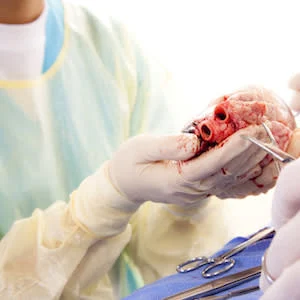
In a first-of-its-kind transplant surgery, the world’s first person received a heart transplant from a genetically modified pig. The patient, David Bennet, was too ill to qualify for a human heart. So far, he is doing well.
This could be an important medical breakthrough and could potentially shorten transplant waiting time for many patients around the world. But while many good things are being said about the achievement, there are also some concerns regarding the ethical implications of the procedure.
How ethical is a pig heart transplant? Here are three arguments by those who feel the procedure may not be right on ethical grounds:
Patient Safety
How safe is such a procedure for the patient? This is the first question that is being asked. It has been clearly stated that this was an experimental surgical procedure. Even if it is conducted with human donor organs, any transplant procedure can be risky for the patient. Often, donor organs are rejected after they are transplanted. So it is logical to wonder if human bodies can reject human organs, how would a patient with an animal organ survive? Animal organs have been used in the past but with very limited success. This is something to consider, but as far as this particular patient is concerned, both the patient and the medical team were aware of the risks and were also aware of the fact that the patient had no other treatment options and would have died without the procedure. The good thing is that the data and experience generated through this procedure can help clinicians determine if this is something that can be safely offered to other patients in the future.
Animal Abuse
Animal rights groups have also spoken out on the ethical implications of this procedure. According to the People for the Ethical Treatment of Animals (PETA), animals should be not be used in this manner, and their genes should not be modified to suit human needs. In the case of David Bennett, the genes of the pig were altered, which is not considered an ethical practice by animal support groups. They believe that animals should not be genetically manipulated and that animals also feel pain and trauma. On the other hand, some people believe that killing pigs to produce and market their meat and eating this meat is more problematic than using pig organs to save lives. This debate is unlikely to be resolved easily as both arguments have strengths and weaknesses.
Religious Implications
Finally, the never-ending issue of religion has been brought into this debate. Do all faiths allow the use of animal organs for human transplants? For example, the Muslim and Jewish faith considers the meat of pigs to be haram/kosher, but would they be open to the idea of a pig’s organ inside the body of a person who follows these religions? So far, the religious authorities from both the Jewish and Muslim communities have stated that their religion forbids them from raising or eating pigs, but receiving a pig heart is not a religious violation as such a transplant aims to preserve human life. Hence, if such a procedure can save a life, religious restrictions to eating pork do not apply here.
As these discussions continue, the most important thing that the medical community is concerned about is the patient's condition. They are more interested in how the patient fares after the transplant, whether his body accepts the organ, and whether his condition improves. That is their area of focus. Depending on the findings and results of this experimental surgery, clinicians can determine the future of animal transplants.