It appears that the CMS is trying to recoup money from $11 billion worth of overpayments. It claims that this occurred due to coding changes for inpatient hospital stays that were not aligned with real changes in hospitals' patient mixes. In the past, the Medicare Access and CHIP Reauthorization Act
(MACRA) allowed for a 0.8% payment reduction each year to pay back these
funds, but as of 2017, this has now been increased to 1.5%.
The new rule also has provisions related to pay cuts due to excess readmissions. These payment reductions will now be based on a hospital's risk-adjusted admission rate during a three-year-period for specific conditions including heart attack, heart failure, pneumonia, chronic obstructive pulmonary disease, total hip/knee arthroplasty and coronary artery bypass graft. The payment methodology for readmissions due to coronary artery bypass grafts is also being revised.
There will an additional payment cut for disproportionate share hospitals (DSH) that serve low-income patients since a large number of these patients are uninsured. As of 2017, DSHs will receive 25% of the payments they would generally receive under the current formula. The remaining 75% will be used as payments for uncompensated care. This will decrease payments by approximately 0.6% next year.
Some other payment-related provisions include:
- the two-midnight rule where CMS will remove the 0.2% payment reduction for hospital stays under the two-midnight rule and will provide a one-time payment increase to account for previous losses.
- the formula for calculating DSH payments will change from dual-eligible Medicare/Medicaid, Medicaid and disabled patients to actual data reported by hospitals. This will be done after implementing additional quality-control measures.
Overall, with these changes, it seems that individual hospitals may fare better or worse depending upon their penalties and payments under the revamped meaningful use programme, the readmissions reduction programme and other initiatives. The rule also finalises quality reporting requirements for 2017 which will also affect payments in 2019 and 2020 and will also implement the Medicare Outpatient Observation Notice (MOON) for patients receiving observation services.
Source: Federal Register
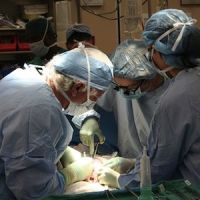
Image Credit: Wikimedia Commons
Latest Articles
CMS, two-midnight rule, pay cut
The Centers for Medicare & Medicaid Services (CMS) has just released the final rule for next year’s inpatient payment system, and there are several changes that’ll affect your hospital’s reimbursement – including a pending pay cut.