New Harvard-led research shows the U.S. spent nearly twice as much as other high-income countries on medical care in 2016, yet had poorer population health outcomes (e.g.,lowest life expectancy and highest infant mortality rate). The main drivers of higher healthcare costs in the U.S. are generally high prices – for salaries of physicians and nurses, pharmaceuticals, medical devices, and administration, according to the study published in JAMA.
The new findings, from Harvard T.H. Chan School of Public Health, the Harvard Global Health Institute, and the London School of Economics, suggest that common explanations as to why healthcare costs are so high – such as the notions that the U.S. has too many doctor visits, hospitalisations, procedures, and specialists, and spends too little on social services that could mitigate healthcare needs – may be wrong.
"We know that the U.S. is an outlier in healthcare costs, spending twice as much as peer nations to deliver care. This gap and the challenges it poses for American consumers, policymakers, and business leaders was a major impetus for healthcare reform in the U.S., including delivery reforms implemented as part of the Affordable Care Act," said senior author Ashish Jha, K.T. Li Professor of Global Health at Harvard Chan School and Director of the Harvard Global Health Institute (HGHI). "In addition, the reasons for these substantially higher costs have been misunderstood: These data suggest that many of the policy efforts in the U.S. have not been truly evidence-based."
The researchers analysed data from 2013-2016 comparing differences in healthcare spending, performance and structural features between the United States and 10 high-income countries (UK, Canada, Germany, Australia, Japan, Sweden, France, the Netherlands, Switzerland, and Denmark).
The study confirmed that the U.S. has substantially higher spending, worse population health outcomes, and worse access to care than other wealthy countries. For example, in 2016, the U.S. spent 17.8% of its gross domestic product on healthcare, while other countries ranged from 9.6% (Australia) to 12.4% (Switzerland). Life expectancy in the U.S. was the lowest of all 11 countries in the study, at 78.8 years; the range for other countries was 80.7-83.9 years. The proportion of the U.S. population with health insurance was 90%, lower than all the other countries, which ranged from 99%-100% coverage.
However, commonly held beliefs for these differences appear at odds with the evidence, the study found. Key findings included:
Belief: The U.S. uses more healthcare services than peer countries, thus leading to higher costs.
Evidence: The U.S. has lower rates of physician visits and days spent in the hospital than other nations.
Belief: The U.S. provides too much inpatient hospital care.
Evidence: Only 19% of total healthcare spending in the U.S. is spent on inpatient services -- among the lowest proportion of similar countries.
Belief: The U.S. spends too little on social services and this may contribute to higher healthcare costs among certain populations.
Evidence: The U.S. does spend a bit less on social services than other countries but is not an outlier.
Notably, administrative complexity and high labour costs in the U.S. also contributed to the country's higher healthcare spending. The study found that administrative costs of care – activities related to planning, regulating, and managing health systems and services – accounted for 8% of total healthcare costs, compared with a range of 1%-3% for other countries. Meanwhile, the average salary for a general practice physician in the U.S. was $218,173, while in other countries the salary range was $86,607-$154,126.
"Efforts targeting healthcare usage alone are unlikely to reduce growth in healthcare spending in the United States, and a more concerted effort to reduce prices and administrative costs is likely needed," the authors conclude.
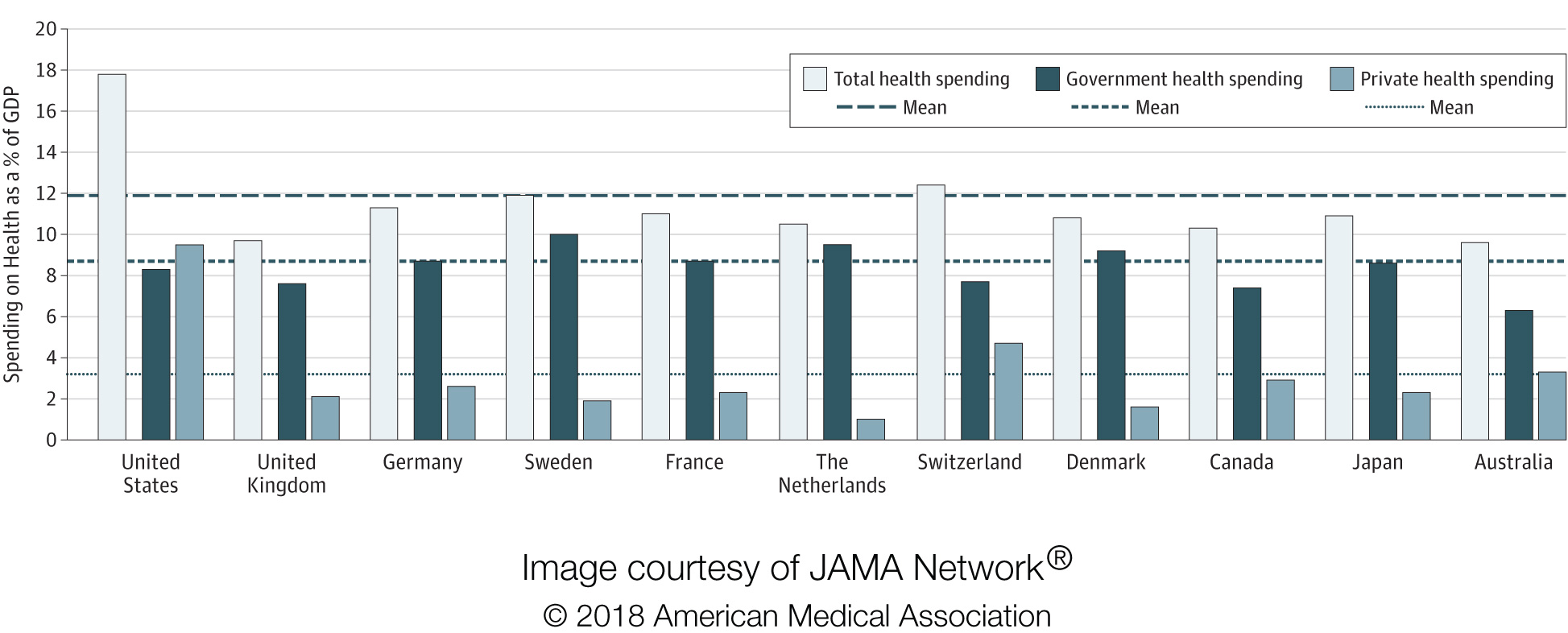
Source: JAMA
Image and video credit: JAMA
References:
Papanicolas I, Woskie LR, Jha AK (2018) Health Care Spending in the United States and Other High-Income Countries. JAMA, online March 13, 2018, doi: 10.1001/jama.2018.1150
Latest Articles
healthcare costs, life expectancy, poor outcomes, infant mortality rate
New Harvard-led research shows the U.S. spent nearly twice as much as other high-income countries on medical care in 2016, yet had poorer population health outcomes (e.g.,lowest life expectancy and highest infant mortality rate). The main drivers of highe






