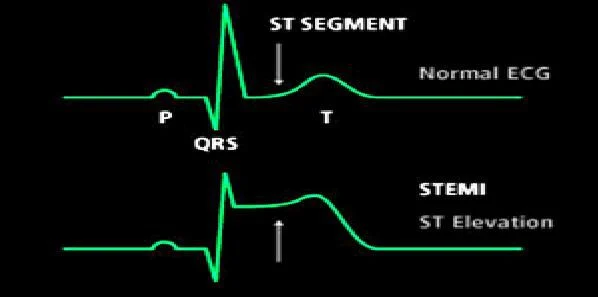
Patients who experienced a certain type of heart attack while hospitalised for conditions other than acute coronary syndromes were at greater risk of death, compared to patients brought into a hospital for treatment following a heart attack, according to results of a new study published in JAMA.
The study was conducted by Prashant Kaul, MD, of the University of North Carolina at Chapel Hill (NC, USA) and colleagues. It aimed to define the incidence, treatment and outcomes of patients who develop ST-elevation myocardial infarction (STEMI; a certain pattern on an electrocardiogram following a heart attack) during hospitalisation for non-acute coronary syndrome (ACS) conditions.
Early restoration of blood flow with percutaneous coronary intervention (PCI; a procedure such as stent placement used to open narrowed coronary arteries) or administration of medication to dissolve a clot remains the primary goal in the initial treatment of eligible patients presenting to a hospital with STEMI. During the past decade, recognition that this strategy is of critical importance has led to the development of a number of regional and national initiatives to facilitate and improve systems of care for STEMI.
These initiatives, however, have focused exclusively on patients who develop STEMI outside of a hospital setting (outpatient-onset STEMI). Very little is known about the incidence and outcomes of STEMI in patients hospitalised for non-ACS indications (inpatient-onset STEMI), the researchers pointed out.
In the study, Kaul et al. analysed data on STEMIs occurring between 2008 and 2011 as identified in the California State Inpatient Database. Dr. Kaul's team used models to evaluate associations amongst location of onset of STEMI, resource utilisation and outcomes. They identified a total of 62,021 STEMIs in 303 hospitals, of which 3,068 (4.9 percent) occurred in patients hospitalised for non-ACS conditions.
Key findings of the UNC study include:
“The question of how to improve outcomes and define optimum treatment in hospitalised patients who experience a STEMI is an area that merits more attention and concern," the UNC team noted. "Although there have been improvements in treatment times and clinical outcomes in outpatients who have onset of STEMI, few initiatives have focused on optimising care of hospitalised patients with onset of STEMI after admission.”
Source: JAMA
Image Credit: The University of Chicago
The study was conducted by Prashant Kaul, MD, of the University of North Carolina at Chapel Hill (NC, USA) and colleagues. It aimed to define the incidence, treatment and outcomes of patients who develop ST-elevation myocardial infarction (STEMI; a certain pattern on an electrocardiogram following a heart attack) during hospitalisation for non-acute coronary syndrome (ACS) conditions.
Early restoration of blood flow with percutaneous coronary intervention (PCI; a procedure such as stent placement used to open narrowed coronary arteries) or administration of medication to dissolve a clot remains the primary goal in the initial treatment of eligible patients presenting to a hospital with STEMI. During the past decade, recognition that this strategy is of critical importance has led to the development of a number of regional and national initiatives to facilitate and improve systems of care for STEMI.
These initiatives, however, have focused exclusively on patients who develop STEMI outside of a hospital setting (outpatient-onset STEMI). Very little is known about the incidence and outcomes of STEMI in patients hospitalised for non-ACS indications (inpatient-onset STEMI), the researchers pointed out.
In the study, Kaul et al. analysed data on STEMIs occurring between 2008 and 2011 as identified in the California State Inpatient Database. Dr. Kaul's team used models to evaluate associations amongst location of onset of STEMI, resource utilisation and outcomes. They identified a total of 62,021 STEMIs in 303 hospitals, of which 3,068 (4.9 percent) occurred in patients hospitalised for non-ACS conditions.
Key findings of the UNC study include:
- Patients developing inpatient-onset STEMI had more than threefold greater in-hospital mortality than those with outpatient-onset STEMI (33.6 percent vs. 9.2 percent).
- Patients with inpatient-onset STEMI were less likely to be discharged home (33.7 percent vs. 69.4 percent), and were less likely to undergo cardiac catheterisation (33.8 percent vs. 77.8 percent) or PCI (21.6 percent vs. 65 percent).
- Average length of stay (13 days vs. five days) and inpatient charges ($245,000 vs. $129,000) were higher for inpatient-onset STEMI.
- Patients with inpatient-onset STEMI were older and more frequently female.
“The question of how to improve outcomes and define optimum treatment in hospitalised patients who experience a STEMI is an area that merits more attention and concern," the UNC team noted. "Although there have been improvements in treatment times and clinical outcomes in outpatients who have onset of STEMI, few initiatives have focused on optimising care of hospitalised patients with onset of STEMI after admission.”
Source: JAMA
Image Credit: The University of Chicago
Latest Articles
STEMI, heart attack, acute coronary syndrome, myocardial infarction, percutaneous coronary intervention
Patients who experienced a certain type of heart attack while hospitalised for conditions other than acute coronary syndromes were at greater risk of death...