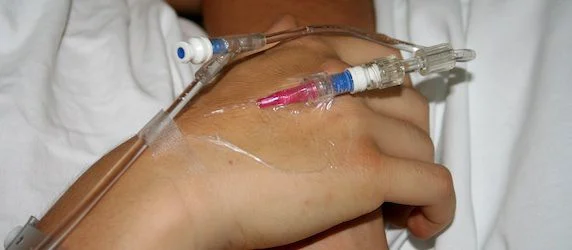
A report published by the National Institute for Health and Care Excellence warns that one third of surgery patients' death within days was caused by too much fluid.
Proper administration of intravenous (IV) drips in England and Wales’ hospitals is not practiced due to an "astonishing" lack of knowledge surrounding the issue, putting the lives of thousands of patients at risk according to experts.
The National Institute for Health and Care Excellence (Nice) has issued guidelines for medical practitioners on their use, as there is a risk of pneumonia or heart failure if a patient is given too much fluid, or kidney failure if they are given too little.
Dr Mike Stroud, a gastroenterologist who chaired the group that developed the guidelines, stated that the team was very confident about the need for improved procedures, since IV administration had not been done well in the past. Dr Stroud went on to express his astonishment about doctors and other healthcare providers not being well educated with regards to patient needs, since this was paramount in making hospitals safer.
According to Stroud IV drips constituted the second most commonly used therapy in acute hospitals, however surveys suggested nine out of 10 doctors were unaware of proper fluid dosage and timing, a fact he attributed to a lack of knowledge resulting from the modality not being a specialty, and as a consequence responsibility for it remained unassigned.
The fact that most patients on a drip were also receiving other treatments made it hard to pinpoint the consequences of mistakes, yet the estimate remains that tens of thousands of people are experiencing complications. Inappropriate administration of IV fluids has been quoted as a source of complications in two previous studies conducted in 1999 and 2011.
As per the Nice guidelines hospitals should identify an IV fluids champion and assign responsibility for training, clinical governance/auditing, monitoring patient outcomes and implementing the reporting of fluid mismanagement incidents.
Dr Jerry Nolan, a consultant in anaesthesia and intensive-care medicine who was part of the Nice guidance group, said the costs incurred by the implementation of guidelines and staff training would be more than offset by the subsequent reduction in complications. He went on to explain that even though medical students are taught the physiology of fluids, there seemed to be a disconnect between theoretical learning and practical application once they graduate to become doctors. In his opinion it was paramount that healthcare professionals understood fluids to be effectively drugs, as therefore their dosage was most important.
Chief executive of the Patients Association Katherine Murphy said it was a disgrace to allow staff to go through their professional life without the right training and support. According to her, the trust boards needed to assign a high priority to this matter as the creation of Nice guidelines required proper implementation in order to be successful.
In June 2013 the Medicines and Healthcare Products Regulatory Agency suspended the use of starch drips in UK hospitals after it was found that the drips were linked to hundreds of unnecessary deaths.
Source: The Guardian
10 December 2013
Latest Articles
IV, IV drips, NICE
A report published by the National Institute for Health and Care Excellence warns that one third of surgery patients' death within days was caused by too m...