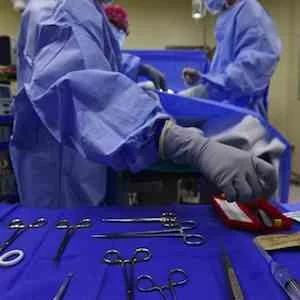
According to a recent study, allowing surgeons-in-training the flexibility to work longer shifts than currently allowed in U.S. and to be able to take less time off between shifts is not associated with greater risk of early serious postoperative complications or death to patients.
The study, called the Flexibility in Duty Hour Requirements for Surgical Trainees (FIRST) Trial, is published in the New England Journal of Medicine.
The study involved 117 U.S. general surgery residency programs and 151 hospitals. The current resident duty hour requirements were compared will less restrictive work hour policies to determine difference in care and outcomes.
"Making duty hour policies more flexible for surgeons-in-training appears to be safe for patients and acceptable to the trainees," said lead study investigator Karl Bilimoria, MD, MS, FACS, a Faculty Scholar at the American College of Surgeons (ACS) and director of the Surgical Outcomes and Quality Improvement Centre at Northwestern University Feinberg School of Medicine in Chicago.
The duty hour policies were revised in 2003 and then again in 2011. Initially, the residents were limited to work 80 hours per week, had capped overnight shift lengths and mandated minimum time off between shifts. Then, again, changes were made that further shortened the shift length for first year residents and increased their time off work after a 24-hour shift. However, Dr. Bilmoria points out that the new restrictions increased the frequency of transferring patients to other care providers. This practice of "handoffs" can compromise the continuity of care and can jeopardise patient safety as well as decrease the quality of education.
The FIRST study analysed the rate of complications among surgical patients in the first postoperative month with the implementation of less restrictive duty hour policies. It also measured residents' perceptions of satisfaction with their overall well-being. Residents were assigned to one of two types of duty hour policies while adhering to the ACGME rules of 80 hours of work a week, one day off in seven and not more than one call at night. One group participated in the Standard Policy group with all existing policies while the other group participated in the Flexible Policy group where they were given the flexibility to implement one or more of the following changes:
- Work shifts could be extended beyond the maximum of 16 hours.
- Senior residents could exceed to 24 hours.
- Residents did not have to follow eight hours off between shift policy and were also not required to have at least 14 hours off after 24 hours of continuous duty.
The results showed that those in the flexible group did not work more hours and were able to work more effectively by rearranging their hours. When evaluating a combined measure of patient deaths and serious complications within 30 days of an operation, the rate was found to similar in both groups at 9 percent. There were also no differences for 10 patient outcomes that were evaluated in the study, including the need for an unplanned second operation.
Residents' satisfaction with the quality of their resident education and their overall well-being was also measured. Those in the flexibility group did not report dissatisfaction anymore than those in the Standard Policy group nor any greater dissatisfaction with their overall well-being. In addition, residents in the flexible group were no more likely than the Standard group to report perceiving a negative effect of fatigue on personal or patient safety.
Overall, the Flexible Policy group reported improved experiences on several measures including continuity of care, operative skills and professionalism. Also, residents in the flexible group were more likely to be present for the entire duration of the operation and were able to care for their patients through an episode of illness instead of handing them off to another provider.
"The results of the FIRST Trial demonstrate that greater flexibility in surgical resident work hours can prevent disruptions in patient care and surgical education, without an adverse effect on patient outcomes," said ABS Executive Director and study coauthor Frank R. Lewis, MD, FACS.
Source: New England Journal of Medicine
Image Credit: Wikimedia Commons


![Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging](https://res.cloudinary.com/healthmanagement-org/image/upload/c_thumb,f_auto,fl_lossy,h_184,q_90,w_500/v1721132076/cw/00127782_cw_image_wi_88cc5f34b1423cec414436d2748b40ce.webp)