HealthManagement, Volume 14, Issue 3 /2012
Paramedics found a 50 year-old man in his apartment, disheveled and with altered mental status. Mildly hypothermic and hypotensive, he was brought into the emergency room where a brief initial cardiovascular physical survey found no pulmonary rales, wheezing, cardiac gallops or murmurs. The patient was intubated for airway protection.
A three-minute cardiovascular limited ultrasound exam (CLUE) using 2D imaging of six sites was performed at the bedside using a 3MHz transducer. The parasternal long axis left ventricular cardiac view demonstrated depressed LV systolic function and mild left atrial enlargement, suggesting congestive heart failure. A “four-corner” exam (two apical and two basal views) of the lung, quickly showed bilateral ultrasonic lung comet-tail artifacts (see figure 2) and pleural effusions, consistent with pulmonary oedema and chronic heart failure.
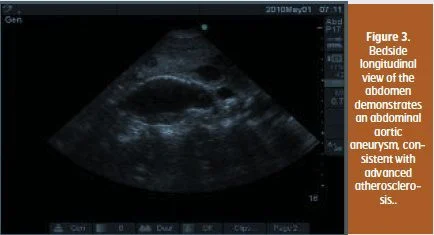
The subcostal view excluded a significant pericardial effusion indicative of tamponade, but demonstrated right ventricular enlargement, consistent with pulmonary hypertension. A midline abdominal scan showed a dilated intrahepatic inferior vena cava, suggesting ample central venous pressure and foundan abdominal aortic aneurysm consistent with advanced atherosclerosis (see figure 3).
The patient underwent head, chest, abdominal and pelvic CT scanning, which were remarkable for subdural hygromas and a 5.5cm abdominal aortic aneurysm without signs of rupture. He was admitted to the intensive care unit where a 5MHz ultrasound venous exam was used to gain jugular venous access in the neck and then exclude subsequent pneumothorax by the presence of persistent lung sliding and comet-tail artifacts. Before venous compression stockings were applied, compression of the deep veins at femoral and popliteal sites was demonstrated by using the same ultrasound transducer.




![Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging Tuberculosis Diagnostics: The Promise of [18F]FDT PET Imaging](https://res.cloudinary.com/healthmanagement-org/image/upload/c_thumb,f_auto,fl_lossy,h_184,q_90,w_500/v1721132076/cw/00127782_cw_image_wi_88cc5f34b1423cec414436d2748b40ce.webp)