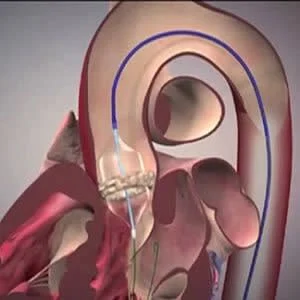
Transcatheter aortic valve replacement (TAVR) is widely used to treat aortic stenosis. The treatment approach is approved by the FDA and is recommended in patients with severe symptomatic aortic stenosis and intermediate surgical risk. However, post-TAVR stroke remains a serious complication and is associated with increased mortality. While the number of TAVR procedures have been consistently increasing in clinical practice, it is still unknown whether stroke risk after TAVR has declined in clinical practice.
This study was conducted to evaluate the trends and prognosis of an early stroke occurring within 30 days of TAVR procedure. 101430 patients treated with TAVR were included in the study. Primary parameters that were assessed included the rates of 30-day stroke, transient ischaemic attack (TIA), and any neurologic event (stroke or TIA).
Findings show that at day 30, there were 373 patients with TIA and 2290 patients with stroke. There was no difference in the 30-day stroke rate between sites with fewer than 100 TAVR cases or more than 100 TAVR cases. It was also observed that patients with 30-day strokes were older and mostly women. Also, patients with 30-day stroke had a higher proportion of prior stroke, prior TIA, and known peripheral arterial disease, hypertension, porcelain aorta, and carotid stenosis. There was no significant difference in the rate of prior AF between patients with and without 30-day strokes. In addition, patients with stroke within 30 days were less likely to be treated with femoral access and had a higher 30-day mortality risk score. General anaesthesia and self-expanding TAVR devices were more prevalent in the 30-day stroke group, and in-hospital AF after TAVR also occurred more frequently in this group.
Both 30-day TIA and stroke rates were stable over time, and there was no significant increasing or decreasing trend. The median time to stroke events was 2.0 days after TAVR. Of the patients in the 30-day stroke group, 48.9% had a stroke within 1 day and 68.4% within 3 days. 91.5% of stroke patients had ischaemic strokes, and 5.6% had haemorrhagic strokes. 3.6% had strokes of an underdetermined subtype.
The rate of 30-day mortality was significantly higher among patients with 30-day strokes compared to those without. Also, among patients who survived to hospital discharge, those with 30-day stroke were less likely to be discharged directly home following TAVR vs. those without strokes.
Overall, these findings demonstrate that the rate of post-TAVR 30-day stroke was stable over time. The majority of early post-TAVR strokes occurred within the first 3 days following the TAVR procedure. Early stroke was independently associated with increased 30-day mortality. Neither dual antiplatelet therapy nor oral anticoagulant therapy was associated with the risk of 30-day neurologic events. However, it is evident that advances in TAVR technology and operator experience has not translated into lower early stroke rates. There is a need for additional strategies to improve the neurologic safety of TAVR.
Source: JAMA
Image Credit: Lee Health
References:
Huded CP et al. (2019) Association Between Transcatheter Aortic Valve Replacement and Early Postprocedural Stroke. JAMA, 321(23):2306-2315.
Latest Articles
Stroke, TAVR, transcatheter aortic valve implantation
This study was conducted to evaluate the trends and prognosis of an early stroke occurring within 30 days of TAVR procedure.