Researchers in France have developed a new scoring system, based on thoracic aortic calcification (TAC), to predict one-year cardiovascular and all-cause mortality after transcatheter aortic valve replacement (TAVR). The predictive performance of Calcification Prognostic Impact (CAPRI) score was confirmed in an independent contemporary cohort, according to a study published online in JACC: Cardiovascular Imaging.
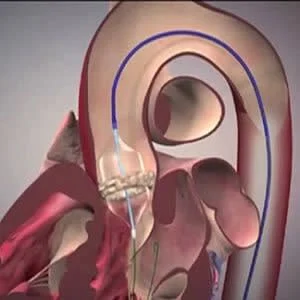
TAVR has become a standard treatment for patients with aortic stenosis at prohibitive, high, and intermediate risk for surgical aortic valve replacement. Many predictive risk models have been used to help identify patients who will benefit from the procedure. All of these risk prediction models are for in-hospital or 30-day mortality post-procedure.
Notably, for TAVR, the 30-day procedural mortality has decreased significantly now approaching 1 percent in clinical trials and less than 4 percent in clinical practice. As such, the focus of clinicians is now appropriately shifting toward identification of those patients who despite undergoing a successful procedure do not receive benefit from the correction of their aortic stenosis (AS).
The CAPRI score, developed by Pierre Lantelme, MD, PhD and colleagues, is based on four domains: thoracic aortic calcification (TAC), patient demographics and comorbidities, atherosclerotic disease, and cardiac function. The components of the latter three domains are patient demographics (age, sex, and renal and lung function), atherosclerotic disease (coronary artery and peripheral vascular disease, history of stroke), and cardiac function (ejection fraction, New York Heart Association functional class, pulmonary artery pressures, aortic valve gradient, and mitral regurgitation severity).
The predictive risk model was derived from 1,425 patients treated between 2010 and 2014 as a derivation cohort and validated in 311 patients treated with TAVR in 2015. Cardiovascular and all-cause mortality at one year was 13.0 percent and 17.9 percent, respectively, in the training cohort and 8.2 percent and 11.8 percent in the test cohort.
According to the journal study, patients with a CAPRI score above 0.70 and 0.78 for cardiovascular and all-cause mortality have a 50 percent chance of dying within the first year after TAVR. If a patient has a score under that threshold, the one-year mortality is <10 percent.
In a linked commentary, Michael Mack, MD, Mohanad Hamandi, MD, and Ambarish Gopal, MD, all from Baylor Scott & White Health, Heart Hospital Baylor Plano (Dallas, TX), say that TAC may provide an objective, reproducible, and potentially widely available tool that can help as a decision aid to define "poor responders" to TAVR at one year.
"Adding TAC to the more conventional predictors contained in the CAPRI can potentially identify with greater certainty poor TAVR responders who are likely to not benefit from the procedure," the commentators say. In addition, TAC was obtained from computed tomography scans, which are routinely performed before TAVR not requiring additional testing.
Therefore, the CAPRI score should be regarded as an objective tool to help the heart team make a decision on therapy and to inform the patient and family. "Defining the futile patient who will not benefit from therapy is a critical goal as the treatment of AS progresses and matures," the commentators say.
Source: JACC: Cardiovascular Imaging
Image Credit: Lee Health
References:
Mack M, Hamandi M, Gopal A (2018) TAC for TAVR: What Is the Score?. JACC: Cardiovascular Imaging, Article in Press; Available online 16 May 2018.
https://doi.org/10.1016/j.jcmg.2018.04.007
Latest Articles
transcatheter aortic valve replacement, Aortic calcification, post-TAVR mortality, thoracic aortic calcification
Researchers in France have developed a new scoring system, based on thoracic aortic calcification (TAC), to predict one-year cardiovascular and all-cause mortality after transcatheter aortic valve replacement (TAVR). The predictive performance of Calcific