HealthManagement, Volume 21 - Issue 7, 2021
Key Points
- Hospitalisation@Home (H@H) will move healthcare towards better sustainability and cost-effectiveness.
- MAFEIP is a web-based financial and quality of life measurement tool that can assess a project’s feasibility for H@H.
- NWE-Chance used the MAFEIP tool for financial modelling to determine H@H’s feasibility for heart failure patients in Belgium and the Netherlands.
Introducing Hospitalisation@Home
Home hospital admissions will help innovate healthcare and move it towards a more sustainable and cost-effective model. The concept, however, is still at an early stage globally, with only a minority of hospitals undertaking hospitalisation at home (H@H) as a usual service offering. Two key challenges in making progress with such an innovation are developing a case for its use at scale and advancing a sustainable business model for the service. To build the case for scale, sufficient evidence is required – financial cost-effective data, being paramount. These challenges are undeniable in Europe – where health systems are fragmented, with many different reimbursement models, organisational processes and procedures, and a wide variety of companies providing technological solutions – when attempting to design a case for scale for H@H services and a sustainable business model.
The NWE-Chance initiative (www.nweurope.eu/nwe-chance) is made up of a consortium of hospitals, industry, and business innovators. Among others, it aims to develop a feasibility study of H@H for heart failure patients (Van der Velde and De Kluiver 2020; Scherrenberg et al. 2021). NWE-Chance searched for an appropriate financial measurement tool to assess the project’s work. The team decided to use the MAFEIP (Monitoring and Assessment Framework for the European Innovation Partnership on Active and Healthy Ageing, www.mafeip.eu) tool to investigate H@H’s financial and quality of life (QoL) aspects. The tool was originally developed with support from the European Commission. Facilitated workshops were led by the Scottish Digital Health and Care Innovation Centre (www.dhi-scotland.com), which used the MAFEIP tool with several key NWE-Chance implementation pilot partners, chiefly hospitals, across the Netherlands and Belgium.
This article explains how the project used the MAFEIP tool to understand better the benefits and impacts of adopting H@H innovations. It shows how data collected in pilot hospital and entered in the MAFEIP tool matters. With appropriate data, it is possible to develop evidence on the cost-effectiveness of the H@H innovation. The MAFEIP tool can also help shape a sustainable business model that can work in different jurisdictions.
What NWE-Chance Is Doing
NWE-Chance addresses the organisational and technological innovations of hospital admissions at home for heart failure patients. NWE-Chance promises the development/optimisation of several integrated eHealth applications (they include blood pressure, weight and oxygen saturation measurements; a vital signs patch for heart rhythm, respiratory rate, posture and activity; plus, an eCoach – a virtual coach). The initiative has a portal for caregivers and a patient app. All have been used to facilitate the admission of heart failure patients
at home.
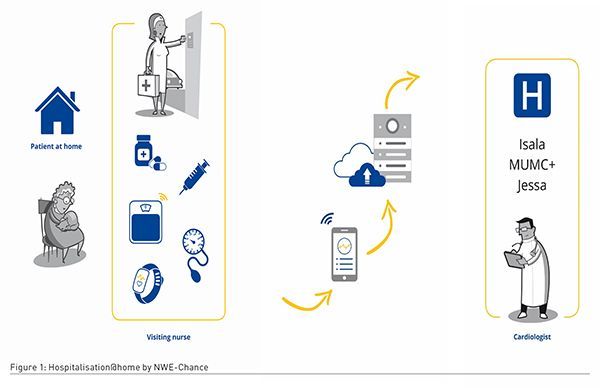
The feasibility of both technology and the supporting care and service process has been tested by three hospitals (each hospital has a different state of organisational readiness concerning home hospital admissions) (Figure 1). The design of the feasibility study has been described by Scherrenberg et al. 2021. NWE-Chance will also launch an innovation hub to bring the stakeholders involved in this organisational shift together: they will share their knowledge concerning home hospitalisations. All these initiatives have been under taken to enable a profound, sustainable transition of the healthcare sector by implementing home hospital admissions at scale.
The MAFEIP Tool
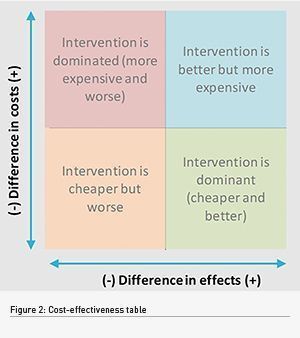
The MAFEIP tool supports evidence-based decision making. Users fill out a range of questions in a web-based application that performs analytic modelling. It presents users with impact assessment health and economic outcome models (value, cost-effectiveness, cumulative utility, transitions between health states, and simulations). Decision-makers need to understand if the intervention will offer good value for the money and is affordable compared to the current service. The diagrams illustrate this concept (Figures 2 and 3). The red and green dots represent examples of outcomes of interventions.
.jpg)
In particular, MAFEIP is helpful for teams and people who have minimum training in economics. MAFEIP allows project teams and their partners to create models that would, otherwise, have to be outsourced to highly-trained and scarce economic skilled staff.
How NWE-Chance Has Used the MAFEIP Tool
The MAFEIP tool permitted the NWE-Chance team to assess the notions of cost-effectiveness, scale, and new business models. The MAFEIP tool guided the NWE-Chance consortium to evaluate the cost-effectiveness and potential impact.
NWE-Chance has, however, used only a limited part of the total functionality that the MAFEIP tool has to offer, and instead concentrated on models for cost-effectiveness and cumulative utility. The partners did not utilise MAFEIP’s full simulation functionality. In total MAFEIP has five stages. The NWE-Chance project used only the first three out of these five; this restriction was due to the limitations on the project’s data availability from the pilot sites. Nevertheless, NWE-Chance was able to run a full model of the data that it had collected to analyse the intervention’s impact.
Data Required for the Intervention Analysis
NWE-Chance ran two MAFEIP related workshops with partners. The workshops’ purpose was to ensure all data input was completed and validated, and that there was a general understanding of data input sources and assumptions being made. The pilot sites which tested the MAFEIP tool were hospital partners Isala and Maastricht University Medical Centre (MUMC) in the Netherlands and Jessa in Belgium.
The MAFEIP tool is organised into a five-stage process. The use of the step-by-step web-based tool was facilitated by the Scottish Digital Health and Care Innovation Centre, whose staff consulted with project partners to answer each of the questions. The tool supported the team members analysing the outcomes and, where necessary, linked to national database sources for the specific country of interest.
Stage 1 – the first three key questions to be answered by the NWE-Chance team relate to the:
- H@H interventions’ Characteristics and aims (this included the project name, which action group it came under, target population such as demography, geography, condition focus, and disease characteristics.
- Description of the intervention (device or/and protocol, clinical implementation, current care state impact on health and resource use in comparison to the current state and the stage of the project (trial, clinical trials ongoing, pilot implementation, routine use etc.).
- Evidenced collected (empirical and/or alternative evidence on effectiveness, impact on resource use, study design, control group, number of patients, empirical or/and alternative health-related Quality of Life (QoL) data – called HRQOL).
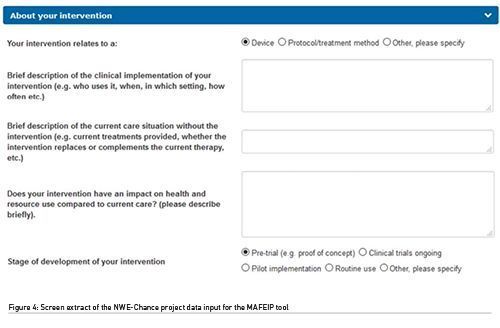
This first data collection stage (Figure 4) was relatively easy to complete for the NWE-Chance partners. However, there were gaps, empirical and alternative evidence on effectiveness and study design. Completing the tool at this stage was a challenge for a variety of reasons. The difficulties included the fact that NWE-Chance had no control group (the control group data input collected and referenced from national statistical databases - general information available at a population level) with which to compare the pilots, and no specific HRQoL data available to reference.
Stage 2 – questions at this point focused on how the intervention had been set up. This included:
- Discount factor (discount rate should equal the level of return that similar stabilised investments are currently yielding) for cost and utility.
- Target population data (minimum and maximum age, gender, country, and currency).
- Patient flow (where the NWE-Chance group could be specific about age and gender of patients if required).
This stage of the tool was easily answered. With direct data input from the split studies having been collected, it was therefore completed in a straightforward manner.
Stage 3 of the MAFEIP tool concentrated on probabilities using the Markov model (Boehler et al. 2015), which considers three states - ‘Baseline’, ‘Disease impaired’, and ‘Dead’. These states are categorised into two groups, a control group and an intervention group. They were arranged to examine the initial distribution among the states. In addition, the tool allowed the NWE-Chance partners to consider the transition probabilities as per average incidence of disease occurrence and recovery for this cohort, as per the control and intervention groups. For our intervention, this refers to the baseline state patients with chronic heart failure that don’t need hospital admission and the disease impaired state patients with chronic heart failure that are hospitalised (at home).
The data for the control group for the NWE-Chance project was referenced from general population statistics and publications on heart failure. Therefore, assumptions were made as per generic referenced data sources for the control group. It should be noted that the NWE-Chance project did not possess data on project-specific mortality (relative risk for mortality in both control and intervention group states). As a result, NWE-Chance opted for general mortality rates linked to human mortality as per a standard database, specific to the country of choice declared as part of the input at Stage 1 of MAFEIP tool. This was why the project workshop and tool had to be used as separate instances, once for the pilots in the Netherlands and then separately for the Belgium pilot. NWE-Chance Belgium pilot focused on Flanders (a region in Belgium). It should be noted that the MAFEIP tool does not go down to the granular level of a specific region in a country.
Other key cost data was required at this stage (3), including healthcare-associated costs (resources used within the healthcare system along with the societal costs). This data was provided by project pilot leads, based on a combination of population statistics (societal costs and project information - resources). If the healthcare data had not been collected at the pilot sites, then this task and input would have been made more difficult. Retrospective data collection would have been required.
Data Assumptions Made by the NWE-Chance Project Partners
Several assumptions had to be made to fulfil the data inputs needed by the MAFEIP model. The partners had either collected specific data themselves or, due to their knowledge of the two countries’ contexts, they could cite information from key publications and national statistical databases. This approach ensured data was reliable and referenced. For both countries, the data input included data on mortality rates, costs of standard care, and incidence prevalence specific to heart failure (which was the disease group focus of the NWE-Chance project).
How NWE-Chance Used the MAFEIP Model to Develop Financial Models
Using the MAFEIP tool in NWE-Chance allowed comparisons to be made between the results measured in the Netherlands and Belgium. More specifically, we analysed the relation to the intervention state (i.e., NWE-Chance apps and technologies) versus the control state (traditional model of care). The measurements occurred in respect of the expected impact in terms of Incremental Effects by Age, Cost-Effectiveness, and Alive states. They are illustrated by three figures divided by country: Incremental cost and effects by age (Figure 5); the healthcare Cost-Effectiveness plane (Figure 6); and patient flow for Alive states (Figure 7).
Benefits of Using the MAFEIP Tool and Next Steps
The NWE-Chance project partners have found MAFEIP a useful tool. It has helped them by highlighting how to undertake initial assessments on whether the H@H heart failure intervention is effective in cost and value. It shows how the intervention and its outcomes differs in each country, with different contexts, and costs taken into consideration in the MAFEIP modelling algorithms. Isala hospital clinical colleagues stated: ‘We will use the MAFEIP outcomes for the development of a business plan for the H@H platform. Furthermore, MAFEIP really pointed us to some opportunities for our future use of H@H.’
Overall, the project partners felt the tool was of interest to both healthcare providers and digital technology providers in moving forward innovations in this field and cases for scale.
The next stage for NWE-Chance is to review the modelling outputs in more detail; this deeper insight will help the team to create different future costing scenarios for the financial models. As a result of such an investigation, the NWE-Chance partners could then optimise the value and return for the person, healthcare partners, and society.
Conclusion
At the end of feasibility projects, decision-makers often say, ‘show me the money’. As it moves towards a more mature state of readiness and case for scale, this question becomes more acute. This relates to firstly how much it will cost and how it compares to the existing service costs, and secondly with a focus on how effective it is in terms of the Health-Related Quality of Life (HRQoL) for patients. These models are difficult to produce when there are no in-house economic experts who can undertake economic modelling. At the feasibility stage, there is often not an extensive budget to commission such expertise, which is usually not readily available due to high demand and being cost-prohibitive.
Therefore, the ability to create economic modelling by project teams with the MAFEIP tool is advantageous. With projects partners that often can input the data easily, this tool with its embedded algorithms has allowed the partners to extract insights from the MAFEIP models to understand the initial financial effects of the intervention. This will allow the consortium to create future scenarios for the target patient population of the intervention and the best business model for service and commercialisation purposes. It is well recognised that to scale digital health in healthcare, the finances need to ‘add up’. An early indication that a new service is cost-effective is key. Providing this reassurance for decision-makers at this stage will prepare a route for a future case for scale to be developed for our and other initiatives.
Acknowledgements
NWE-Chance has received funding from the Interreg NWE Programme under grant agreement number NWE 661.
Conflict of Interest
None.
References:
Boehler CEH et al. (2015) Development of a web-based tool for the assessment of health and economic outcomes of the European Innovation Partnership on Active and Healthy Ageing (EIP on AHA). BMC Med Inform Decis Mak, 15(3): S4.
EHTEL (2020) How hospitals at home can benefit from digital therapeutics: An EHTEL factsheet. Available from www.ehtel.eu/images/220620_EHTEL_Digital_Therapeutics_factsheet_DEF.pdf
Scherrenberg M et al. (2021) Home hospitalisation strategy for patients with an acute episode of heart failure using a Digital Health supported platform: Multicentre Feasibility study - Rationale and study design. Cardiology.
Van der Velde AE, De Kluiver EP. (2020) Innovating in healthcare: hospital admissions at home. HealthManagement 20(8).
Project References:
NWE-CHANCE Project - www.nweurope.eu/nwe-chance
MAFEIP Tool - Monitoring and Assessment Framework for the European Innovation Partnership on Active and Healthy Ageing - http://mafeip.eu/





