HealthManagement, Volume 21 - Issue 6, 2021
Key Points
- Care anytime, anywhere: Providing patients with seamless access to their health information, with personalised prompts customised to patients’ health concerns, encouraging patients to more proactively manage their own health.
- Clinical decision support and partnership: Integration with clinical systems would allow real-time sharing of patients’ health information with other healthcare providers, which in turn, supports clinicians’ decision-making and collaboration to improve patient care beyond the hospital.
- Productivity and role redesign: Through digitalisation, time saved on attending to patient registration and payment can be used for patient service associates (PSAs) to upskill their competencies as part of their career development and progression, and ultimately to provide value-added services (VAS) to patients. The PSAs can embark on basic nursing and allied health competencies and in turn, the nurses and allied health professionals may progress to focus more on higher-level acuity proficiencies.
Programme Infrastructure
At TTSH, we have taken a modular, stackable approach in building the programme infrastructure. The ambulatory care digital stack is built on a common infrastructure, HealthHub, a one-stop portal and mobile app jointly developed by the Singapore Health Ministry and Integrated Health Information Systems (IHiS), the national technology agency for the public healthcare sector. HealthHub provides Singapore residents online access to their health records and relevant health content, with the view to improve their health literacy and encourage adoption of healthy lifestyles.
HealthHub is linked to SingPass, with a base to house datasets managed by existing hospital IT systems. SingPass stands for Singapore Personal Access, a secure online platform by which Singapore residents can access Singapore government e-services. SingPass is managed by the Government Technology Agency of Singapore (GovTech), the designated governmental agency which provides the national-level infrastructure to harness infocomm technologies, networks and big data to create tech-enabled solutions.
A digital “marketplace” platform sits on top of this common infrastructure where modularised tools and services will be available for selection and stacking to build new application functions rapidly, and add on other functions befitting to new needs. Leveraging on common national-level infrastructure reduces the development time, as there is no need to build an application from scratch and also future-proof its usability. This approach will allow us to focus on designing and customising emerging solutions, without having to worry about the underlying infrastructure.
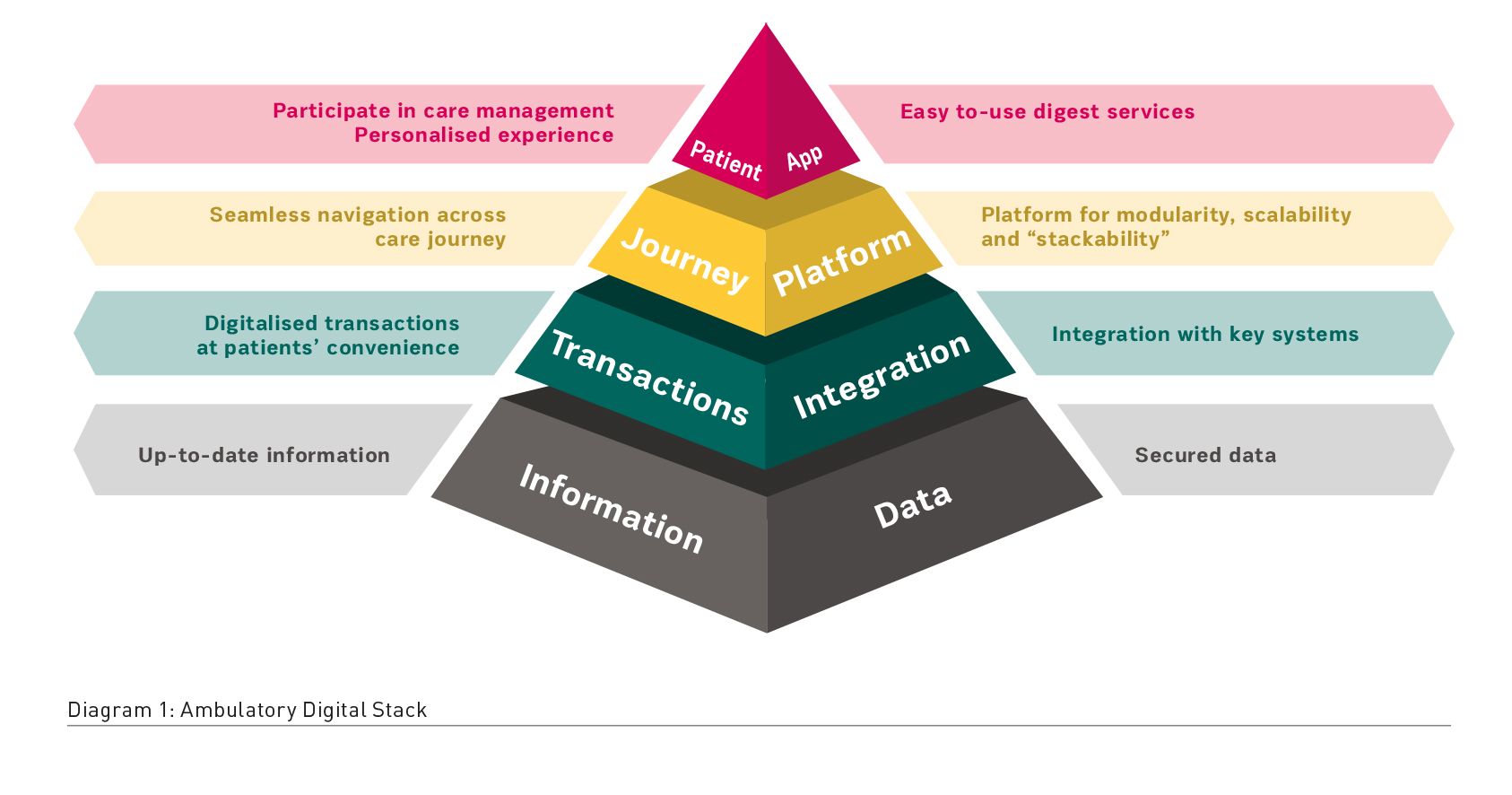
Key Features
The digital stack is mapped to mirror the patient perspective and aims to deliver the care model through three strategic thrusts, MyAssistant, MyHealth, and MyGuide. Each thrust is tailored to provide the patients with personalised access to ambulatory care.
MyAssistant (rollout between FY20 to FY22) consists of features that allow patients to manage their essential outpatient clinic transactions such as registration and e-payments, giving them better control of their schedule. An e-itinerary for the upcoming visit and queue status keeps them informed by providing them with up-to-date information. Profiling of their digital identity will help us better understand their preferences so that we can better personalise their care and experience:
Registration: Much like the online check-in process before a flight, patients can choose to register on the mobile app ahead of their clinic appointments to minimise their waiting time at the clinic.
Queue Status: Leveraging on the mobile queue itinerary, patients know how many people are ahead of them, giving them better control of their schedule.
E-Payment: Patients can leave the hospital straight after their medical consultations without having to queue at a counter using their phones.
Personal Profile: Patients can update their personal particulars any time through the application to ensure that they receive the latest notifications and allow us to deliver more targeted healthcare to them.
Appointment: Appointment rescheduling and cancellation can be performed at a touch of a button without waiting on the line to speak to an operator during peak hours.
Under MyHealth (rollout between FY20 to FY24), patients will have access to their health and medication records, diagnostic results, order a resupply of medication, improve their health literacy and even activate teleconsultation. These features are designed to support patients to take better ownership in managing their health:
Health Records Management: Patients would be able to access their personal health records from their mobile app.
Diagnostic Results Management: Results from diagnostic investigations would be accessible on the mobile app, shifting away from reliance on physical records.
Prompts: Other than appointment reminders, prompts will also include fasting instructions, no-driving reminders, and customised education content based on the patient’s customised profile to help them manage the health challenges that they face.
Health Journal: The app can serve as a platform to encourage relationship-based care between the patient and clinicians. Patients can connect wearable devices and connected medical devices to record their health information, journal their day-to-day symptoms and capture information that may be related to their condition such as exercise, sleep, diet, hydration etc. In return, we could help them analyse the data in the context of their overall health to generate personalised insights and digital prescriptions on the app. Clinicians can also utilise the additional information, aided by visualisation and machine learning tools to better understand their health needs and behaviour. This can eventually lead to precision medicine and personalised care.
MyGuide (targeted rollout in FY23 and beyond) features functionalities such as indoor navigation, car finder and an events portal, which support patients and visitors to effortlessly navigate between their homes and hospital. Beyond physical navigation, integration of billing and insurance systems could allow automatic e-submissions of insurance claims for hospitalisation expenses. Other potential applications include allowing patients to check their eligibility, and apply for healthcare subsidies, financial aid or other grants without having to provide supporting financial documents. Such end-to-end solutions would ensure that nobody in need of healthcare would be deprived due to administrative or financial constraints.
In line with our overarching model of leveraging on national-level IT infrastructure, these features should be integrated with existing applications, which would allow patients to search for government, social and wellness services near their homes. With access to these applications, patients would have ready access to information, such as services offered by social service agencies, health-promoting activities and events. Here are two examples of such applications which fit this model:
LifeSG app: It allows users to access over 40 government services, ranging from checking their eligibility for subsidy and support schemes, assistance with job search, housing matters, to financial and legacy planning.
Healthy 365 app: Managed by Singapore Health Promotion Board, this application aims to encourage users to adopt a healthier lifestyle by availing a calendar of complimentary health activities (e.g. Pilates, kickboxing, Zumba etc) and a National Steps Challenge to encourage physical activity. This is complemented by an incentive structure to encourage participation.
Future Plans - Potential and Possibilities
The features above describe mainly transaction-level and selected journey-level interactions. These functions lay the foundation for broader clinical integration with other SIPs and the Next Generation Electronic Medical Record (NGEMR).
Each SIP focuses on a different aspect of patient care transformation such as inpatient care, resource monitoring and utilisation and others. The NGEMR is a critical piece of Singapore’s healthcare IT infrastructure, serving as a centralised platform which records the entire patient journey from the point of admission to discharge, including both medical and administrative data.
Providing healthcare providers across different settings (e.g. primary care, intermediate and step-down care and the community) with real-time access to pertinent medical information will promote more informed decision-making and foster stronger provider-provider collaboration for seamless care delivery beyond the hospital.
Another exciting aspect is the potential of harnessing artificial intelligence capabilities to derive predictive clinical insights. A machine learning algorithm could be developed to analyse multi-dimensional facets of an individual patient’s health data (e.g. biomarkers, healthcare utilisation or health behaviours) to identify patterns or antecedents leading up to an acute health episode, which would then trigger personalised prompts to the patients or alerts to designated healthcare providers for early intervention. These prompts would also be applicable in preventive health, such as when they are due for health screenings or to remind individuals with a positive family history to seek targeted screening and early medical attention.
Fundamentally, the goal of healthcare digitalisation is towards the betterment of patients’ health outcomes. We aim to generate tailored health insights to educate and empower individuals to become activated agents who take charge of their own health, so that they stay healthy as long as possible and help them integrate it into their busy lives.
Impact on Patient Experience and Workforce Transformation
While CoW leverages on digital tools, it is by no means an IT project alone. Rather, it supports the shift towards a relationship-based clinical model with a view to provide a personalised and enhanced patient experience. The business model that supports and complements this relationship-based clinical model drives the phases and thrusts of CoW. Innovation is key to the approach we have laid out from taking an information-/ (data-) driven baseline to attain person-focussed care, which is centred upon personal activation (through the app).
With the phased implementation of CoW, routine functions like registration, appointment scheduling and payment can be undertaken through enablers, such as the HealthHub app. Time savings through digitalisation presents an opportunity for workforce transformation, whereby the competencies of our patient service associates (PSAs) can be enhanced to take on higher-level work like basic nursing skillsets (e.g. venepunctures and castings). Our nurses, in turn, are freed up to practise at the top of their licence, to take up roles such as nurse-led arthroplasty assessment and counselling, and Prolia intramuscular injections and counselling, which are traditionally undertaken by doctors.

Conclusion
TTSH’s digital transformation journey is complemented by the redesign of our outpatient clinic spaces to embrace a counter-less concept. Patients who arrive for their appointments are met with a neater and more aesthetically pleasing layout from the clinic entrance. Friendly PSAs are on hand to assist with registration where needed, either at the self-service e-kiosks or via the HealthHub app. After consultation, patients can make payment at Self-payment kiosks (SPKs) or via CoW’s mobile payment platform. These physical changes to our outpatient clinics collectively set the stage for our initial journey towards digitalisation of care.
Conflict of Interest
None.






