ICU Management & Practice, Volume 18 - Issue 2, 2018
A French study of patients with lung cancer or end-stage tracheal lesions has successfully used cryopreserved human aortic grafts to rebuild the windpipe and airway sections removed because of disease. The study is published in JAMA, to concide with its presentation at the American Thoracic Society 2018 conference.
The study, Airway and/or Pulmonary Vessels Transplantation (TRACHBRONCAR) [clinicaltrials.gov/ct2/show/NCT01331863], was led by Emmanuel Martinod, MD, PhD, professor of thoracic surgery at the Assistance Publique Hôpitaux de Paris and University of Paris. The study included 20 patients, who had had sections of their windpipe removed, and followed those who received airway transplantation (5 tracheal, 7 bronchial, 1 carinal) between October 2009 and February 2017, with final follow-up in November 2017.
You might also like: Bioengineering approach to artificial tracheas
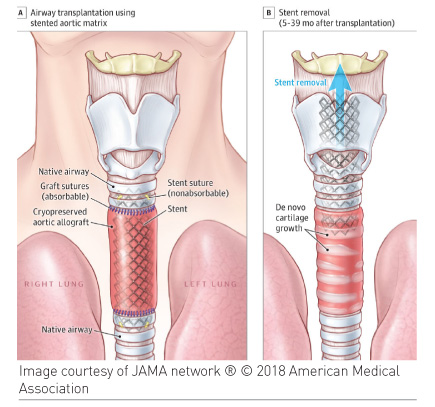
The surgery involved airway transplantation using a cryopreserved aortic graft, which was not matched by the ABO and leukocyte antigen systems, and a custom-made stent that was inserted into the graft to keep the airway from collapsing but was later removed, at a mean postoperative period of 18 months.
Results
One patient, who underwent carinal transplantation, died (5% 90-day mortality). No patients who underwent tracheal or bronchial reconstruction died after 90 days. After nearly four years 10/13 patients were alive, and 8/10 were breathing normally through newly formed airways after stent removal. In addition, new generation of cartilage was seen in the transplanted areas. The researchers report that there were no major complications related to the allograft or the stent.
The authors conclude that this approach is feasible for complex tracheal and bronchial reconstruction. They recommend further studies and multicentre randomised clinical trials to evaluate the benefit-risk balance of the approach for specific indications such as end-stage tracheal diseases, locally advanced thyroid cancer, and proximal lung cancer. They also note additional areas for research, including accelerating the de novo cartilage generation to enable earlier stent removal, and assessment of long-term quality of life in patients who receive a transplant.
In an accompanying editorial, Valerie W. Rusch, MD, of Thoracic Service, Department of Surgery, Memorial Sloan Kettering Cancer Center, describes the study as an “elegant solution to challenges that have long bedeviled the field of tracheal surgery. For some patients with cancer, this approach may preserve lung function and quality of life by avoiding pneumonectomy while permitting an oncologically sound operation.”
References:
Martinod E, Chouahnia K, Radu DM et al. (2018) Feasibility of airway transplantation usinga bioengineered stented aortic allograft. JAMA, 20 May. doi: 10.1001/jama.2018.4653
Rusch VW (2018) Has reconstructionof the central airways been transformed? From aorta to trachea. JAMA, 20 May. doi:10.1001/jama.2018.4652





