Strokes are a major cause of death and long-term disability globally, including in developing countries. In China, strokes are also the leading cause of morbidity and mortality, with prevalence rates having risen sharply over the past decade. Several studies have shown that the capacity to identify stroke signs, knowledge of coping with stroke symptoms, and emergency coping abilities during the pre-hospital period are major determinants of successful stroke prevention and treatment.
Other studies have demonstrated that the level of knowledge about strokes in the general population is low, which can be improved with the implementation of appropriate health education interventions. There are presently no references to methods assessing community resident knowledge regarding ways to cope with pre-hospital stroke symptoms in the scientific literature. Thus, having an instrument which would allow evaluations of such knowledge among high-risk populations and family members would be a valuable asset to healthcare providers, as it would enable them to more effectively tailor stroke education interventions to help overcome patient concerns.
This study aimed to develop and validate the Pre-hospital Stroke Symptoms Coping Test (PSSCT). The study consisted of two phases: (1) the instrument development phase and (2) the evaluation of psychometric properties phase.
Materials and Method
A total of 25 potential items were originally identified: 20 were derived from a review of the literature, monographs on stroke knowledge, and the cerebrovascular guidelines for Chinese public health education programmes on strokes; five were extracted from semi-structured interviews with stroke patients. An expert panel of 11 healthcare providers, including six doctors and five nurses from the emergency, brain surgery, and neurology departments, was invited to review the items for content, breadth, and applicability, and rate each item on its validity and relevance.
The content validity index (CVI) of each item was calculated, and six items with indexes <0.70 were subsequently deleted. The 19 items of the PSSCT were finalised after a Delphi expert consultation was conducted. The test contained three sections assessing coping with typical symptoms and symptoms associated with vomiting and twitching. Its psychometric properties were investigated in a community sample of 300 high-risk patients and family members. Eligible participants were recruited from three different communities consecutively across Harbin, China, through posters placed in community publicity columns until the required sample size was reached.
Descriptive statistics (means and standard deviations) were calculated for the continuous variables, such as descriptions of participants’ clinical-demographic characteristics. The Kuder-Richardson (KR20) coefficient was used to assess the reliability of the PSSCT. A CVI of ≥0.70 was used as the cut-off to indicate sufficient content validity. We also compared the scores of participants who had and had not experienced a stroke to determine the discriminant validity. A significance level of 0.01 was used for all statistical analyses.
Results
Five pairs of high-risk patients and their family members (n = 10) were excluded, because their knowledge of coping with pre-hospital stroke symptoms could not be evaluated due to logistical reasons. Therefore, 290 (96.7 percent) valid questionnaires were obtained. The remaining 290 participants (135 males, 155 females; mean age = 62.03 years, SD = 12.69 years) were included in the internal reliability and validity assessments. Most participants (n = 220) had not experienced a stroke, and the remaining 70 had personal experiences with stroke.
The average time taken to complete the PSSCT was approximately five minutes, suggesting that the test was readily accepted by participants. The PSSCT demonstrated adequate surface validity and content validity, and good internal consistency (KR20 = 0.822) and test-retest reliability (0.769), with difficulty (P) and degree of differentiation (D) ranges of 0.28–0.83 and 0.15–0.66, respectively.
The 19-item test was also able to distinguish between individuals who had/had not experienced a stroke. Experienced individuals scored significantly higher overall and on coping with typical symptoms and twitching (P<0.01), indicating that the PSSCT has good discriminant validity.
Conclusion
This study aimed to develop a practical 19-item instrument to evaluate knowledge of coping with pre-hospital stroke symptoms among community residents. The PSSCT demonstrated robust internal consistency reliability and validity. The findings also highlighted the importance of or necessity for community-oriented public education programmes on the subject, as many residents lacked essential coping knowledge with regard to pre-hospital stroke symptoms.
The insufficient coping knowledge of high-risk populations susceptible to stroke and their family members observed in this study presents a critical problem, but also vital clues into future directions for community health education on stroke. Furthermore, use of a standardised instrument, such as the PSSCT, would greatly facilitate cross-study comparisons.
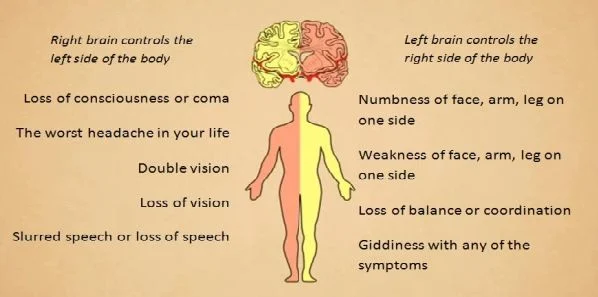
Image Credit: National Healthcare Group, Singapore
Other studies have demonstrated that the level of knowledge about strokes in the general population is low, which can be improved with the implementation of appropriate health education interventions. There are presently no references to methods assessing community resident knowledge regarding ways to cope with pre-hospital stroke symptoms in the scientific literature. Thus, having an instrument which would allow evaluations of such knowledge among high-risk populations and family members would be a valuable asset to healthcare providers, as it would enable them to more effectively tailor stroke education interventions to help overcome patient concerns.
This study aimed to develop and validate the Pre-hospital Stroke Symptoms Coping Test (PSSCT). The study consisted of two phases: (1) the instrument development phase and (2) the evaluation of psychometric properties phase.
Materials and Method
A total of 25 potential items were originally identified: 20 were derived from a review of the literature, monographs on stroke knowledge, and the cerebrovascular guidelines for Chinese public health education programmes on strokes; five were extracted from semi-structured interviews with stroke patients. An expert panel of 11 healthcare providers, including six doctors and five nurses from the emergency, brain surgery, and neurology departments, was invited to review the items for content, breadth, and applicability, and rate each item on its validity and relevance.
The content validity index (CVI) of each item was calculated, and six items with indexes <0.70 were subsequently deleted. The 19 items of the PSSCT were finalised after a Delphi expert consultation was conducted. The test contained three sections assessing coping with typical symptoms and symptoms associated with vomiting and twitching. Its psychometric properties were investigated in a community sample of 300 high-risk patients and family members. Eligible participants were recruited from three different communities consecutively across Harbin, China, through posters placed in community publicity columns until the required sample size was reached.
Descriptive statistics (means and standard deviations) were calculated for the continuous variables, such as descriptions of participants’ clinical-demographic characteristics. The Kuder-Richardson (KR20) coefficient was used to assess the reliability of the PSSCT. A CVI of ≥0.70 was used as the cut-off to indicate sufficient content validity. We also compared the scores of participants who had and had not experienced a stroke to determine the discriminant validity. A significance level of 0.01 was used for all statistical analyses.
Results
Five pairs of high-risk patients and their family members (n = 10) were excluded, because their knowledge of coping with pre-hospital stroke symptoms could not be evaluated due to logistical reasons. Therefore, 290 (96.7 percent) valid questionnaires were obtained. The remaining 290 participants (135 males, 155 females; mean age = 62.03 years, SD = 12.69 years) were included in the internal reliability and validity assessments. Most participants (n = 220) had not experienced a stroke, and the remaining 70 had personal experiences with stroke.
The average time taken to complete the PSSCT was approximately five minutes, suggesting that the test was readily accepted by participants. The PSSCT demonstrated adequate surface validity and content validity, and good internal consistency (KR20 = 0.822) and test-retest reliability (0.769), with difficulty (P) and degree of differentiation (D) ranges of 0.28–0.83 and 0.15–0.66, respectively.
The 19-item test was also able to distinguish between individuals who had/had not experienced a stroke. Experienced individuals scored significantly higher overall and on coping with typical symptoms and twitching (P<0.01), indicating that the PSSCT has good discriminant validity.
Conclusion
This study aimed to develop a practical 19-item instrument to evaluate knowledge of coping with pre-hospital stroke symptoms among community residents. The PSSCT demonstrated robust internal consistency reliability and validity. The findings also highlighted the importance of or necessity for community-oriented public education programmes on the subject, as many residents lacked essential coping knowledge with regard to pre-hospital stroke symptoms.
The insufficient coping knowledge of high-risk populations susceptible to stroke and their family members observed in this study presents a critical problem, but also vital clues into future directions for community health education on stroke. Furthermore, use of a standardised instrument, such as the PSSCT, would greatly facilitate cross-study comparisons.
Image Credit: National Healthcare Group, Singapore
References:
Zhao Q, Yang L, Zhang X, Zhu X, Zuo Q, Wu Y, Yang L, Gao W, Li M, Cheng S
(2014) Development and Validation of the Pre-Hospital Stroke Symptoms
Coping Test. PLoS One. 2014; 9(10): e110022. PMCID: PMC4201517
Latest Articles
Stroke, cerebrovascular, health education, psychometric
Strokes are a major cause of death and long-term disability globally, including in developing countries. In China, strokes are also the leading cause of mo...