According to a new study conducted by researchers at Beth Israel Deaconess Medical Center (BIDMC), endovascular aortic repair offers benefits for most patients and provides them a safe operation and quick recovery. The study is published in The New England Journal of Medicine.
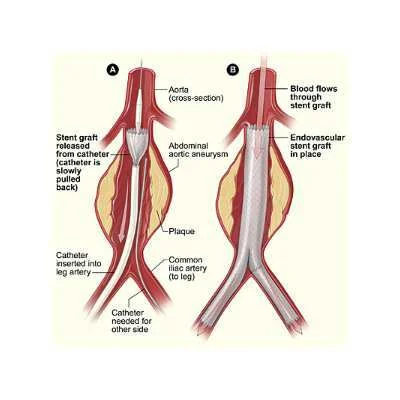
Approximately 40,000 Americans undergo elective surgery for abdominal aortic aneurysm that pose risk of life-threatening rupture and those which are typically five centimeters in diameter or larger or that are fast-growing. The condition is treated either through an open abdominal incision or through an endovascular procedure where a stent is placed inside the artery using a catheter fed through the femoral artery in the groin.
"Abdominal aortic aneurysm is common, especially among men over the age of 65 who have ever smoked and among individuals with a family history of the condition," said lead author Marc Schermerhorn, MD, Chief of Vascular Surgery at BIDMC and Associate Professor of Surgery at Harvard Medical School. "Endovascular aortic repair (EVAR) for AAA began in 1991, and over the years we've seen the number of endovascular cases steadily increase, making repair available to those who might not be healthy enough to undergo an open procedure."
During this study, the researchers examined national Medicare data from 2001-2008 involving nearly 80,000 patients who had undergone elective repair of AAA. Half of the patients had open procedures, and half had EVAR. The findings of the study showed that endovascular repair was superior to open repair for the first thirty days and continued to remain superior for the next sixty days. The benefits of endovascular repair endured for a minimum of three years. Even patients who were sicker and who underwent EVAR continued to improve and the results appear to be durable. The study also showed an early survival benefit for patients who had undergone EVAR. Mortality rate with EVAR was 1.6 percent as compared to 5.2 percent with open procedures.
Patients in the EVAR cohort had lower rates of perioperative medical and surgical complications like pneumonia as well as shorter hospital stays (an average of 3.5 days) as compared to 9.8 days in the open repair group. Patients in the EVAR group were also more likely to go home after surgery, rather than to a rehabilitation center or a nursing home. However, the findings do show that the survival advantage of EVAR decreased over time and after eight years, the survival rates for both the groups was nearly even. While interventions related to management of the aneurysm were more common after EVAR, interventions for surgical incision complications were more common after open repair.
"Importantly, aneurysm rupture occurred in 5.4 percent of EVAR patients who survived for eight years versus 1.4 percent of patients who received open repair," said Schermerhorn. "The importance of this key finding is that we need to focus our efforts at minimising this risk after EVAR. Patients need to come back for follow-up after endovascular surgery and undergo these additional interventions, if needed, to prevent late rupture."
Source: Beth Israel Deaconess Medical Center
Image Credit: Wikimedia Commons
References:
Schermerhorn, Marc L. et al. (2015) Long-Term Outcomes of Abdominal Aortic Aneurysm in the Medicare Population. New England Journal of Medicine. 373 (4): 328 DOI:10.1056/NEJMoa1405778