High saturated fat levels in red meat have long been known to contribute to heart disease for people in general. This time new research suggests that red meat allergy may also lead to increased risk of cardiovascular disease. Researchers say plaque levels in arteries from patients with sensitivity to red meat allergen are much higher compared to plaque buildup in patients who are not sensitised to red meat.
The study, which is supported by the U.S. National Heart, Lung, and Blood Institute, part of the National Institutes of Health, appears in Arteriosclerosis, Thrombosis, and Vascular Biology (ATVB), a peer-reviewed journal of the American Heart Association.
"This novel finding from a small group of subjects from Virginia raises the intriguing possibility that allergy to red meat may be an underrecognised factor in heart disease," said study leader Coleen McNamara, MD, a professor of medicine in the Cardiovascular Research Center of the University of Virginia Health System, Charlottesville. "These preliminary findings underscore the need for further clinical studies in larger populations from diverse geographic regions and additional laboratory work."
Only in recent years did scientists identify the main allergen in red meat, called galactose-α-1,3-galactose, or alpha-Gal, a type of complex sugar. They also found that a tick – the Lone Star tick – sensitises people to this allergen when it bites them. That is why red meat allergies tend to be more common where these ticks are more prevalent, such as the Southeastern United States, but also extending to other areas, including Long Island, New York.
While allergens can trigger certain immunological changes that might be associated with plaque buildup and artery blockages, little is known about the type of substance that is responsible for this effect. In the current study, researchers showed for the first time that a specific blood marker for red meat allergy was associated with higher levels of arterial plaque, or fatty deposits on the inner lining of the arteries. The blood marker they identified is a type of antibody (immunoglobulin or IgE) that is specific to the alpha-Gal allergen.
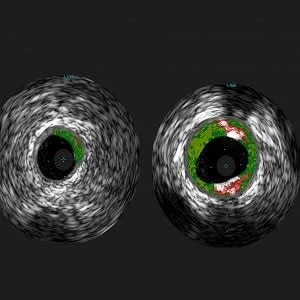
To identify this blood marker, the researchers analysed blood samples from 118 adults and detected antibodies to alpha-Gal, indicating sensitivity to red meat, in 26 percent of them. Using an imaging procedure, the researchers found that the quantity of plaque was 30 percent higher in the alpha-Gal sensitised patients than in the non-sensitised patients. These plaques, a hallmark of atherosclerosis (hardening of the arteries), also tended to be more structurally unstable, which means that they have an increased likelihood of causing heart attack and stroke.
However, as the research team noted, the evidence for a link between red meat allergens and coronary artery disease is still preliminary. The team plans to conduct detailed animal and human studies to confirm their initial findings.
Currently, the only treatment for red meat allergy once it is diagnosed is strict avoidance of red meat.
Image Credit: Angela Taylor, M.D., University of Virginia Health System
Latest Articles
heart disease, red meat, red meat allergy
Allergen in red meat linked to heart disease