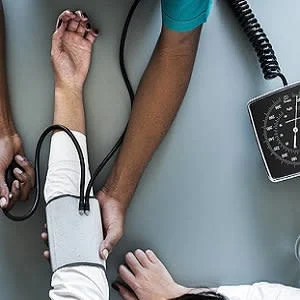
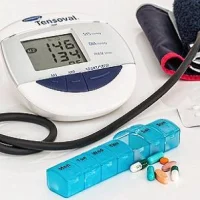
Nearly a third of American adults have high blood pressure (or hypertension) that puts them at higher risk for heart attacks, strokes, and death. While medication and diet can help lower blood pressure, it's worth noting that more than half of all Americans with hypertension don't have the condition under control.
A few integrated healthcare systems, such as Kaiser Permanente Northern California, have achieved control rates as high as 90 percent in their patients, but this approach has been considered out of reach for the many low-income and minority patients who rely on less well-resourced safety-net settings for care.
A new study, published in the journal Circulation: Cardiovascular Quality and Outcomes, demonstrates that best practices established in well-resourced clinics can work in safety-net clinics that serve high-risk populations.
UC San Francisco researchers, who led the study, collaborated with clinical leaders in the San Francisco Department of Public Health to devise a simplified intervention to improve rates of blood pressure control in the city's safety net clinics. The modified treatment programme was designed to suit the needs of the patients seen in the San Francisco Health Network (SFHN), 12 clinics run by the San Francisco Department of Public Health.
The first step was to develop an internal hypertension patient registry, in order to track blood pressure control. The tracking system was intended to benefit both the doctors monitoring their patients' health and the patients themselves, allowing appropriate outreach and reminders.
Next the team developed a treatment algorithm adapted for the SFHN. This algorithm encouraged the use of fixed-dose medications – two or more drugs in one pill – advantageous to their patients, who then require fewer trips to the pharmacy and don't have to manage as many individual pills. The researchers also adapted their algorithm to account for patients' potential social instability, which could make close monitoring required for some medications unrealistic; they took into account food insecurity and additional health conditions that could increase side effects from some of the recommended medications. To help ease the financial burden imposed on patients whose insurance might not cover certain medications, the researchers made sure to only include medications covered by the most common insurers for these patients.
The programme, dubbed "Bring it Down San Francisco", also included regular check-up visits to monitor blood pressure. Nurses and pharmacists were allowed to take standardised blood pressure measurements, allowing patients faster access to monitoring without requiring full doctor appointments. And with regular, trusted and standardised blood pressure measurements, doctors could be more proactive in adjusting medication dosages to fit their patients' needs when they did come in for appointments.
With the programme, blood pressure control rates in the city’s safety-net clinics rose from 69 percent to 74 percent over 15 months. Despite the disadvantages and difficulties faced by these clinics, the data speak for themselves, according to the study's first author Valy Fontil, MD, MAS, assistant professor of medicine at UCSF. "We didn't have a lot of funding for it, and it still worked."
If implemented across the country, the programme could potentially improve blood pressure control in vulnerable populations and, eventually, address racial and socioeconomic disparities in hypertensive-related diseases.
Image Credit: Pixabay
Latest Articles
hypertension, blood pressure control, hypertensive-related diseases
Successful interventions in hypertension control can be adapted for low-resource settings