Digital breast tomosynthesis (DBT) has outperformed digital mammography (DM) over a five-year period, according to a new study published in Radiology.
The review, which was conducted at the University of Pennsylvania in Philadelphia, identified that DBT screening was responsible for detecting a higher proportion of poor prognosis cancers than DM, as well as providing increased cancer detection rates and fewer false positive findings.
You might also like:Stand-alone Tomosynthesis Breast Cancer Screening Paper Wins EUSOBI Award
Of course, previous studies on the advantages of DBT have tended to align with these results; as well as improved cancer detection, there has also been a reduction in recall rates for women when using this technique. However, the Philadelphia team was keen to scrutinise these findings over an extended period – an area in which little previous research exists.
Key Findings
Focusing on the outcomes of patient screenings over a five-year timescale, the researchers looked at more than 56,000 DBT exams from 2011 onwards, alongside 10,500 DM exams prior to this period. They then compared these findings with results from a variety of local cancer registries.
The outcomes were positive. DBT cancer detection rates were 6 per 1,000, compared to 5.1 per 1,000 for DM, while DBT screening recall rates also compared favourably at 8% to DM’s 10.4%. Around a third of DBT-detected cancers were associated with poor prognosis, while DM was linked with a quarter of those found. All of these figures remained stable across the five-year DBT screening period.
Dr Emily Conant, the study’s lead author, was excited by the findings. “We showed that the improved performance with DBT was maintained over multiple years,” she said. “This is the longest follow-up with cancer registry matching that has been published thus far.”
Dr Conant also highlighted the benefits of having access to a diverse patient population, citing the example of more aggressive breast cancer subtypes developing in African-American women.
“We found different types of biology in the cancers detected across our diverse population and that’s an important takeaway of this paper,” she said.
Why Does DBT Perform Better?
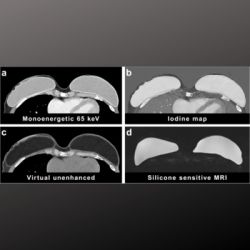
DBT – also sometimes referred to as 3D mammography – has emerged over the last decade as an important development in screening for breast cancer. It involves the insertion of a flexible, low-radiation X-ray tube that takes projections of the breast from a wide variety of angles.
This allows radiologists to view the breast in layers, or slices, enabling them to build a clearer picture. “With tomosynthesis you can remove some of the overlapping or obscuring breast tissue, so that both normal and abnormal findings are better seen,” added Dr Conant. “That provides both improved cancer detection and decreased false positives.”
In the meantime, Dr Conant and her team hope that their study can serve as a springboard for further research, ideally with more diverse populations and a longer timescale. “This is very promising and important data,” she concluded, “that can certainly be used to model larger trials.”
Source: EurekaAlert
Image credit: Pixabay