonary clearance. New risk reduction strategies should be employed as per recommendations. Geriatric consultations should be obtained in all cases, emergent or elective. They, in addition to the primary team and intensive care team, should be a part of an interdisciplinary group that manages the care of the elderly patient. We will look more specifically at the data supporting this team approach in our next article in this series in ICU Management on Eldertrauma Care.Through adherence to the above principles, can we achieve better outcomes when cure is possible and better, more dignified palliative care when cure is not possible.
�