HealthManagement, Volume 21 - Issue 4, 2021
The Telemedicine Community Readiness Tool proves its worth in supporting communities internationally on their journey towards expanded telemedicine use.
Key Points
- Empowering communities, while preparing for long-term telemedicine implementation and use, is vital. It can encourage telemedicine deployment during ongoing waves of the COVID-19 pandemic.
- The Telemedicine Community Readiness Model (TCRM) gives communities a tool to create a favourable environment for telemedicine.
- The TCRM been tested internationally and is available free of charge.
- Personas are a useful change management tool. Further focus on professional personas is needed to consider the professional perspectives in health, care, and management when working on improving telemedicine.

Supporting Telemedicine Implementation During COVID-19
Use of telemedicine has increased rapidly in 2020/2021 due to the special situation created by the COVID-19 pandemic. To enable this increase, various barriers have been lowered temporarily e.g. the removal of blockages to financing and inter-jurisdictional use (Bokolo 2020). To sustain the use of telemedicine, however, longer lasting business models that are not based simply on exceptional circumstances are needed. These are business models which can operate at the level of individual telemedicine solutions and can, in turn, be more widely supported by communities. Hence, communities can be empowered, thereby helping them to prepare for long-term telemedicine implementation and use. To this end, a telemedicine community readiness model (TCRM), based on earlier Momentum Blueprint work (Jensen et al. 2015), has been developed and is available for use free of charge. Using the steps of the model will help to encourage the scaling-up of telemedicine innovations. This model has already assisted several communities – in Australia, Croatia, and Scotland – to identify key aspects of their own telemedicine success stories. Further experimentation, and development of tools, is now taking place in the context of other scaling-up exercises. Implementing the TCRM could really help to encourage telemedicine implementation in the future, including during any ongoing waves of the COVID-19 pandemic.
Telemedicine in 2021 and Beyond
During 2020, there were many telemedicine innovations. Internationally, increasing numbers of telemedicine solutions were put in place, including in the field of mental health (Folker et al. 2021), and they were utilised for many reasons outside of social distancing and the special circumstances posed by the COVID-19 pandemic. Innovations began seemingly overnight. Barriers that had previously been assumed to exist were suddenly overcome, because COVID-19 did not leave citizens and organisations with many other alternatives. What can, however, be perceived from former pandemic or epidemic situations based on other respiratory conditions like SARS or MERS, is that an increase in innovation and continued use of telemedicine is rarely sustained after the special situation ends (Reifegerste et al. 2021).
The COVID-19 situation has taught us three main lessons. First, we have learned that there is a continuing need to focus on telemedicine use, including how it can be integrated together with real-life (physical) appointments and treatments. Second, we should empower stakeholders – as well as communities – to develop long-term strategies to implement telemedicine initiatives successfully. Third, we should create environments which make it easier to scale-up telemedicine initiatives in scope and number. Most likely, ‘hybrid care’ will become a core endeavour – bringing together virtual and physical health and care encounters. Tools that can help communities engage will be essential in ensuring a smooth implementation.
The Telemedicine Community Readiness Model (TCRM)
The Telemedicine Community Readiness Model (TCRM) underpins telemedicine development by communities and stakeholders. The TCRM was developed to support communities – and stakeholders in those communities e.g. community representatives, legislative institutions, and payers – to create a favourable environment for implementing and scaling-up telemedicine. It is a valuable tool that helps to assess and improve the status quo for telemedicine in communities that can be connected locally (e.g. regions or health networks) or through a shared concern (e.g. a common disease). The model consolidates research on telemedicine barriers, and success factors for telemedicine implementation, e.g. by incorporating the findings of the Momentum Blueprint (Jensen et al. 2015; Whitehouse and Lange 2017).
How to Use the TCRM?
There are three main steps to using the TCRM. First, the TCRM guides users through a series of questions that help them to assess the status of telemedicine initiatives, the involvement of users in the community, and the level of evidence generated on what kinds of telemedicine projects already exist in the community. These questions help people to rate their community according to a particular level, in terms of their telemedicine adoption “as is” (today) (see Figure 1).
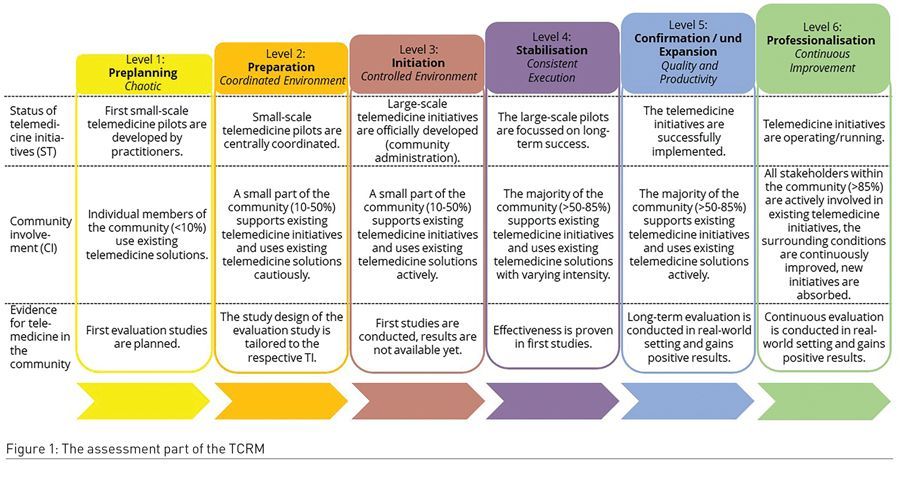
Second, based on the rating, the TCRM proposes specific improvement aspects that help the community to be better prepared to implement telemedicine successfully. Third, community stakeholders work together to develop a specific strategy for how to put the proposed improvement aspects into practice. These community stakeholders can include a wide range of people e.g. representatives from communities, payers, healthcare professionals, technicians, or others using telemedicine.
Who Can Use the TCRM?
The TCRM aims to empower representatives in communities to get their community ready for the successful implementation and scaling-up of telemedicine initiatives. The TCRM can be used together with the appropriate personas.
Ella is one of the Blueprint personas which were designed to help understand the profiles of people focusing on improved health and care, often by using digital technologies (Blueprint personas 2021). Ella can serve as a supporting persona for other communities, initiatives, and projects that want to include a professional perspective in their work.
As head of digital healthcare innovations in a rural community in Eastern Saxony, Germany, Ella is a good example of a community representative. The community she works and lives in is characterised by its long distances from the clinics or hospitals where patients must visit medical specialists. As part of her work, Ella aims to introduce telemedicine solutions into her community to lower the burden of the effects created by the decreasing number of clinical specialists working in Saxony. Even though it is sometimes challenging for Ella to work with the health professionals in her community – especially as the older ones remain reluctant to change – she is thrilled to be able to build an environment in which professionals and users are involved and are motivated to use telemedicine. Ella uses the TCRM to get inspired as to what she can do specifically to reach her aim of improved care delivery in her community (Figure 2).

International Use of the TCRM and its Success Factors
The TCRM has now existed for over two years. It has been evaluated at several stages during its development in differing communities in Australia and Germany by healthcare professionals, representatives of health insurance companies and network organisations in healthcare. Now, it is available free of charge as a web tool. It is accessible to anyone who is searching for support on telemedicine deployment in his/her community.
During the winter of 2020-2021, sites in Australia, Croatia, and Scotland tested the model. The communities in these three countries were all at level 4 (‘stabilisation’) of the TCRM, meaning that they were consistently employing telemedicine, and had already implemented several telemedicine initiatives in which more than half of the people within the community are now involved. Challenges around confirmation, expansion, and professionalisation remain for these test sites, denoting the shift needed to levels 5 and 6. All three sites are highly interested in generating evidence that their telemedicine initiatives serve the communities as intended. They have conducted at least some first evaluation studies. Based on an initial assessment of their status quo, various actions have been identified that can help further improve the telemedicine implementation in all of these communities. The three countries’ best practices and successes in reaching a level of stabilisation in their work (level 4 of the TCRM) follow.
Australia: The Australian community involved people with an Aboriginal background and racial diversity. Australia is a country with several states. The community benefitted from the following five practices, among others:
- Stakeholders designed the layout and settings on mobile devices based on citizens’ needs.
- Aboriginal team members were involved to ensure culturally appropriate communication with users.
- Focus was placed on partnerships with state-wide services.
- The infrastructure used was interoperable.
- Technical needs were very much driven by the clinical use case described by the community, and not by the available technology.
Croatia: Croatia focused primarily on cooperation and involvement. Among other activities, it conducted co-development workshops with relevant stakeholders (including software developers, doctors, nurses, patients, and policy makers). Implementation was supported thanks to a pre-existing framework for telemedicine reimbursement, which meant that adequate financial resources were available for telemedicine initiatives.
Scotland: The Scottish community experienced provision of adequate financial resources, with developments occurring at the national level and in a national context. Government Funding and Local Health Board resources were helpful in implementing telemedicine initiatives. A Scottish government programme exists which defines a sustainable scaling-up strategy necessary to implement and scale-up telemedicine initiatives in the long-run.
Other sites continue to download and use the TCRM.
Next Steps With the Use of the TCRM
In addition to the success factors presented, the TCRM helps mainly in identifying aspects for improvement which consist of hard and soft factors. Specific ‘hard factors’ (e.g. infrastructure, resources) and ‘soft factors’ (e.g. vision, awareness) are proposed by the model, which help each community to mature towards a state where it is easy to implement telemedicine initiatives.
Communication is also important. The TCRM supports communication among all of the stakeholders involved in a community by providing a unified understanding of their situation in order for them to work together
seamlessly.
Since the TCRM is now in active use and freely available, it will serve as a knowledge base for sharing best practices in capacity building among communities regarding telemedicine initiatives. By offering such support to communities, an implicit aim of the model is to help in sustaining the increased use of telemedicine throughout ongoing waves of the 2021 COVID-19 pandemic and in the years beyond. The Helict team of TU Dresden, as part of the reference site of Saxony, is always happy to assist other regions that need support with using the TCRM. For more information on the work of Helict, please visit their webpage.
The TCRM is one of several tools that are undergoing revision and expansion, with a view to their extended use in the future. Two others are the SCIROCCO Exchange tool and the Momentum framework (Jensen et al. 2015). EHTEL and its members – including people from the region of Saxony in Germany – are keen to support digital health advances. For more information on the work that EHTEL has been conducting, in this time of opportunity and challenge, visit its Imagining 2029 webpage dedicated to digital health and its COVID-19 webpage. Hybrid care is one of EHTEL’s current work streams.
Conflict of Interest
None.

References:
Blueprint personas. Blueprint Personas. Spin-Off Personas. https://blueprint-personas.eu/spin-off-personas/ (2021)
Bokolo, A. Jnr. Use of Telemedicine and Virtual Care for Remote Treatment in Response to COVID-19 Pandemic. J Med Syst 44, 132 (2020). https://doi.org/10.1007/s10916-020-01596-5
Folker, M.P., Nielsen, S.L., Craggs, M.A. Harnessing the Potential of Technology for Mental Healthcare. Health Management. 21, 3 (2021)
Jensen, L.K., Knarvik, U., Pedersen, C.D., Tangene, W., Whitehouse, D. Deliverable 3.4 Personalised Blueprint for telemedicine deployment: validated and tested version (2015).
Reifegerste, D., Harst, L. & Otto, L. Sauerbruch, STARPAHC, and SARS: Historical Perspectives on Readiness and Barriers in Telemedicine. J Public Health (Berl.) (2021). https://doi.org/10.1007/s10389-021-01513-1
Whitehouse, D., Lange, M, ‘Good practice in change management. Deploying telemedicine service at large-scale’. Telemedicine: Improving Health Security in the Balkans. IOS Press: Amsterdam, Netherlands, 111-121 (2017).





