HealthManagement, Volume 18 - Issue 2, 2018
In addition to user preference and image quality, the major purchasing considerations are:
- Configuration—the types of studies to be performed will dictate the capabilities, options, and features that will be needed.
- Portability—Where the scanner will be used will influence the choice of mounting options.
- User interface complexity—Who will be using the scanner will determine how easy it needs to be to use.
Once
these issues have been addressed, buyers should perform appropriate
apples-to-apples comparisons of POC scanners and negotiate pricing.
End users should perform evaluations of the scanners under
consideration to compare image quality, ease of use, and other factors.
the goal should be to choose a scanner that will best meet your facility's current clinical needs and that is most likely to address
potential future changes in use.
Configuration—What types of studies will be performed?
The specific clinical applications (ie, the types of imaging procedures the scanner will be used for) will dictate its base configuration. the configuration choices include the imaging modes available, the image display and analysis software, and the transducers. For example, a scanner configured for use in labour and delivery would need an obstetrical calculation package and a low-frequency curved linear-array transducer suitable for third-trimester pregnancies, whereas a system used for anaesthesiology applications would have software to enhance needle visualisation, plus high-frequency linear-array transducers suitable for superficial imaging.Recognising the diversity of POC ultrasound applications, some vendors offer several versions of their systems, each designed for unique clinical specialties. These specialised configurations enhance the use of the device for the given clinical application, but may present limitations if the scanner is going to have other clinical uses. If the scanner will be used for shared services, buyers should ask vendors if it can be configured for multiple applications.
The primary modes of operation include the following:
- B-mode (brightness mode) depicts anatomy as a 2-d display and is the basic imaging mode found on all ultrasound scanners.
- M-mode (motion mode) is used to assess the motion of tissues (eg, the opening and closing of heart valves) and is primarily used for cardiac assessments.
- Doppler modes enable assessment of blood flow and are available in qualitative and quantitative versions.
- Colour-flow imaging is a qualitative means to assess blood flow and comes in two versions, colour doppler imaging (CDI) and power doppler imaging (PDI). CDI displays the direction of blood flow relative to the location of the transducer, whereas PDI displays the strength of the blood flow. Both these modes are routinely utilised by many clinicians who use POC ultrasound.
- Quantitative Doppler modes are used by clinicians who need to better characterise blood flow. The quantitative Doppler modes are pulsed wave (PW) and continuous wave (CW). PW allows analysis of flow at a specific depth in the b-mode image but is subject to some limitations—most notably its inability to measure very high flow velocities. PW is used in such disciplines as rheumatology, emergency medicine, and vascular surgery. CW is used for cardiac applications and can be used to measure higher blood-flow velocities than PW can.
- Needle-enhancement mode improves the detection and display of needles and other interventional devices and is used during interventional procedures such as needle biopsies and catheter placements. We recommend that a needle-enhancement mode be included on any scanner used in interventional procedures.
As for transducers, many types are available, and their cost can range from a few thousand dollars to more than $20,000 each. therefore, it is important to buy only those transducers that are required to perform the services intended.
Transducer types include:
- Flat linear array—Primarily used to assess superficial structures (eg, the breast or thyroid) and for most vascular imaging applications.
- Curved linear array—Primarily used for obstetrical and abdominal applications.
- Sector—Primarily used for cardiac applications and some deep abdominal applications (eg, for bariatric patients).
- Endocavity—Designed to be inserted into the body. they are available in a variety of designs that include endovaginal transducers for gynaecological and early obstetrical applications, endorectal transducers for prostate applications, and transoesophageal transducers for insertion into the oesophagus for detailed cardiac assessments. Some vendors offer endocavity transducers that can be used for both endovaginal and endorectal applications, which obviates the need to buy two individual transducers.
Portability—Where will the scanner be used?
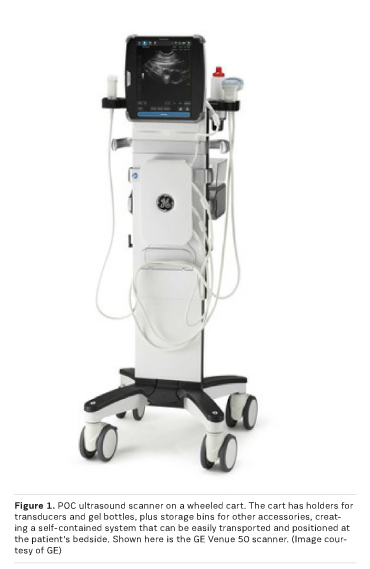
The size and weight of POC ultrasound scanners that are not designed to be handheld can make them challenging for users to hold, while performing clinical studies. Thus, vendors offer a variety of mounting options to enhance the use of the device in different clinical settings. Listed below are common mounting options for POC scanners, as well as settings where these options may be most appropriate.- Wheeled cart—Allows users to easily transport the scanner between patient rooms or to other locations within a facility (see Figure 1). Wheeled carts provide a stable platform for the scanner and include transducer and gel-bottle holders and storage for accessories. A cart also provides an easy method to adjust the position of the scanner in relation to the patient during an exam. Cart-mounted POC scanners are commonly used in emergency departments, surgical suites, and critical care units. Because use of a wheeled cart creates a self-contained system with all needed components and accessories readily at hand, it may be an attractive option even for settings that don't require the scanner to be transported (eg, private physician office).
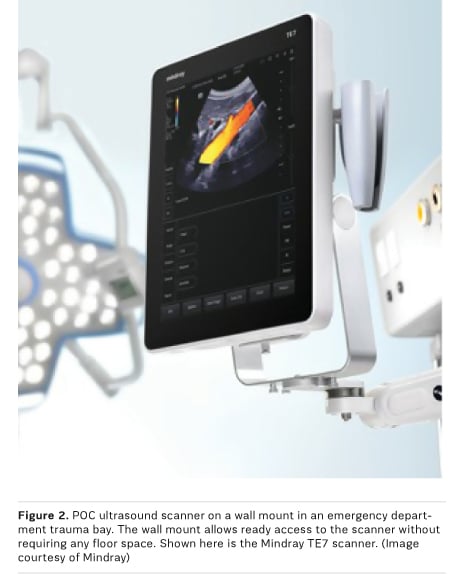
- Wall mount—Allows the scanner to be mounted to an articulating arm so that it is readily accessible for use but does not require any floor space (see Figure 2.) Thus, a wall mount may be a useful option for settings where floor space is limited (eg, small emergency department rooms, private physician offices). Wall mounts are typically limited in terms of transducer holders or storage space, so transducers and accessories must be kept in a convenient location nearby.
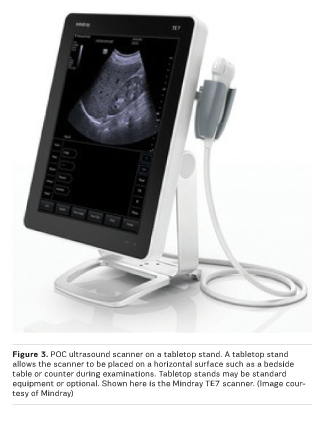
- Tabletop stand—Provides a means to place the POC scanner on an existing counter or table. Tabletop stands may have transducer and gel-bottle holders but lack storage for accessories (see Figure 3.) These stands are most appropriate for users who do not need to transport the scanner between care settings, such as those in a private physician office. Some scanners employ a kickstand or other method for keeping them upright on a table during use.
Users who frequently need to perform imaging assessments in a variety of locations within a facility should consider such aspects as battery life and the overall size of the POC system (ie, the scanner, transducers, and accessories). When the scanner is not in use, it should be kept in a location that has access to AC power receptacles to keep the scanner's battery charged. Additional care-setting considerations include device integration with existing infrastructure (eg connection to an electronic medical record [EMR] or picture archiving and communication system [PACS]), personnel access, and security.
User interface complexity—Who will be using the scanner?
Recognising that POC ultrasound is used by individuals who have a wide range of imaging skills and experience, vendors have incorporated the latest technologies—including touchscreen inter- faces and tablet-computer functionality—to make their systems easy to use. the ease of use of the scanner is related to its level of technical complexity (ie, the number of, and ease of access to, user- adjustable parameters) and its imaging capabilities (eg, modes of operation). POC scanners that possess fewer user-selectable imaging parameters and fewer imaging modes may be appealing to new or less experienced users; however, their simplicity has the potential to limit the types of data that can be acquired and the ability to optimise image quality.In addition to considering the skills and experience of the end users, buyers should recognise that those skill levels will improve over time. As users' skills improve, they may want to per form more complex assessments and use the scanner for additional applications, which may require up-grades to the scanner.
Buyers should inquire about any potential limitations of the scanner in terms of the types of transducers supported, the available modes of operation and other features, and the upgradability of the device. Scanners that can be upgraded may be a better option than models that have limited upgradability: having the flexibility to add new transducers, imaging modes, or other features to an existing scanner will likely be more cost-effective than having to purchase a completely new one should clinical demands change over time.Where practical, facilities that require multiple scanners may want to standardise on just one model or a single vendor's product line to facilitate clinician familiarity with the units and to simplify maintenance. However, we recognise that standardisation on just a single model or vendor may not be practical due to the needs of some clinical specialties.
Finalising the decision
Once
the issues described above have been ad- dressed, buyers should perform
appropriate apples- to-apples comparisons of POC scanners and negotiate pricing. When pricing scanners, buyers should consider the overall
configuration of the system, including the standard features, as well
as the additional costs of transducers, mounting hardware, and other
options. End users should perform evaluations of the scanners under
consideration to compare image quality, ease of use, and other factors.
the goal should be to choose a scanner that will best meet your
facility's current clinical needs and that is most likely to address
potential future changes in the utilisation of POC ultrasound.
ECRI Institute, a nonprofit organisation, dedicates itself to bringing the discipline of applied scientific research in healthcare to uncover the best approaches to improving patient care. As pioneers in this science for 50 years, ECRI Institute marries experience and independence with the objectivity of evidence-based research.
ECRI’s
focus is medical device technology, health- care risk and quality
management, and health technology assessment. It provides information
services and technical assistance to more than 5,000 hospitals,
healthcare organisations, ministries of health, government and planning
agencies, voluntary sector organisations and accrediting agencies
worldwide. Its databases (over 30), publications, information services
and technical assistance services set the standard for the healthcare
community.
More than 5,000 healthcare organisations worldwide rely on ECRI Institute’s expertise in patient safety improvement, risk and quality management, healthcare processes, devices, procedures and drug technology. ECRI Institute is one of only a handful of organisations to have been designated as both a Collaborating Centre of the World Health Organization and an evidence-based practice centre by the US Agency for healthcare research and quality in Europe. for more information, visit ecri.org.uk



