Eliminating Redundant Chest Radiology
It is common for patients in the ICU, particularly those who are mechanically ventilated, to have daily routine chest radiographs in an attempt to find relevant abnormalities that would otherwise remain undetected.
A large study by Graat and colleagues evaluated the clinical value of 2,457 routine CXRs in a combined surgical and medical ICU and found that only 5.8% of routine CXRs showed new or unexpected findings, 2.2% of which warranted a change in therapy (Graat et al. 2006). Synonymous results were recorded for both medical and surgical patients.
A randomised control study of medical ICU (MICU) patients by Krivopal and his team divided MICU patients into those who received routine CXRs and those who only received non-routine (clinically indicated) CXRs. They came across a greater percentage of radiographs with significant findings, requiring intervention, in the non-routine group (26.5%) than in the routine group (13.3%) (Krivopal et al. 2003). Significant interventions included diuresis, antibiotic administration or an invasive procedure. The non-routine group also received significantly less radiographs per person than the routine group: 4.4 versus 6.8. There was no significant difference in outcome between the groups with regard to length of intubation, ICU stay, hospital stay or mortality.
More recently, Oba and Zaza (2010) conducted a meta-analysis, for which they selected eight studies that compared on-demand approaches with daily routine strategies, including a total of 7,078 patients. No difference in ICU mortality, ICU length of stay and duration of mechanical ventilation was found between the two groups. The meta-analysis highly suggests abandoning routine CXRs.
A review from Ioos and colleagues (2011) supports the approach for decreasing the number of CXRs ordered in the ICU, and addresses the use of alternative techniques like ultrasonography and capnography in:
1. Ensuring the correct position of enteral feeding tubes when combined with epigastric auscultation;
2. Diagnosing and monitoring pneumothoraces; and
3. Post-procedural techniques after central venous catheter insertions.
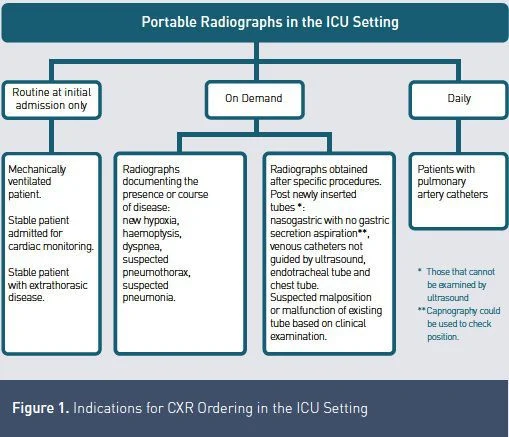
Based on our review of the best currently available evidence, and on the latest recommendations following the consensus opinion of the American College of Radiology expert panel, which was revised in 2006, we can summarise the acceptable indications for ordering CXRs in the ICU.
Conclusion
Previous studies advocating daily routine chest radiography in ICUs were all observational without providing a comparison. The efficacy of daily routine chest radiography was probably overestimated in these because of inadequate study design. To help in designing future studies, it is worth mentioning that clear identification of patient population, enrollment criteria, and various definitions of efficacy (unexpected findings, new findings and findings that lead to treatment change) are needed.
The CXR should never replace clinical evaluation of the patient but should be prescribed on the basis of clinical suspicion. As a consequence, the organisation of the ICU might have to be modified to allow the implementation of such a strategy for prescription and the reduction of the number of CXRs ordered.
Future Studies
More studies are needed to help in defining a guideline for selecting the most efficient and appropriate CXR strategy. The author of this article agrees with the suggestion from Hejblum et al. (2008) that bedside CXRs in adult ICUs be categorised into four groups (Figure 2). This classification system could help in future studies to identify specific ICU situations in which unnecessary CXRs can be reduced.