Researchers Found That the Combination of Two SedLine Parameters, Patient State Index (PSi) and Suppression Ratio (SR), Had High Predictability for Mortality 180 Days After Cardiac Arrest
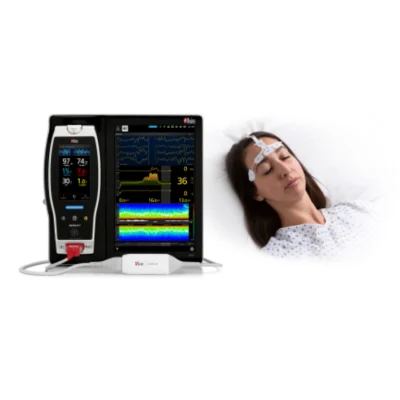
Masimo announced today the findings of a study published in the Journal of Critical Carein which Dr. Tae Youn Kim and colleagues at the Dongguk University College of Medicine and Yonsei University College of Medicine in Korea evaluated the ability of two parameters provided by Masimo SedLine® brain function monitoring to predict neurological outcomes and long-term survival in post-cardiac arrest ICU patients.1 The researchers found that the combination of the two parameters, Patient State Index (PSi) and Suppression Ratio (SR) had “high predictability” for mortality 180 days after cardiac arrest.
This press release features multimedia. View the full release here: https://www.businesswire.com/news/home/20210705005314/en/
Noting that “accurate prognostication” in post-cardiac arrest patients is important to determine treatment plans and “whether to continue or withdraw intensive care,” and that a “multi-modal” approach is recommended because “no single prognostic factor has been shown to have higher prognostic accuracy than those of other factors,” the researchers sought to evaluate the prognostic accuracy of the two Masimo SedLine parameters as predictors of neurological outcomes, both alone and in combination. The researchers chose PSi because, as they note, raw EEG data can be “difficult to use” and PSi, which is derived from EEG, is widely used in anesthesiology for determining the degree of procedural sedation, “significantly co-varies with changes in the state” under general anesthesia, and “can significantly predict” the level of arousal in varying stages of anesthetic delivery. The researchers chose SR because it helps to estimate the percentage of EEG suppression and is therefore considered a good predictor of poor neurologic outcomes.2
They enrolled 103 adult patients between January 2017 and August 2020 who experienced a non-traumatic out-of-hospital cardiac arrest, had been successfully resuscitated after CPR, and received targeted temperature management during their ICU stay. PSi and SR were continuously monitored using Masimo SedLine from immediately after ICU admission until 24 hours after return of spontaneous circulation (ROSC), recorded at one hour intervals. Neurological outcomes were categorized using the Pittsburgh Brain Stem Score (PBSS) and Cerebral Performance Category (CPC). Data on survival at 180 days was obtained via telephonic interviews.
The researchers found that using either PSi or SR alone had “good predictability” for poor neurological outcome, and that the combination of low PSi and SR had “high predictability” for mortality 180 days after cardiac arrest. They used receiver operating characteristic (ROC) curves to determine that “a mean PSI ≤ 14.53 and mean SR > 36.6 showed high diagnostic accuracy” as single prognostic factors for patients in their study. Furthermore, “Multimodal prediction using the mean PSi and mean SR showed the highest area-under-the-curve value of 0.965 (95% confidence interval 0.909–0.991).” In the study cohort, patients with mean PSi ≤ 14.53 and mean SR > 36.6 had “relatively higher long-term mortality rates” (69% died in the group) than those of patients with values > 14.53 and ≤ 36.6 (11% died in the group).
The researchers concluded that “PSi and SR are good predictors for early neuro-prognostication in post-cardiac arrest patients.” They also noted, “The combination of PSI and SR showed better predictability of poor neurologic outcome than did each individual parameter.”
References
Kim TY, Hwang SO, Jung WJ, et al. Early neuroprognostication with the Patient State Index and suppression ratio in post-cardiac arrest patients. J Crit Care. 2018. https://doi.org/10.1016/j.jcrc.2020.06.003.Seder DB, Fraser GL, Robbins T, Libby L, Riker RR. The bispectral index and suppression ratio are very early predictors of neurological outcome during therapeutic hypothermia after cardiac arrest. Intensive Care Med 2010;36(2):281-8.
Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr.2011 Feb;100(2):188-92.
de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ.2009;Jan 8;338.
Taenzer A et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
McGrath S et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
McGrath S et al. Inpatient Respiratory Arrest Associated With Sedative and Analgesic Medications: Impact of Continuous Monitoring on Patient Mortality and Severe Morbidity. J Patient Saf. 2020 14 Mar. DOI: 10.1097/PTS.0000000000000696.
Estimate: Masimo data on file.