According to an article published in the February issue of Critical Care Nurse, extracorporeal life support is a promising treatment for paediatric patients in cardiac arrest who are unresponsive to CPR. The article examines the use of extracorporeal cardiopulmonary resuscitation (ECPR) and the ethical principles associated with its use and the advancement of end-of-life care.
“More than 50,000 patients have survived because of ECPR, and this revolutionary treatment offers hope where there was none before,” said author Jennie Ryan, MS, CPNP-AC. “However, the appropriate use of this therapy and delineated guidelines for initiating and withdrawing it have yet to be defined.”
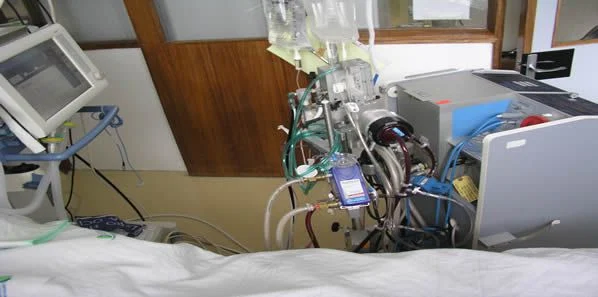
During veno-arterial ECMO, blood is drained from the right atrium. It is then oxygenated through the extracorporeal circuit and is transfused back to the body, bypassing the lungs and the heart. Using artificial oxygenation and perfusion can thus provide the body a period of haemodynamic stability and allows resolution of the underlying disease processes.
ECPR is the initiation of ECMO following cardiac arrest that has been unresponsive to conventional CPR. The transition from ECPR to ECMO occurs when the patient has been placed on the extracorporeal circuit. While neurological outcomes still require further investigation, it is evident that the survival rates for ECPR patients are higher than those for traditional cardiopulmonary resuscitation.
However, patients supported by ECMO require skilled nurses to manage their daily care. They also require frequent lab and physical assessments as well as neurological checks and daily ultrasound imaging. That is why it is important to provide adequate training to nurses in centres which are engaged in deploying the ECMO circuit as this is critical for ensuring a smooth transition from CPR to artificial circulation.
Ryan points out that ECPR is an advanced and complex treatment and requires extensive knowledge from every member of the team. She also adds that appropriate support of the patient and the patient's family is also crucial during the caring of critically ill patients. Nurses should be skilled at communicating with patients' families as they are the primary point of contact for them.
There are some ethical concerns associated with ECPR as to when it should be withdrawn. In most cases, the burden of this choice is left to the patient's caregivers.
Source: American Association of Critical Care Nurses (AAC)
Image Credit: Wikimedia Commons