HealthManagement, Volume 21 - Issue 1, 2021
In the world of modern healthcare, especially since the start of the COVID-19 pandemic, the understanding of interaction between healthcare professionals’ burnout, morale and competence level is key to improving the quality of care and decrease staff turnover. A team of experts investigate this complex area and question some current practices of competence acquisition.
Key Points
- How competency affect our frontline staff is the main question to be asked by any organisation.
- Burnout is a major problem among healthcare professionals.
- Competence acquisition needs to be balanced in terms of theory, mentoring and experience in line with the 70-20-10 model.
- Current inadequate models of competence acquisition lead to exhaustion, frustration and retention among nurses.
- Increased standardisation in competence and skill acquisition may help to improve quality of care.
Everyone has heard of ‘competency’. But what exactly is it? Let us start with what it is not. It is not the typical skills checkoff, traditional e-learning, or what we like to call the ‘great paper chase’ that happens right before annual reviews happen. You know what we are talking about; the pages of ‘competencies’ staffers must complete before their annual review that they wait until the last minute to complete. We already know that a lack of competence leads to poor patient outcomes and poor-quality care. What we need to question is how does competency affect our frontline staff? Does competency create less stress, less burnout, or greater satisfaction for the staff? Does this lead to the ultimate question: Does it decrease turnover? These are the elements this article will be discussing based on a literature search.
To decide if competency does affect all of these things, we need to first start at the beginning by defining the key principles.
Burnout: Sources, Development and Consequences
There are several definitions of burnout. The term describes a state of illness. People with burnout are completely exhausted – physically, emotionally and mentally – and performance is significantly reduced. The description has given the disease its familiar name: burnout syndrome. It is also known as stress syndrome. According to the World Health Organization (WHO), burnout is not a disease, but a problem “related to lifestyle difficulties” (WHO 2019).
The term ‘burnout’ first appeared in the U.S. in the 1970s. The psychotherapist Herbert Freudenberger described the consequences of heavy stress in the so-called helping professions. According to this, doctors and nurses who sacrifice themselves for other people through their work are often ‘burned out’. This manifests itself in exhaustion, excessive demands and listlessness (Institute for Quality and Efficiency in Health Care [IQWiG] 2020).
Burnout runs in a cycle with 12 stages (Freudenberger 1975) but individual stages can be skipped. The main component is the continuous deterioration until, in the end, it is hardly possible to distinguish it from severe depression. The first part of it is the Alarm Reaction and includes the compulsion to prove oneself (1), working harder (2), and neglecting their own needs (3) and displacement of conflicts and needs (4). The next part is the Resistance Phase and includes revision of values (5), denials of problems (6), withdrawal (7) and obvious behavioural changes (8). The final phase is the Exhaustion Phase which starts with depersonalisation (9), inner emptiness (10), depression (11) and finally the burnout syndrome (12).
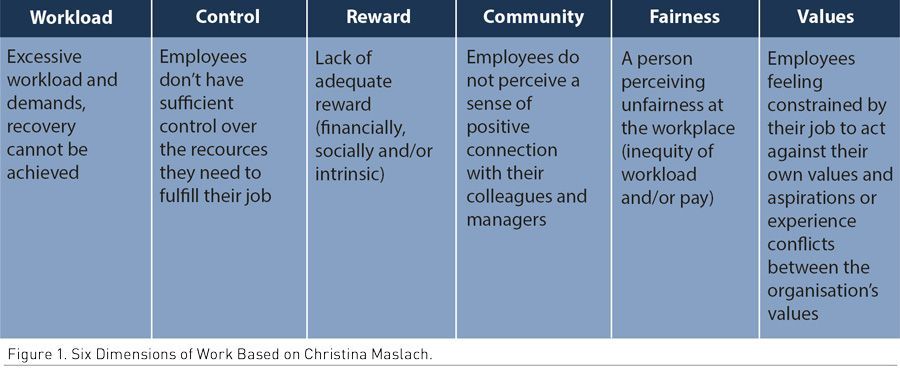
Christina Maslach (Social Psychologist U.S.) theorised that burnout was a state that occured because of a prolonged mismatch between a person and at least one of six dimensions of work (Figure 1). In addition, there are more and more developments of burnout outside of normal work processes, especially in circumstances of associates who take care of people in need at home (Maslach and Leiter 2016).
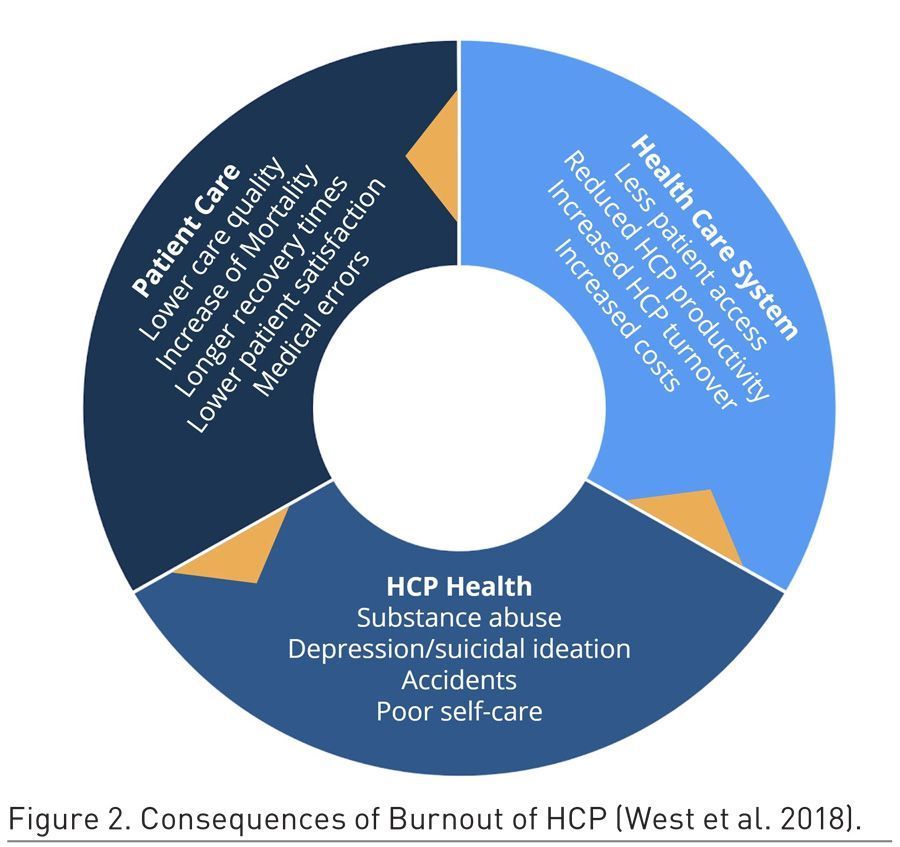
The presence of burnout among healthcare professionals (HCP) is associated with worsening patient safety, the weakness of the healthcare system – including suffering of the individuals themselves – and increasing shortage of HCP (Figure 2).
Competency Acquisition in Healthcare
The interest about our knowledge, skills and competencies goes back to the ancient history of early philosophers. Still today, understanding the nature of competencies and its impact on outcome is and should be on top of any organisation’s agenda. However, there has been huge progress on understanding the nature of competencies, knowledge on how we learn, and how competencies are transformed into high-quality outcomes.
In ancient times, the transfer of competencies was primarily done by learning from the masters. The one and only way to become a blacksmith was through an apprenticeship, learning by closely mentoring the tacit knowledge (Polanyi 1966) of the right temperature for iron to be shaped into essential tools for society.
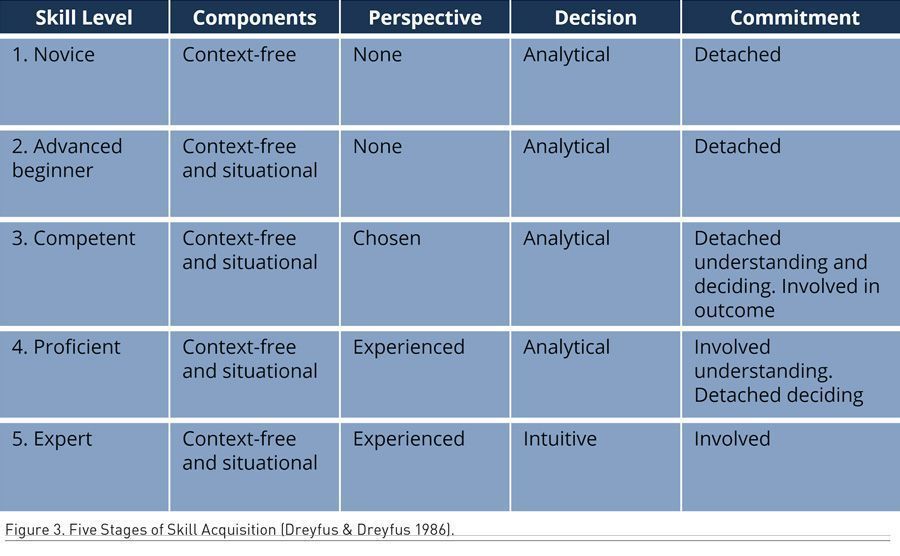
This key principle is the same one we base all our residency programmes on today. While acknowledging that courses and theoretical knowledge do not make a competent HCP, it can take one to the level of ‘advanced beginner’ (Dreyfus 1986) by knowing the subject matter (Figure 3). But it lacks the situational contexts, holistic perspective such as the entire patient journey, and understanding of outcome.
Link Between Competency and Retention
More recently, the 70-20-10 model for learning and development has been suggested by Lombardo and Eichinger (1996) to explain that theoretical learning covers only 10% of the learning while the last 20% and 70% of the competence acquisition come from mentoring and experience over time, respectively. In the healthcare setting, the residency programme fills in the 20% of mentoring, oftentimes in a very structured manner. The latter 70% of the learning journey is what evolves over the course of becoming an experienced practitioner (Lombardo and Eichinger 1996).
Nurse turnover and the retention of healthcare staff in general is a well-founded and global concern. According to a 2019 survey of 424,284 U.S. healthcare workers, the average nurse turnover calculated to 17.1% annually while as much as 89% of the total staff at an average hospital has shifted since 2015. These numbers are from prior to 2020 and do not include the impact of COVID-19. The same survey uncovered that more than 21% of all newly graduated nurses quit their jobs within the first year. We need to investigate the 5- to 10-year experience to lower the annual turnover rate to less than 15%.
Drawing the line back to the 70-20-10 learning and developing model indicates an interesting and well-spoken correlation: nurses as well as other healthcare workers need to learn swimming in deep water is unsuccessful. Literature (Polanyi,1966; Dreyfus 1986; Lombardo and Eichinger 1996) shows us there is no good reason to believe that our ‘superheroes’ are competent at this early stage of their careers. Clearly, the lack of competence causes frustration, disappointment and exhaustion, resulting in an unfortunate separation of employment.
Europe vs. U.S.: It is About Quality of Care
Competencies and skill acquisition in European healthcare specifically have been studied more closely by Patricia Benner (1984), building up on Dreyfus (1986) explaining nurse’s competency through experience (learning ‘how to’) without the theoretical (‘knowing that’) knowledge being taught. While Benner has gained much attention in Europe, Donna Wright’s Competency Assessment model (2005) is more widespread in the U.S. The competency model is supposed to form a more standardised approach to competence to ensure quality of care and draws the link from competencies at the point of care to patient outcome. It ties in with the increasing push for the value-based healthcare (VBH) model (Porter 2010) that has enforced the finance and reimbursement model by Medicare in the U.S. It is also suggested for Europe by Porter (2010) as a response to the strain on health budgets caused by an ageing population, more chronic conditions, and higher cost of care driven by more advanced treatments available.
With the tight link between competency and quality, is it likely to suggest that downplaying the need for competency development, particularly in early years of nursing careers, causes reduced quality of care and outcomes. Which, again, leads to exhausted staff, increased turnover, and negative impact on competencies as a closed loop.
So, what can we do about this? How do we handle stress and this dreaded burnout that looks like it is bound to happen across the world as our healthcare systems are overrun with sick people? In the next article, next month, we will discuss some tools to use to decrease burnout, increase staff morale, and decrease turnover.
Conflict of Interest
None. 
The authors would like to thank Aaron Greenfield from Tampa, Florida, USA for completing an editor duty on the article before it was sent over to the Publisher.
References:
Benner, P. E. (1984). From novice to expert: Excellence and power in clinical nursing practice. Menlo Park, Calif.: Addison-Wesley Pub. Co., Nursing Division.
Dreyfus H. (1986) Mind over machine (Reprint ed.). New York: Free Press.
Freudenberger HJ (1975) The staff burn-out syndrome in alternative institutions. Psychotherapy: Theory, Research & Practice, 12(1):73–82.
Institute for Quality and Efficiency in Health Care (IQWiG) (2020) Depression: What is burnout? In InformedHealth.org [Internet]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279286/
Lombardo M, Eichinger R (1996) Career architect development planner (1st edition). Minneapolis, MN: Lominger Limited.
Maslach C, Leiter M (2016) Chapter 43 – Burnout. In Stress: Concepts, cognition, emotion, and behaviour. Ed. George Fink. Handbook of Stress Series, 1:351-357. Cambridge, MA: Academic Press.
Polanyi M (1966) The tacit dimension (1st ed.). London : Routledge & Kegan Paul.
Porter ME (2010) What is value in health care? N Engl J Med, 363(26):2477-81. Available from http://vbhcprize.com/wp-content/uploads/2014/03/Porter-What-is-value-in-healthcare.pdf
West CP et al. (2018). Physician burnout: Contributors, consequences and solutions. Journal of Internal Medicine, 283(6):516–529.
World Health Organization (2019) Burn-out an "occupational phenomenon": International classification of diseases. Published 28 May. Available from https://www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases
Wright, D. (2005). The ultimate guide to competency assessment in health care, third edition (wright, ultimate guide to competency assessment in health care) (3rd ed.). Creative Health Care Management.





