There are many people who die suddenly,
even though they had no risk factors for heart disease. It is believed that in the majority of these people the cause of
death is some type of abnormal electrical activity of the heart. When the heart
rate or rhythm becomes abnormal this is known as an arrhythmia. These
arrhythmias are known to cause sudden death. To help save lives of these
individuals, healthcare workers insert small defibrillators that recognize
arrhythmias and then send a jolt of electricity to revert the heart rhythm back
to normal. But how do doctors decide who needs this small expensive device,
which also requires a small surgical procedure?
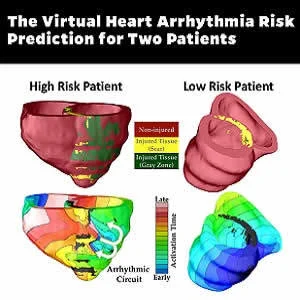
To address this issue, researchers at John Hopkins University have developed a non-invasive 3-D virtual heart assessment tool. Dubbed VARP- virtual heart arrhythmia risk predictor, this tool can help doctors determine whether a patient is at high risk for arrhythmias and who would most benefit from the defibrillator. The research team just published their initial studies in the online journal Nature. The conclusion was that this virtual heart test provided more accurate predictions on risk assessment that the current heart pump measurements used by other physicians.
According to Natalia Tranyanova, Professor of Biomedical Engineering at the University, "Our virtual heart test significantly outperformed several existing clinical metrics in predicting future arrhythmic events. This non-invasive and personalized virtual heart-risk assessment could help prevent sudden cardiac deaths and allow patients who are not at risk to avoid unnecessary defibrillator implantations."
In their study the researchers looked at data from 41 patients who had survived a heart attack and has an ejection fraction of less than 35 percent. All these patients had an implant inserted. The Hopkins team than used the preimplant MRI scans of the recipient hearts to build patient specific digital replicas of their organs. Then using computer modeling techniques they assessed the electrical processes in the heart cells. With the virtual heart, some developed arrhythmias and others did not. This method then allowed the researchers to factor in geometry of the patient's hearts, the way electrical waves moved through and the impact of scars from a previous heart attack. The VARP results were compared to the defibrillator recipients after the implant to see how the technology predicted life threatening arrhythmias.
The study revealed that patients who tested positive for arrhythmia risk with the VAPR tool were 4 times more likely to develop arrhythmia than those who tested negative.
So far the tool has only been tested in 41 patients and in a retrospective manner. Only a prospective study will determine if it is useful in detecting malignant arrhythmias and who will benefit from a defibrillator.
Source: JAMA
Image Credit: JAMA