In fact, the
percentage of doctors in the U.S. who get disciplined or pay a malpractice
claim is four times less in some states than in others, a study by a pair of University of Michigan Medical
School researchers showed.
And since there probably isn’t a fourfold difference in the actual behaviour of doctors, the reason for this difference lies in the wide variation between states in their regulations, procedures and resources for punishing doctors who do wrong.
Consumer advocates have noted variation between states’ physician discipline rates and standards in the past. But this study, published in BMJ Quality and Safety, is the first nationwide academic evaluation of the topic, and uses statistical techniques to more reliably calculate the actual situation in each state.
Delaware, Kentucky and Ohio came in with the highest adjusted rates for all disciplinary actions. But it’s the states with the lowest rates - such as Massachusetts, New York, Connecticut and Pennsylvania - that should probably look the hardest at their current standards, say the researchers.
“We don’t know what the ‘right’ rate of physician disciplinary action is, but no state should want to be in the extremes,” said John A. Harris, M.D., senior author of the new paper. “Patients assume oversight of doctors is well-regulated in all states, that all doctors are held to the same ethical standards and disciplined appropriately when needed. But there’s no central governing body, and there’s significant variation.”
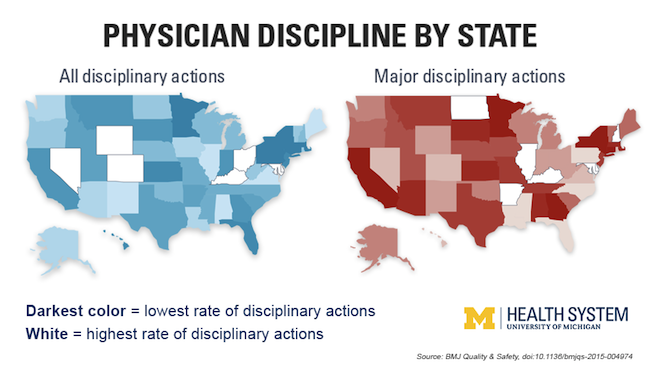
Image credit: University of Michigan
Harris and his co-author Elena Byhoff, M.D., are both Robert Wood Johnson Foundation clinical scholars at the U-M Medical School and the U-M Institute for Healthcare Policy and Innovation.
This is the latest study of physician misbehaviour by Harris, an obstetrician-gynecologist. He has also studied how the rise in female practitioners in his specialty has affected the rate of allegations of sexual misconduct against Ob/Gyn doctors.
National Data Reveals State Variation
The data for the study came from the U.S. Department of Health & Human Services’ National Practitioner Data Bank, which covers all 50 states and the District of Columbia. The researchers focused on the most recent data available, from 2010 to 2014.
Since 1986, the NPDB has collected data from each state on actions that state medical boards take against doctors who have been shown to have done something wrong, from substance abuse and sexual misconduct to improper prescribing, fraud and negligence.
The NPDB includes information about punishments ranging from minor fines or required monitoring, to major actions such as revoking or suspending a doctor’s medical license. It also includes information on payments made by doctors in response to malpractice claims, which the researchers used to create a measure of the malpractice climate in each state. It doesn’t include actions taken by individual hospitals that don’t get reported to the state medical board.
Hospitals, clinics, state medical boards and insurers routinely access the NPDB when making decisions about which physicians to hire, credential, license or include in their networks. Patients can’t access it, and public access to state-level information about individual physicians varies greatly by state, Harris said.
Harris and Byhoff combined all this with information on the number of physicians practicing in the state, to calculate a reliability-adjusted yearly state rate of all medical board disciplinary actions per 1,000 physicians.
For the U.S. as a whole, they show that there are 3.75 disciplinary actions each year for every 1,000 physicians practicing - including 1.15 serious disciplinary actions. But the yearly range among states was huge, from 7.93 disciplinary actions of any type per 1,000 physicians in Delaware down to 2.13 per 1,000 in Massachusetts, and from 2.71 major actions per 1,000 physicians in Delaware down to 0.64 in New York.
Medical Boards Make The Difference
The researchers note that in each state, the medical board acts as a self-governing body, with wide discretion on what kind of punishment to dole out for violations of different sorts.
“In one state the punishment for a particular violation could be a fine, while in another state you could lose your license for doing the same thing,” said Byhoff. “It has implications for the ability of physicians to move from state to state,” if their punishment in one state is not enough to keep a hospital or practice in another state from hiring them.
The researchers hope their findings will be heeded by state regulators and medical boards. Factors such as how easy it is to make a complaint to a state board, how many resources a board has to investigate complaints, the actual makeup of the board including how many non-physicians are on it, and the standards for making a judgment and choosing a disciplinary action all play into the variation, the researchers concluded.
The U.S. is one of a few countries that lack a national system for overseeing and punishing physician misbehaviour. Australia recently changed over to one, after decades with each state or territory having its own medical board. Studying other countries’ systems compared with the state-level systems in the U.S. could yield further information about how to address variation and protect the public, Harris noted.
“Don’t we want all doctors operating in the same ethical way, and being disciplined appropriately if they fail to do so?” he asked.
The researchers are supported by their fellowships from the Robert Wood Johnson Clinical Scholars Programme, and by the Department of Veterans Affairs.
Reference: BMJ Qual Saf 2016;0:1-8. doi:10.1136/bmjqs-2015-004974







