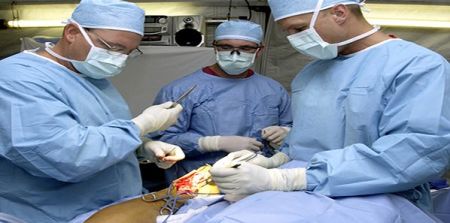
One of the most common postoperative complications seen after open heart surgeries is an infection at the surgical site. The infection can develop in the surgical wound of either the patient's sternum or leg. It is believed that surgical site infections (SSIs) affect 2 to 20% of coronary artery bypass graft (CABG) procedures and can be devastating for patients.
CABG is the most common type of open heart procedure performed in the U.S., with approximately 159,000 surgeries performed in 2013 alone. The reduction of SSI rate can provide two primary benefits: fewer postoperative complications and reduced length of hospital stay.
The Vancouver General Hospital in Vancouver, British Columbia participated in the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP). The NSQIP database is a leading nationally validated, risk-adjusted, outcomes based programme that has been designed to measure and improve the quality of surgical care provided in hospitals.
The average cardiac NSQIP SSI rate at Vancouver General Hospital was 7%, twice that of other hospitals that also participate in ACS NSQIP. That is precisely why Dr. Klein, MD, FRCP, study co-author and an anaesthesiologist at the University of British Columbia and other members of Vancouver General's cardiac surgery quality improvement team led the effort to reduce SSI reduction. Their goal was to reduce this rate to 2%. They were successful at doing so and were able to lower the infection rate to 1.6% in nine months, a dramatic 77% reduction.
The lead author of the study, Barbara A. Drake, RN, Clinical Quality and Safety Coordinator for General Hospital believes the successful reduction was primarily achieved through teamwork and through the inclusion of all healthcare disciplines that are involved in the care of cardiac surgical patients. These included surgeons, anaesthesiologist, nurse practitioners, infection control specialists, quality coordinators, pharmacist, educators, nurse leaders and staff nurses.
These reductions were also achieved by improving guidelines for prophylactic antibiotic use. The routinely administered, weight-based intravenous dose of antibiotics was given to patients at the best time and was repeated in patients during long surgical procedures. Patients also received new types of wound dressings that were especially designed to reduce the chances of infection. Patient body temperatures were normalised as soon as they were off the cardiac surgery bypass machine. This also helped reduce the chances of infection.
The SSI reduction program implemented by Vancouver General Hospital was called CLEAN, an acronym for C: Clean hands before touching the dressing, chlorhexidine wipes used on the body before surgery, clippers used for hair removal, and nasal decolonisation; L: leave the dressing on for 72 hours postoperatively, and leave the chlorhexidine disinfection or six hours after operation; E: engage patients and staff to implement best practices for maximum prevention; A: appropriate use of antibiotics; N: normothermia, normal blood glucose, nutritious meals and no smoking.
By achieving these reductions, the hospital was able to save $300,000 a year. According to Dr. Klein, "This project shows it is possible to really improve patient outcomes and obtain excellent compliance from physicians in changing clinical practice."
Source: ScienceDaily
Image Credit: Wikimedia Commons
Latest Articles
heart surgery, infection
One of the most common postoperative complications seen after open heart surgeries is an infection at the surgical site. The infection can develop in the s...