Starting 20 May 2020, a new law will be implemented in England regulating a new system of deemed, or presumed consent for routine organ and tissue donation. All adults will be considered to have no objection to becoming a donor after they die, unless they have prior registered their decision to ‘opt out’ or confirmed being part of an excluded group.
You may also like: Caring for Organ Donors in the ICU
It is noted that in England, the new law will apply only to organs/tissues used in ‘routine’ transplants, namely heart, lungs, liver, kidneys, pancreas, intestinal organs, nervous tissue, blood vessels, bone, marrow, tendon, corneas, skin and rectus fascia.
However, the donor’s express consent will still be required for novel or
rare transplants, such as, for example, tissue from sexual and reproductive
organs. In addition, the trachea will be considered as routine only when part
of heart-lung transplantation, and eyes will not be part of face transplants.
The new law, known as Max
and Keira’s law, aims to help the 5,200 people in England who await a
life-saving, or life-enhancing, transplant. Keira Ball was a young girl who passed
away after a road traffic accident in the summer of 2017. Four people were
saved by her donation – her kidneys went to adults, her liver went to a baby
and her heart went to a Max Johnson who was nine at the time. Max Johnson and
his family’s campaigned in favour of an opt-out system for organ donation, and
the law had been eventually changed.
According to Health Secretary Matt Hancock, this step will make organ
donation easier and more available to people in need of transplantation. “Donating
organs will remain a personal decision,” Hancock said. “While the new system
starts in May, people will continue to be able to record their decision to opt
out at any point. It’s important that everyone takes the time to discuss their
choices on donation with their families, whatever their preference may be.”
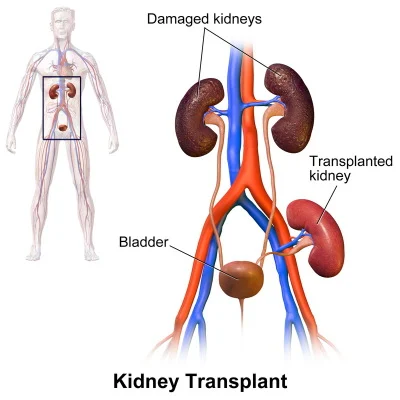
Over 50% of Transplants Are Kidneys
Around 80% of those waiting for a transplant are in need of a kidney, according to Fiona Loud, Policy Director of Kidney Care UK. In the US, for example, in 2019 out of nearly 40,000 transplants, more than half (23,401) were kidney transplants and 872 were kidney/pancreas transplants, and in the waiting list for 123,275 organs, 102,437 were for kidney and 1,796 for kidney/pancreas donation. “Patients have been waiting and hoping for this change, which stands to make a positive contribution to lives and our society, for many years,” Loud said welcoming the introduction of Max and Keira’s Law.
12 March is World
Kidney Day (WKD), a joint initiative of the International Society of
Nephrology (ISN) and the International Federation of Kidney Foundations (IFKF).
It is a globalcampaign that aims to raise awareness of the importance of kidneys
to overall health and to reduce the frequency and impact of kidney disease and
its associated health problems worldwide.
International Experience
In Wales, which in December 2015 became the first country in the UK to move away from an opt-in system in organ procurement, the results have already shown to be positive. Wales now has the highest consent rates in the UK, experiencing more registered donors, fewer family refusals and more living donations. In Scotland, the relevant law will come into force in Autumn 2020. The current legislation for Northern Ireland is to opt in to organ and tissue donation. Notably, the importance of registering deliberate active consent for opting in is highlighted elsewhere.
National donor consent legislations vary
across the world. Spain, where deemed-consent law was passed in 1979, has the
world's highest rate of actual donation. Other countries with similar policies
include Belgium, Austria, France, Columbia, Norway, Italy, Chile and Singapore.
Expressed consent, on the other hand, is required in the US, Denmark, Canada
and Brazil among others.
A 2019 study
compared data on organ donation and transplantation rates for 35 OECD countries
(17 classified as opt-out, 18 as opt-in). It found that opt-out countries had
fewer living donors per million population than opt-in countries, while no
significant difference in deceased donors was identified. Rates of kidney,
non-renal or total solid organ transplantation did not show any substantial
difference between the two groups. The authors suggested that even with deemed
consent regulations in place, other barriers to organ donation must be addressed.
Source: Kidney Care UK
Image credit: by
BruceBlaus – Own work, CC BY-SA 4.0, Wikimedia
Commons


![Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging](https://res.cloudinary.com/healthmanagement-org/image/upload/c_thumb,f_auto,fl_lossy,h_184,q_90,w_500/v1721132076/cw/00127782_cw_image_wi_88cc5f34b1423cec414436d2748b40ce.webp)